Nearly two weeks since new Covid-19 cases were confirmed in the community in Auckland, no one knows where they came from. Isaac Davison talks to the scientists at the forefront of solving the puzzle.
Professor Shaun Hendy was nursing a beer in a pub on Vulcan Lane 11 days ago when an email flashed up on his mobile phone screen.
It was from a senior official at the Department of Prime Minister and Cabinet (DPMC), and it was titled urgent.
The DPMC official wanted Hendy's team at scientific institute Te Pūnaha Matatini to do statistical modelling of a new Covid-19 case in Auckland with no links to the border, and they wanted it fast.
"At first we thought it might have been a drill, because we have been talking about having a dry run for this," said Hendy.
"But unfortunately it wasn't. There was a sinking feeling in everyone's stomachs as it became more and more evident it wasn't."
Having moved to a restaurant for dinner, Hendy worked with his phone glued to his ear and his laptop on the table. "I stopped drinking when the first email came through," he said.
An hour later, at around 7pm, he emailed the analysis back to the Prime Minister's advisors. His team of researchers at the University of Auckland estimated that there were between 30 to 70 people outside managed isolation in Auckland who were carrying Covid-19.
The email was forwarded to Cabinet ministers who were meeting that evening, and at 9.22pm Prime Minister Jacinda Ardern went on television to reveal a bombshell - there were four new positive Covid cases in the community and more cases were likely. That cluster has since grown to more than 70 people.

Since that moment, Hendy has been among hundreds of scientists, laboratory workers, contact tracers and others who have been working around the clock to find the source of infection for this new outbreak. They have been armed with techniques and innovations which have emerged or been fine-tuned since the first lockdown in New Zealand. And they have been working with the same urgency of those first, frantic hours two Tuesdays ago.
Yet nearly two weeks on from Ardern's late-night press conference, the source of the surprise cluster in Auckland remains a mystery.
"The trail is quite cold now," said Professor Michael Baker, an epidemiologist from the University of Otago's Department of Public Health.
"With an outbreak you are always looking backwards. It may be that the source had a very mild illness, and they maybe infected another person, who introduced a cluster, and none of those people even knew they had the infection. That's the difficulty."
As each day goes by with falling numbers of positive cases, confidence grows that the cluster which began in South Auckland has been contained. But finding its source is still a top priority, because it will reveal the chink in New Zealand's pandemic armour and help prevent it being breached again.
One of the most potent weapons in this search has been genome sequencing, which involves matching the genetic fingerprints of new Covid cases with previous or existing cases in New Zealand and overseas to work out where they came from.
"Perhaps the biggest difference from the first outbreak is that back then we now know we had at least 277 separate virus introductions," said the Prime Minister's Science Advisor Professor Juliet Gerrard - referring to the number of different strands of the virus which arrived from overseas.
"This time we have two - and only one that seems to have led to a significant cluster. This means that genomics is able to be used forensically to help track how the virus moves from person to person, and which cases are connected."

After the four family members in South Auckland tested positive last week, their test swabs were flown to Wellington the following day and then couriered to an Institute of Environment Science and Research (ESR) lab. The genetic material was separated from the mucus on the swab and then analysed by computer.
If its genetic makeup matched a previous case in ESR's database, the problem would have been solved within 24 hours of the discovery of the new positive cases. That information could then have been passed to contact tracers who would look at any links between the old cases and the new ones.
But there was no match.
The next step was to check whether the samples matched an international database of Covid cases. There is a sprawling, Interpol-like international database for virus cases, and countries which are doing sequencing put their data online for other countries to check if they have a match. If a match was confirmed, officials could look at recent arrivals to New Zealand from that country.
It was discovered that the sequences from the cases in Auckland were similar to cases in the United Kingdom. But again, there was no strong match, and the mystery remained.
Dr Jemma Geoghegan, an evolutionary virologist at the University of Otago, said there were barriers to getting a perfect match. Some samples had a "low viral load", or a faint sign of the virus, and a genome could not be extracted. New Zealand was also at the mercy of other countries and how much sequencing they were doing.
"All evidence points to the fact that this is a new introduction from overseas," Geoghegan said. "[However] we can't find the evidence from overseas because many countries aren't actually sequencing the genomes of their cases. We are just relying on that."
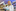
Until now, this work has mostly been theoretical for Geoghegan.
"It is quite surreal. For years I have spent my career researching how viruses jump to new hosts and spread through populations. And how the genetics evolve through time and space.
"And now genomic sequencing and this sort of analysis has come to be part of the crucial response. It's a silver lining of this horrible pandemic."
While the genomic testing has not yet found the source of infection, it has given scientists some reassurance.
As the virus is passed on from person to person over time, it mutates, and these changes can be detected during sequencing. The further it travels, the more it changes. If the genetic makeup of the latest confirmed cases in Auckland were significantly different from the cases two weeks ago, it could indicate that the virus has passed through many more people who have not yet been found.
"In the Auckland cluster, all of the genomes are very, very closely related," Geoghegan said. "Which reassures us that we are likely capturing the majority here. But we are getting samples daily, and this could change quickly."
Two days after the positive cases were confirmed in South Auckland, the most reliable methods of investigation - diagnostic testing, contact tracing and genome testing - had failed to turn up the source of infection.
The Ministry of Health then added a more unusual line of inquiry to its investigation. It started testing the surfaces at the Americold cold storage facility in Mt Wellington, the workplace of the Auckland cluster's index case, a man in his 50s. Police were called in to use their criminal forensic skills on the investigation, which focused on whether the virus could have come to New Zealand via frozen freight.
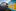
Little is known about whether this is actually possible. The virus can survive for up to 72 hours on plastic and stainless steel, or less than 24 hours on cardboard. One piece of research, in the Lancet, showed that the virus remained stable for more than two weeks at 4C. There have also been reports that Covid-19 was detected on frozen food packaging which was imported to China - chicken wings from Brazil and fish products from Ecuador. But there was no evidence to suggest infection had then occurred from these imports.
Gerrard, the Prime Minister's chief science advisor, was asked to provide advice on the likelihood of the outbreak starting in this way. She concluded that it was "very unlikely" source of infection, but could not completely rule it out.
This line of inquiry has now all but wrapped up - another dead end.
Dr Siouxsie Wiles, a microbiologist from the University of Auckland who specialises in infectious diseases, said that all possible routes of incursion had to be covered off.
"One of the reasons I'm really glad they were pursuing the Americold angle, as well as everything else, is if it was really was true, it would show that here is a weakness that we need to plug. Not just us - but every other country in the world."
A week after the latest outbreak was confirmed in Auckland, the mystery briefly became more complicated.
A maintenance worker at the Rydges Hotel in central Auckland tested positive for Covid, despite having no close contact with anyone at the hotel's managed isolation facility. The infection was quickly linked to a female traveller who had come from the US, which meant the source of infection was known. But it was not known how it made the jump from the traveller to the maintenance worker.
In an attempt to find an intermediary which links the two people, guests and workers at the hotel had blood tests.

Baker said nose and throat swabs had a 10 per cent false negative rate. Serology, or blood tests, gave the ministry a second chance to find the intermediary. Those blood tests are now taking place - the latest addition to a growing investigative arsenal.
In the end, the missing link in the story was found through more humble means - hotel swipe cards. Data from the cards showed that the worker used a lift minutes after the traveller, and possibly contracted the virus by touching a surface, like an elevator button.
On top of the new, innovative detective work, some of the existing testing methods have been ramped up and are now operating at far greater capacity. Diagnostic testing of nose and throat swabs has reached 26,000 a day.
"The numbers were absolutely off the scale," said Bryan Raill, a medical laboratory scientist at Middlemore Hospital. Staff at his lab were working into the early hours of the morning to process up to 3000 samples a day, any one of which could be the clue to preventing a resurgence of a pandemic in New Zealand.
Labs have increasingly used a technique known as "pooling", in which up to eight samples are mixed together and tested at once. If it comes back negative, all the samples are negative. If it's positive, the samples are tested again individually.
"It's like this," said Raill. "If you are at Sylvia Park shopping mall and you've lost your 5-year-old boy. There's lots of lost 5-year-olds but he's got a yellow pirate hat on.
"You can amplify that so suddenly you've got dozens of copies of him with yellow hats on - how easy he becomes to spot. And that's what we do with viral fragments - ramp up the numbers so you get a signal."
Despite the growing, diversifying hunt for the source of infection, the mystery of where it came from lingers on.
"We're running out of methods now," Baker said.
While it would not assist with the current investigation, he said further measures could be used to detect the source of infection in future, including a Covid Card which people carry in their wallet and which detects any close contact with positive cases.
Sometimes the task of tracking the microscopic source of the latest outbreak weighs on scientists. It can be daunting, sighed Siouxsie Wiles: "It is a tricky damn virus."
It is more difficult than finding a needle in a haystack or a grain of sand on a beach. The average diameter of the virus is 120 nanometers. A human hair is about 75,000 nanometers. Somewhere in Auckland, a particle that size could be fading inside an oblivious person's respiratory tract, the hidden piece of the puzzle which could help prevent another pandemic outbreak in New Zealand.
"It's quite possible we may never know the origin," Geoghegan said. "We're looking back in time now. But we'll keep looking. We'll keep looking for clues."

