The whole country will move into a new Covid response framework on Friday. How that will play out, experts agree, is extremely difficult to predict and will depend on multiple factors. Derek Cheng takes a deep dive into what they are, and why there are reasons to feel both optimistic
Traffic light system: A new era for the Covid 19 Delta response - Why there are reasons for both optimism and dread

Subscribe to listen
The first crux is how the virus will spread after December 3, when the whole country moves into the traffic light system, but the Auckland boundary remains.
Cases outside Auckland have so far been contained, and it would likely take something unexpected to change this because vaccination coverage (currently at 85 per cent double-dosed for those aged 12 and up) continues to increase, and traffic light settings Red and Orange are more restrictive than alert level 2.
The bigger crux is what will happen once restricted travel in and out of Auckland begins from December 15, and then potentially unrestricted travel from January 17 - including MIQ-free Kiwis from Australia.
There are a lot of nerves surrounding how far and wide the virus will spread, and whether enough has been done to protect our most vulnerable - Māori in particular, as well as those with mental health and addiction issues.
But there are several more crunch points: Will case management ensure suitable treatment for people, either at home, in MIQ, or in hospital? Will contact tracers be able to stay ahead of outbreaks as they pop up? How will the Government use the public health levers of the new system, and how effective will they be?
It could be potentially disastrous if the response falters at any of these points.
But there are also reasons for optimism, which could see New Zealand coming through the summer period having avoided the tragic outcomes that most of the rest of the world have suffered, and continue to suffer.
"There's a big range of potential outcomes," says Covid-19 modeller Professor Shaun Hendy.
"A lot will depend on how aggressive the Government is with the traffic light settings."
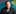
Peak immunity, booster shots, and approaching summer
Hendy says Auckland, where the outbreak has plateaued, will "likely see numbers tracking up again" after December 3.
Some Aucklanders may continue to stay home as a precaution, but others will return to work, or welcome the bursting of household bubbles by celebrating the end of more than 100 days in lockdown.
The traffic light system has measures to minimise transmission through vaccine passes, but they can't really be enforced in people's homes.
"A lot of it depends on how people who aren't vaccinated behave," says Hendy, especially as gathering size limits that include the unvaccinated have now been extended from 10 to 25.
"They may not be going to restaurants, but they may all be having dinner parties or other social activities that might just concentrate it in ways that are really unhelpful."
If the outbreak does indeed start growing again, the risk of the virus spreading around the country will also grow from December 15.
This will be mitigated by travellers needing to be fully vaccinated or to have a negative test, but there will be so many travellers that the virus will inevitably be transported from Auckland.
It may appear in a place and hit a highly vaccinated wall, and fizzle out. Finding a foothold in areas with lower vaccination coverage will be easier, which tend to be more rural, socially-deprived areas far away from health services.
"I think we will see some tragedies over the summer where the vaccine is taken by people from Auckland to different corners in New Zealand, where it will infect family and friends at social gatherings," says epidemiologist Professor Michael Baker.
"There will be people, mainly unvaccinated, who get very sick. Some will die, some will get rushed to hospital, but maybe not on a huge scale."
Middle-aged deaths may be the most common, he said, because coverage among 65s and older is very high (94.4 per cent, and among Maori 91.6 per cent); of the three deaths this week, two were in their 50s, and one in their 40s.
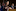
Other reasons for optimism - alongside high coverage of older people - include peak immunity, or close to it, for the vast bulk of the vaccinated population who were jabbed in recent months.
Another is the booster programme, starting on Monday, for those who had their first jab more than six months ago.
"How much a booster shot can reverse the waning is one of the most positive possibilities we face going forward," says Otago University Professor and specialist public health physician Philip Hill.
"We thought Delta was somehow more capable of overcoming vaccine protection against infection and transmission in its own right, but it looks like quite a lot of that was probably due to waning."
And summer is approaching, which will entice people outdoors. It also means fewer people in workplaces, at least for the Christmas and New Year period.
Median scenario - thousands of weekly cases, dozens in hospital
A model by Hendy's team estimates a worst-case scenario of 16,000 cases a week nationwide, with 800 needing hospitalisation and up to 80 needing ICU care.
This is unlikely to transpire, Hendy adds, unless the Government and the public throw all caution to the wind.
Prime Minister Jacinda Ardern has already said no part of the country will start in Green, Auckland and regions with low vaccination coverage will be in Red, and other regions will be set in a way where yo-yoing between colours is minimised.
The median estimate is 1800 cases a week, 90 of whom would need hospital care and up to nine needing ICU care.
One area experts are watching closely is schools, where outbreaks have driven transmission around the world, including in the UK and Victoria. Children are less likely to get sick from the virus, but they still can, and they can infect people they live with - especially the unvaccinated.
So far in the outbreak there have been 42 children under 12 in hospital, with 19 of them spending at least 24 hours there including 12 babies younger than 1.
And among active cases in New Zealand, 36 per cent are under age 20 and 19 per cent are under age 10.
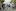
"They can play quite a significant role in driving transmission. That's something that's going to continue to be an issue perhaps until we decide to vaccinate people under 12," says Hendy.
With only a few weeks of the term left, keeping case numbers low in schools could be critical.
"We're about to go into the summer holidays, so if we manage that, it could be a lucky escape for us," Hendy says.
It would be even better, he adds, if children under 12 could be vaccinated before the 2022 school term starts.
Government safety levers and 'postcode lottery' services
Ardern has learned the lessons of Europe, where countries with high vaccination rates dropped all public health measures, only to reintroduce them later when the virus surged again.
Chief among the measures in the traffic light system is the separation of the vaccinated and unvaccinated in higher risk settings including bars, clubs and events.
A question mark remains, however, over how effective this will be because there is no requirement for businesses to use the Government's vaccine pass verifier.
Business owners only need to sight someone's pass rather than actually scanning it, which digital experts say will defeat the purpose of having it.
"It's hugely frustrating to see the key purpose and functionality of the pass being eroded," University of Auckland research fellow Dr Andrew Chen said on Twitter.
"After all the effort to make a functioning system, to educate the public on how it works, to integrate it into our Covid defences, it would be no better than a pinky promise,"
The Government has given itself some wiggle room in saying it could, at some point, make the use of the verifier less voluntary.
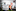
If the spread around the country mirrors what happened in Auckland, it would creep into more deprived and marginalised communities.
Māori vaccination coverage of the eligible population has ramped up in recent months, but still remains well behind the national average (66 per cent versus 85 per cent), with an even larger gap for ages 12 to 34.
Leaders in regions where such communities are more prevalent - including Northland, Tairāwhiti, and parts of the Bay of Plenty - are already telling tourists to stay away for summer.
Then there's the even lower coverage among those with mental health or addiction issues - groups that the virus invaded in Auckland and Waikato.
For those receiving mental health treatment, the range across DHB regions is from 57 (in Hawke's Bay) to 80 per cent (Auckland) double-dosed coverage, according to data platform Tūtohi; for Māori, it is 46 (Bay of Plenty) to 68 per cent (Auckland).
For those supported by addiction services, the range is 40 (West Coast) to 67 per cent; for Māori, it is 25 per cent (West Coast) to 58 per cent.

"Unfortunately, we've faced that postcode lottery with each DHB doing it in slightly different ways," says Philippa Jones, national operations manager of the Needle Exchange Programme.
"It's been quite hard to get the vaccinations to come to us, which is what's needed if we want to get our clients vaccinated."
The NEP has been able to offer vaccinations at its static outlets in Christchurch, Palmerston North, Hamilton, and in places near to its Auckland and Dunedin outlets.
"We've just got to keep helping as many of our clients as possible to make informed decisions about vaccinations."
Reactionary, rather than proactive or pro-equity
If an outbreak gets a foothold, a localised lockdown and vaccination surge could quickly bring it under control.
But this is also reactionary. Rather than chasing outbreaks, measures could be put in place to protect those communities in advance of any virus creeping in.
The Government has arguably been doing this with its $120 million rollout to boost Māori vaccination coverage, including $60m to "support Māori and iwi-led initiatives to protect their communities against Covid-19".
But health experts question whether it's enough, given how many of the unvaccinated will now need multiple conversations to be convinced.
"It's possible to have a more proactive investment and resourcing approach to protect Māori communities, and I don't see it happening," says National Māori Pandemic Group co-leader Rawiri Jansen.
"To take that even further, it's actually possible to imagine a pro-equity response, because the families where the virus is travelling are more likely to be in overcrowded, transitional housing, exposed to a lot of risks.
"We have to address housing issues, employment, income issues. We don't see that happening. It should happen."
Baker says all infectious diseases thrive where inequity and deprivation are present.
"We have the knowledge. We have the tools. There's really no excuses. It's about delivery, commitment and strategy to deliver all these tools in the most equitable way."
Hendy agrees that the Government can, and should, do more.
"Everybody's wellbeing depends on everybody else's. This is a real wake-up call. The fact we've left this group behind is potentially going to cause the whole country significant problems over the next few months and next year."
This was also addressed in a September report by the independent continuous improvement group led by Sir Brian Roche: "There is a gap in addressing the impacts on Māori and Pasifika. To begin to address the impacts on these populations, analysis
of the economic impacts of not investing in equity needs to be incorporated into planning."
Case management at home - lessons learned?
In a highly vaccinated population, most Covid cases will have mild or no symptoms and will isolate at home, keeping MIQ and hospitals wards freer for more complex cases.
"They can be managed very safely, very effectively with very little intervention, apart from having some central oversight and a point of contact if there's any problem," says Dr Bryan Betty, medical director of the Royal College of General Practitioners.
"However, there's a group of patients who may have comorbidities or other risk factors - you actually need to monitor them reasonably closely."
Health Minister Andrew Little has already conceded that home isolation didn't get off to the best start.
There was an initial underestimate of the number of cases there would be, and then many weren't contacted quickly enough because it was left to over-worked and under-resourced Public Health units.
Three people have died while in home isolation, with the Coroner looking into how their care was managed.
On Thursday Little unveiled an upgraded model, with primary care playing a key role in the initial clinical assessment of home-isolating cases, followed by a social needs assessment, and then ongoing clinical monitoring.
Involving GPs made "eminent sense", Betty says, given their rapport with patients and knowledge of their history - but not everyone has equal access to primary care.
"Some practices will be very involved, and in other localities are very short of general practice and GPs," he says.
"There may be groups of practices coming together to provide care in other localities in combination with the DHB."
About 1500 cases are already isolating at home in Auckland, and this number will balloon if there are outbreaks all over the country.
Betty said the Government should have been planning the home isolation model six months ago.
"And GPs should have been involved so by the time it happened - it was going to happen at some point - we were prepared for it."
The Government has also copped criticism for not doing more to increase ICU capacity, and its strategy - to train non-ICU nurses to step in as needed - as been described by health professionals as inadequate.
Little has said that each hospital will need to be able to care for Covid patients isolating from non-Covid patients, and some will have to cover other parts of the region where hospital reach is thin.
Expanding contact-tracing capacity - but by how much?
One of the biggest question marks hangs over contact-tracing capacity.
The Ministry of Health used to release regular contact-tracing metrics that were developed by Dr Ayesha Verrall before she became a Cabinet Minister, but none have been released since June despite Official Information Act requests and intervention from the Ombudsman.
The first few weeks of the Delta outbreak saw the system struggling to cope with 80 cases a day, and hundreds of staff were urgently trained.
At the time, the ministry's capacity was meant to be for up to 1000 cases a day - but this was never stress-tested, and it failed the real-world test.
There have also been a decent proportion of contacts a day still awaiting a call to check if they're being tested and are isolating, which has been a blind spot for Cabinet ministers when making alert level decisions earlier in the outbreak.
"Anyone who is a contact of a case and will need to self-isolate and/or get a test, they need to know that as soon as possible, preferably within five days or so of their first exposure - and with Delta probably four days," says Professor Philip Hill.
"At least 80 per cent of contacts need to know within five or even four days, and if the system can't perform at that level, it is simply not good enough."
That blind spot shrank in September when daily case numbers dropped to as low as single digits, and fewer than 10 per cent of active contacts were yet to be reached by contact-tracers.
But it climbed to more than 20 per cent by the second week of October as case numbers rose, and on Thursday 33 per cent of active contacts - or 2104 out of 6311 contacts - were still yet to be contacted.
Hill highlights three areas in particular where contact-tracing will be critical: quickly ringfencing a newly detected outbreak, pushing an existing one towards zero when cases are reduced to low numbers, and turbo-boosting containment whenever the Government looks to shift from Red to Orange or Orange to Green.
He has said in his previous report, with Dr Debbie Ryan, that capacity needed to be clarified and agreed with the minister, and then established.
If the ministry has done that, it isn't saying so.

The most specific answer director general of health Ashley Bloomfield has said recently is "hundreds" of cases a day, adding that capacity is being expanded and will be used in a targeted way.
That means, according to Hendy, sending resources to where they're most needed, such as complex cases who live in overcrowded housing.
"Well-off Pākehā people like myself, we can be left a bit more to our own devices, we've got larger homes, we're not living with large numbers of people, we've got financial resources so we don't have to go to work," Hendy says.
"We need to get really better at using more scalable approaches that rely on using the app, for example, for a large number of cases. There is work going on into that. That's going to be crucial for the coming year."
The ministry has also been criticised for taking so long to include rapid antigen testing (RAT) into its testing arsenal.
Roche's September report said that the backlogs at testing stations at the start of the outbreak – when people waited up to 12 hours in line – ended up "compromising early outbreak containment".
On Thursday, the Government announced that businesses will be able to use RAT from authorised suppliers from Wednesday next week, and the general public will be able to buy them from pharmacies from December 15.
It also plans to boost daily testing capacity from 16,000 to 60,000 a day.
Team of five million?
The effectiveness of the traffic light system in keeping Kiwis safe over summer - like the alert level system before it - will rely on social cohesion and public buy-in.
But a recent Newshub poll found 65 per cent of respondents - when asked if they fully understood the traffic light system - said "no".
Says Hendy: "We've got a lot of learning to do, and it will be challenging. This new system is going to rely on individual responsibility, so hopefully we get our heads around that as we hit Christmas, and we can all do our bit."
Baker dreads the worst, but remains hopeful.
"At the end of summer, I want for people to say, 'Nothing happened, you were wrong, you were a prophet of doom.' That would mean that the public health measures and the vaccinations have worked."
And as epidemiologist Sir David Skegg has previously noted, there will also be a player that we have no control over: luck.
