It's now been six months since New Zealand recorded its first case of Covid-19 - and little could have prepared us for what was to come. So what about the next six months? Science reporter Jamie Morton looks at the five burning questions facing us in the road ahead.
Coronavirus Covid-19: The five burning questions facing NZ

Subscribe to listen
Police hand out face masks to travellers at Manukau Bus Station, upon Auckland's return from lockdown. Photo / Greg Bowker
Coming here means staying in managed isolation or quarantine for at least two weeks, and completing a health assessment and returning a negative test before leaving.
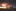
Over the 100-day stretch that Kiwis spent in the freedom of alert level 1 - and even with troubling revelations that more than 50 people left isolation when they shouldn't have - we might've thought those defences were enough to protect us.
But only after the virus' return last month did we learn a mere third of border workers had themselves ever been tested - something the Government announced would start happening back in June.
Embarrassed, it scrambled to fix the problem, and took the extra step of bringing in Sir Brian Roche and Heather Simpson to ensure the gaps got plugged.
It's beefed up its testing of MIQ staff. Encouragingly, the latest round, covering 97 per cent of workers, turned up no positives.
Any confirmed cases now must be moved to a quarantine facility, and work to widen MIQ capacity should ease the pressure to send arriving travellers to hotels outside of Auckland.
While the city's outbreak has been tracked only as far as the Americold coolstore in Mt Wellington, the general and obvious assumption is a border breach somewhere.
It's likely that case will never be solved. But there are plenty of more pertinent questions before us.
One is why officials aren't making testing of arrivals on their third day in isolation compulsory.
The minister in charge, Megan Woods, says that could be looked at more closely if there was ever a case of transmission from an MIQ facility.
National's Judith Collins has pledged a new Border Protection Agency staffed by continually-traced officials - and a requirement for travellers to test negative even before they step on a plane.
NZ First has similarly floated a new, dedicated agency, and also wants MIQ facilities moved to army bases.
Health Minister Chris Hipkins doesn't see the need for another bureaucracy, nor the need for a pre-test, arguing the highest risk time for travellers is actually on their way here.
Are more reintroductions and lockdowns inevitable?

Assuming our border can never be completely water-tight - and that the highly-infectious virus behind this pandemic isn't going away any time soon - further outbreaks may be a given.
Professor Juliet Gerrard, the prime minister's chief science advisor, points out that even Taiwan, which similarly beat Covid-19 with famously sophisticated border measures, had new cases arrive by sea in April.
How far can we squeeze the risk down?
Modelling by researchers at Te Pūnaha Matatini finds that soon-to-be-enforced weekly testing of border workers should double the chances of spotting a case before it could spread further.
Specifically, that early detection could limit an outbreak to fewer than three people, compared with potentially 17 people if it was only picked up in someone who'd already been infected.
But Te Pūnaha Matatini's director, Professor Shaun Hendy, says such modelling works on the assumption that theory will always be put into practice.
"With this outbreak at the moment, we could not put our hands on our heart and say that we are not going to have to go back into lockdown."
In what he considers New Zealand's "pre-vaccine" phase of the lockdown, he sees a good chance of Covid-19 finding its way back into the community.
"It's a massive operational response, and we think it will be very hard to run that in a completely failure-free way."
The good news is more community cases don't need to come with more lockdowns.
New Zealand is getting better at testing and tracing. For instance, the more than 270,000 tests carried out since the Auckland cluster's discovery in mid-August accounted for a third of those across the country's whole pandemic.
"There will almost certainly be more reintroductions of the virus, but there is no reason why we cannot eliminate Covid using a Taiwanese approach with better testing, case finding and contact tracing, rather than lockdowns," University of Auckland epidemiologist Professor Rod Jackson says.
"The next week or two in Auckland will be a great test of this."
Do we have all the tools we need?
We've come a long way in a few months.
The NZ Covid Tracer app has been downloaded more than two million times, and the Ministry of Health is fielding several thousand requests for QR codes each day.
Gerrard's not convinced Kiwis would agree to the Taiwanese approach of state surveillance using GPS on phones - nor the large fines that come with breaches.
"In the absence of GPS monitoring, it would be fantastic to see Bluetooth functionality added to our NZ Covid Tracer app as soon as we can," she says.
"The Irish have led the way here and I think we can learn a lot from them."
Ireland's Covid Tracker app harnesses a phone's Bluetooth signal to hook up with devices carried by people lingering within two metres for more than 15 minutes.
New Zealand's CovidCard isn't an app, but a separate card worn on a lanyard.
Despite original backer and entrepreneur Sam Morgan pulling out of its development, the Government is pushing ahead with two trials - one in Rotorua and one among MIQ staff and returnees.
But experts point out that such digital solutions can never replace manual tracing, especially given a large chunk of the population either don't have phones, live in remote communities, or move frequently.
"Working with highly-connected people within those communities may be a much more effective way to reach people than phone or app-based methods," Otago University epidemiologist Dr Amanda Kvalsvig says.
"These methods may also be much more acceptable for marginalised communities where people can feel threatened when approached by officials."
There's much improvement that can also be made on the testing front, too.
Without better tech, the country might be at risk of "false negative" tests which leave infected people under the impression they're Covid-free, Kvalsvig says.
Until that threat is addressed, she suggests people in high-risk places like the border who return negative tests should still distance themselves for a set time afterward.
And what is that better tech?
Scientists at ESR are exploring the potential for saliva tests, which may prove more sensitive and effective, and less invasive, than the nasal swabs Kiwis are used to.
There are opportunities for more serology or antibody testing - blood tests that can show if a person may have once had been infected without knowing, revealing hidden chains in outbreaks with mystery sources - and rapid antigen tests.
The latter, still being developed, can identify those who are infected within a few minutes, allowing them to self-isolate and avoid infecting others.
"The pandemic is clearly going to be with us for some time, so it's worth investing in better systems and tools," Kvalsvig says.
"These approaches can also help us to react more effectively to other infectious disease outbreaks, including the next pandemic."
When will we get a vaccine?
It's New Zealand's bridge back to the rest of the world, but, depending on which expert you ask, a successful vaccine might be a reality by early next year or years from now - if at all.
University of Auckland vaccinologist Associate Professor Helen Petousis-Harris says the most promising candidate is the University of Oxford and AstraZeneca's viral vector vaccine.
Dubbed ChAdOx1-S, it's already been shown to prompt the one-two hit of a T-cell and antibody response with a month of inoculation, and is now well into the critical and final Phase III stage.
"They anticipate having results in the fourth quarter, and starting to distribute it globally from that point forward," Petousis-Harris says.
"So it does look like we'll be seeing the prediction of having a vaccine next year play out."
But Professor Graham Le Gros, the programme director of Vaccine Alliance Aotearoa New Zealand – Ohu Kaupare Huaketo, thinks a vaccine might still be as long as two years away.
"The brutal truth is we don't know a lot about this virus and how to make an effective vaccine against it," he told the Herald last month.
"I don't want to depress anyone, but it is going to take time. We have to be patient. My guess is two years."
Professor James Ussher, the alliance's science director, says some vaccine candidates might be shown to be "efficacious" early next year "at the earliest".
And of course, Petousis-Harris adds, where exactly New Zealand is in the queue remains to be seen.
The Government has earmarked hundreds of millions of dollars - it won't disclose precisely how much, for commercial reasons - to get Kiwis and our Pacific neighbours as far up the line as possible.
That involves making our own batches here. Around $3m of that funding will go to Kiwi biotech company Biocell to upgrade its facilities so it can roll out 100 million doses.
The sector has further suggested New Zealand might piggy-back off Australia's just-signed deal with AstraZeneca for local production.
For Kiwis impatient for an agent now, scientists point out the global race for a vaccine is without precedent in scale and speed.
As at last month, 29 vaccine candidates around the world had reached the clinical evaluation stage, with seven in Phase III.
One Kiwi consortium has been exploring potential homemade candidates - such as an inactivated vaccine approach led by Otago University's Professor Miguel Quiñones-Mateu, and a recombinant spike protein vaccine being developed in Dr Davide Comoletti's Victoria University lab - for the past few months.
Fonterra's cutting edge research centre in Palmerston North has lent biotech company CVC an homogeniser, used to break up particles, to assist vaccine researchers trying to access specialised equipment as they work towards first clinical trials.
Before the latest cash injection was announced, the Government had already poured $37m into securing a vaccine here, including $5m for manufacturing one here, and $10m for local research.
It may even offer its ultimate vaccine supplier indemnity against any claims arising from its use to help fast-track the process - although regulator MedSafe still wouldn't allow a vaccine whose safety wasn't backed by clinical data.
Nevertheless, Kiwis don't appear to have any qualms about getting the shot when it arrives.
A recent poll found three-quarters of New Zealanders would get the Covid-19 vaccine once available - but only half would be willing to pay for it.
Does New Zealand need an oversight overhaul?
National aren't alone in arguing for a bureaucratic shake-up to better manage our pandemic response.
While we wait for a vaccine, Otago University's Professor Michael Baker figures the time is right for radical change at the highest levels.
In an op-ed in The Conversation, Baker and fellow Otago epidemiologists Kvalsvig and Professor Nick Wilson made the case for a new science council to better inform the national response and support the research sector.
Right now, the Government can draw on its in-house experts and respected independent science advisor Dr Ian Town, along with Gerrard's office and its technical advisory group, of which Baker is a member.
On top of a special council, Baker is keen to see a well-resourced research and development strategy, and for the Government to make its data more refined and open.
Immediately after the October election, he's called for an official inquiry into the response to pinpoint weak spots and to pave the way for a new national public health agency.
Even before Covid-19, he argues recent disasters like the Havelock North gastro outbreak and last year's measles epidemic spelt the clear need for one.
The Government has shown little interest in the concept, nor does it want to hold a rapid inquiry, but, for Baker, they present some obvious ways to bolster New Zealand's elimination playbook.
"Of these measures, I think the high-level group is the most urgent to provide a way of integrating the streams of science advice into a more coherent, medium-long term plan," he says.
Gerrard says this is already happening in a sense, with an informal group bringing together modellers, scientists and policymakers, and chaired by Treasury deputy secretary and chief economic advisor Tim Ng.
"This could perhaps form the basis of a more formal structure."
More broadly, she's happy with where New Zealand's response is now sitting.
"Like the rest of the world, we have quickly adopted new tools to fight Covid-19," she says.
"We are in a far stronger position now than we were for our first wave of infection."