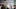A cataract clouded Mavis Hall's vision so badly that she gave up driving, then broke her wrist tripping on a step.
Her sight could easily be restored through surgery that takes 20 minutes and would remove the clouded lens inside her right eye.
Hall's optometrist had applied several times to Counties Manukau DHB, but she was deemed below the threshold for surgery.
"He was disgusted," Hall recalls of her optometrist's reaction. "He couldn't understand why. He said, 'This is not right, and I've had so many other people like you.'"
After one assessment a DHB ophthalmologist explained there'd be no surgery, she says - and then offered his details if she went private. The approximate cost, $4000, was beyond them.
Hall, 82, stopped driving as her vision worsened, despite being the main driver after her husband Douglas' knee replacement.
Her world appeared as if through frosted glass. Favourite pastimes including reading and crosswords became difficult. When walking, Hall turned her head to use her good eye to spot obstacles.
"It got to the stage where I actually tripped over and had a head injury and chipped a bone in my wrist. I was doing all sorts of tripping over and knocking things, it was pretty bad," Hall says.
"It really took everything out of me. I was too nervous to do anything."
Postcode healthcare
Like other Kiwis, the Halls have given to the Fred Hollows Foundation, a charity that treats eye conditions in the Pacific.
The accompanying stories are powerful: patches removed from the restored eyes of people who lived with blindness for years, when a straightforward 20-minute cataract operation could renew sight.
However, a growing number of New Zealanders are also living with significant vision loss, because of tough DHB thresholds for cataract surgery.
That unfortunate group won't show on waiting lists, because they are simply sent away. Only those who clear the lofty thresholds are counted as "waiting". Political pressure and scrutiny is avoided.
The situation is one of the clearest examples of so-called "postcode healthcare", because each DHB estimates how many cataract surgeries can be carried out – balancing demand and capacity – and sets a threshold accordingly.
Those can vary greatly. Auckland DHB, for example, has the lowest surgery threshold in the country. A person with cataracts as bad as Hall's would likely get surgery before having to stop driving.
However, if on the Counties Manukau side of the boundary line, which slices through Otahuhu, they'd be turned down.
Cataracts mostly affect the elderly, but the Weekend Herald has confirmed cases where people of working age have had their drivers licence cancelled and employment imperilled - and still didn't clear the bar for surgery. People who can muster enough money go private. The rest suffer.
Charity at home
Dr Trevor Gray has seen the situation get worse and worse. He worked in the public system for 20 years, carrying out cataract surgeries from the ADHB's Greenlane Clinical Centre in Auckland, and now works at his own private practice, Re:Vision, in Mount Wellington.
"I know the failings of the system, and the strengths," he tells the Weekend Herald. "Ours is one where there are lots of strengths and a few failures. But this is one aspect where there are definitely people falling through the cracks."
Distressed by what he encountered, Gray had an idea – what if private surgeons like himself set aside time once a week or month to do cataract surgery on a needy patient, free of charge?
He anticipated wariness from surgeons if they had to pick patients, or turn them away. They'd be more likely to sign up if all they did was the surgery, he reasoned, and a third party handled referrals and assessment.
Gray chose to work with the Auckland Regional Charity Hospital (Arch), which for ten years has encouraged and enabled volunteer surgeons, including ophthalmologists, to use private theatres at cost or no charge to qualifying patients.

Cataract patients must meet three criteria – they've been declined public hospital treatment, can't afford private, and there's a compelling reason why they need surgery, such as the imminent loss of a driver's licence.
Other ophthalmologists have signed on, and patients from Northland, Auckland, Whanganui and beyond have had their vision restored.
They include a head of department at a secondary school, who in her 50s was finding it harder to mark papers, and was eventually told by her optometrist she couldn't drive – her only way to get to work. Her husband and son had their own health problems and she was the sole breadwinner.
Another was Mavis Hall, who had surgery at The Eye Institute just before Christmas in 2017, nearly 18 months after last being declined by Counties Manukau.
"I was never made to feel any different from those who were paying for it," she tells the Weekend Herald from her South Auckland home. "I felt very comfortable and very blessed, really. I was just absolutely delighted. It is marvellous. [Dr Gray] is such a marvellous fella."

Optometrists face 'horrible' decisions
Gray, a native South African who wears bright red Allbird sneakers with his suit, says he hopes more surgeons sign-up.
"If everyone did it – 20 minutes out of their day, once a month – can you imagine the impact all around the country?"
Optometrists are in a terrible position, he says, something he knows from his time in the public system.
"We'd often see patients referred in from their optometrist who say, 'Well, this patient here, I can't do anything more with glasses, and their vision is worse than driving level vision, so I'm forced, legally, to cancel their licence.'
"They're loath to do this because it's the patient's only source of income – they drive to work or drive as part of their work – or they have to drive for caregiving. And the optometrist is in this horrible position."
The flow-on effects create huge costs for wider society, and government.
"When you realise how low cost a cataract operation is, and how high impact it is – it transforms things overnight and painlessly – there is no other operation in the Western world that has as positive an impact on an individual and their extended family."
Disappearing waiting lists
Patients needing electives (medical or surgical services that aren't required immediately) are prioritised. DHBs give each person a score from 0 to 100 (lowest to highest priority), according to clinical and social need.
If the score reaches a certain threshold - set by each DHB according to capacity and demand - they will be accepted for cataract surgery, to be carried out within four months. DHBs regularly review and update elective surgery thresholds, to ensure patients who are accepted are treated within the four-month wait time.
This nationwide clinical priority assessment criteria (Cpac) booking system was introduced in 1998 as a way to provide transparency and consistency about who gets treated with limited health resources.
Previously, the size of waiting lists, particularly for cataract and hip procedures, was scrutinised each election cycle. That political heat has now largely disappeared.
"It was an incredibly clever thing the department of health did," says Gray, also a clinical senior lecturer at the University of Auckland. "They said, 'Okay, we're going to do away with waiting lists.' Because as the ageing population came on, the numbers just kept increasing.
"If a patient doesn't meet the threshold for that DHB – gone. They are vaporous. There is no waiting list. They are just told, 'You don't meet the criteria, sorry, go away. Come back when things are worse.
"The DHBs have just dumped that back to GPs and optometrists in the primary sector. And these patients keep going back, saying 'Surely I'm bad enough now? I've lost my driver's licence.'"
The size of the problem is impossible to know, Gray says, because optometrists and GPs have stopped referring patients they feel won't meet the DHB cataract funding criteria, as they know there is no point.
Information obtained by the Weekend Herald reveals big differences in local thresholds for cataract surgery: a priority score of 45 out of 100 will get surgery at Auckland and Tairāwhiti DHBs. At least 56 points are needed in the Waikato, 60 in Nelson Marlborough and 61 for Southern DHB residents.
Those differences are significant, Gray says.
"In Auckland, patients who are just about to lose their drivers licence but haven't lost it yet, will almost always get their surgery.
"But if they live on the opposite side of the road at Otahuhu – you have this line – you have already lost your driver's licence before you are even half considered for cataract surgery. There is huge variation and delivery of care around the country."
Postcode healthcare cuts across other specialties. The Herald's Fair Care series has found half of South Auckland children sent for specialist skin conditions are declined an appointment, for example, while across town Auckland DHB declines fewer than one in 10 patients.

The Specsavers effect
Demand for eye services has boomed as Kiwis age and sicken with conditions including diabetes, which if not well controlled can destroy eyesight.
New treatments such as Avastin injections for age-related wet macular degeneration have saved the sight of tens of thousands, but can be needed monthly and have put huge strain on resources.
Services have struggled to cope, and that's cost people their sight. The Herald recently reported on the case of an 11-year-old girl who went blind in one eye after her case was buried amid a huge backlog at Counties Manukau.
Her case isn't isolated. In the past two years, Auckland, Canterbury, Nelson-Marlborough, Northland and Southern DHBs have reported a total of 37 "adverse events" where delays resulted in patients losing sight.
Extra funding and a huge effort by staff, many whom worked overtime and weekends, slashed waiting lists across the country, but pressures remain.
Most recently, health boards have been inundated with referrals from optometrists including Specsavers, after a change in eye screening technology.
At Auckland DHB, this has contributed to a doubling of monthly referrals received, when compared to the previous year. The cataract threshold at nearby Waitematā DHB was recently hiked to try to cope with demand, but this hasn't eased pressure as much as expected.
There's not much spare capacity or cash for eye or other services - all 20 DHBs are forecasting deficits this year, totalling about $346 million.

An end to the 'racial' divide in Auckland eye care?
Dr Brian Kent-Smith, chair of the New Zealand branch of the Royal Australian and NZ College of Ophthalmologists, supports bringing cataract surgery thresholds inline. However, he says a bigger problem is the threat of treatment delays for other conditions.
"In an ideal world, everybody would have their cataracts moved Asap. But nobody should go blind because of a cataract. And they can and do go blind because of untreated glaucoma, untreated macular degeneration, untreated diabetic retinopathy. That is irreversible blindness."
Counties Manukau residents with those conditions had faced longer delays than those lucky enough to live within Auckland DHB's boundaries, he says.
"Basically you had this socioeconomic and largely racial divide - an imaginary line through the centre of Auckland. And if you were above the line you were in the wealthy areas, and you got better care."
Kent-Smith, who works at Northland DHB, says that division could soon be wiped from the map. He understands the two DHBs are discussing merging their ophthalmology departments.
"I am aware of talks taking place…[to say], 'These are Auckland patients, whether we physically bus them from Otahuhu to Greenlane to have the surgeries, or whatever'. If you don't physically have the operating theatres in Manukau, then those people should be operated on at ADHB."
Comparing thresholds 'can mislead'
Health Minister David Clark says the ministry and sector are working together to reduce wait times and improve treatment, and Budget 2018 allocated $32 million a year to support access to a range of planned care.
A focus on one area of eye health must not come at the expense of another, he says, and DHBs are best placed to decide how much funding to put towards different specialties and surgeries: "There will always be variation across the country, in line with different environments, population mix, and pressures."
Ministry of Health spokesman Sam Kunowski says comparing local thresholds in isolation could mislead.
"Quantitative information such as thresholds, intervention rates, and the number of referrals received and accepted, needs to be considered alongside qualitative information from referrers and surgical services to determine whether an appropriate level of access is being offered," says Kunowski, group manager for DHB performance and support.
"New Zealand is likely to always have more patients than our publicly funded non-urgent medical and surgical services can cope with at any one time. This has always been the case, and public health systems internationally face a similar challenge."

Simon Dean, clinical head of ophthalmology at Counties Manukau DHB, says the cataract threshold reflects high rates of smoking, obesity, diabetes and other ill-health risk factors among its more than 569,000 residents.
Counties has about 41,000 diabetics within its boundaries, the highest in the country and well above Auckland DHB (24,500) and Waitematā (28,000).
That piles more pressure on its cataract service, the country's second-busiest. Some diabetics below the threshold for cataract surgery are nonetheless operated on, because diabetic eye screening is reliant on the clinician being able to view the back of the eye.
"A cloudy cataract will often obscure that view," Dean says. "The high number of diabetics in the region adds to the number of patients requiring cataract surgery."
Recent Counties Manukau board minutes suggest unease at the regional differences in cataract thresholds. Dr Mary Burr, general manager of surgery, "noted that it would be helpful if there is a national threshold rather than different thresholds for each area".
Gray also seeks an end to postcode healthcare – "a Kiwi is a Kiwi, and we shouldn't be unequally served by a public service" – and wants to eventually stop having to do surgeries pro bono.
"We'd love for the government to make us redundant," he says. "But there are patients who really highlight the fact the public hospital system is letting society down. They have paid taxes for years, and all they need is a cataract operation to keep driving and working.
"We are trying to do something in the interim, while the public hospital system gets its act together."
• To seek possible access to Auckland Regional Charity Hospital-supported surgery (cataract or other) your GP, ophthalmologist or optometrist must submit application forms available on www.aucklandcharityhospital.org