In Boston and in the Netherlands, scientists are racing to build a vaccine against virus strangling the world.
Each workday morning in March, Noe Mercado drove through the desolate streets of Boston to a tall glass building on Blackfan Circle, in the heart of the city's biotech hub. Most residents had gone into hiding from the coronavirus, but Mercado had an essential job: searching for a vaccine against this new, devastating pathogen.
Parking in the underground lot, he put on a mask and rode the empty elevator to the 10th floor, joining a skeleton crew at the Center for Virology and Vaccine Research at Beth Israel Deaconess Medical Center. Day after day, Mercado sat at his lab bench, searching for signs of the virus in nasal swabs taken from dozens of monkeys.
The animals had been injected with experimental vaccines Mercado had helped create. The monkeys then had been exposed to the coronavirus, and now Mercado was finding out whether any vaccine had protected them. One morning, after he loaded all the data into a software program, a single telling graph set his heart beating: Some of the vaccines, it appeared, had worked.
Mercado hurried around the lab to share the news. Given the times, there were no hugs, no high-fives. And he did not bask in glory for long. Making a vaccine demands patience, attention to detail — and a tolerance for bitter failure.
"Yeah, I'm excited, but I'm also thinking about the next step," Mercado later recalled. "What if it doesn't pan out?"
The coronavirus has now infected about 14.4 million people worldwide and killed at least 605,700. Millions more may die. The only hope for a long-term protection, literally the only shot at a return to normal life, is an effective vaccine.
In January, researchers at the vaccine centre dropped everything they were doing to find one. The man heading up the effort is Mercado's boss, Dr. Dan Barouch, director of the centre and one of the world's leading vaccine makers.
Now they are about to take a major step forward. Janssen Pharmaceutica, a division of Johnson & Johnson, has been working with the Beth Israel team to make a coronavirus vaccine based on a design pioneered by Barouch and his colleagues 10 years ago.
This week, clinical trials of the vaccine will begin in Belgium. Barouch's team will soon start up a trial in Boston.
The past six months have been a blur of long weeks and late nights, of strict safety measures and scarce lab supplies. "Everything has been orders of magnitude more challenging than in the pre-pandemic era," Barouch said.
Researchers around the world have been making vaccines of their own, some with dead viruses, others with protein fragments and strings of DNA. As of July, there are over 135 vaccines in preclinical tests, and more than 30 others in clinical trials on people. Never have so many vaccines moved so quickly into trials for one disease.
Since January, Barouch's team in Boston has run experiments in cells and monkeys, while Janssen's researchers in the Netherlands have raced to find a recipe for producing the new vaccine in huge quantities. Already they have started producing a batch for the clinical trials.
If the vaccine proves safe in initial tests, a trial for efficacy will begin in September. If that experiment is successful, Johnson & Johnson will manufacture hundreds of millions of doses for emergency use in January. Over the course of next year, the company plans to produce up to 1 billion doses.
While Johnson & Johnson is one of the world's biggest companies, with a market capitalisation over US$370 billion ($559 billion), it's a fairly small player in the vaccine market. On July 1, its Ebola vaccine received approval from the European Commission. Its vaccines for other diseases are still in clinical trials.
Even so, the US government has given US$456 million to Johnson & Johnson, funding from the Trump administration's Operation Warp Speed; the company has invested another US$500 million in the coronavirus vaccine project.
Barouch and his colleagues are finishing tests of the final formulation in monkeys. In coming months, they will begin to see how people respond to the injection.
It is a monumental task to develop a vaccine so quickly against a pathogen that no one had heard of before this year. But, Barouch said, "I'm even more optimistic now than I was several months ago."
A cluster of 41 cases in China
On January 10, Barouch hosted the lab's annual retreat on the top floor of Boston's Museum of Science.
At the end of the meeting, they discussed news of a mysterious cluster of 41 pneumonia cases in Wuhan, China. "Forty-one cases seemed like a lot at that point," Barouch said.
The new cases reminded them of severe acute respiratory syndrome, a disease caused by a coronavirus, which had appeared in China in 2002 and had spread to 29 countries, striking 8,096 people and killing 773, before it was halted. Chinese scientists had just reported that another coronavirus was on the loose.
"We thought, maybe we should make a vaccine for that," recalled Jinyan Liu, a staff scientist at the centre. But without more information about the new virus, there was nothing they could do.
Everything changed that night. At 9:41pm, Dr. Kathryn Stephenson, the director of the centre's clinical trial unit, sent Barouch a short email from her iPhone: "This was released today — saw someone link to it on Twitter."
The link led to an open-access virology site where scientists based in China had posted a file containing the entire genetic sequence of the new coronavirus. "Please feel free to download, share, use, and analyze this data," wrote Yong-Zhen Zhang, a professor at Fudan University in Shanghai and the leader of the consortium.
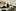
Five minutes later, Barouch emailed Liu, Mercado and Zhenfeng Li, a research assistant at the centre: "Can one of you extract the new coronavirus sequence from this file?"
Soon the four scientists were poring over the sequence, a series of 30,000 genetic letters that no one had seen arranged in this order before. "We worked Friday, Saturday and Sunday, day and night," Liu said.
By the end of the weekend, they had a good idea of what they were up against, and how to defeat it potentially. On Monday, the scientists returned to the lab, ready to start on the most ambitious endeavour any of them had ever undertaken.
But the researchers would not have to create a vaccine from scratch. They would be working from a playbook that Barouch had been writing for 20 years.
By 2004, when Barouch opened his first lab at Harvard Medical School, he had gained a reputation as an ambitious young researcher. He immediately set a suitably daunting goal: a vaccine against HIV, the virus that causes Aids.
The virus had been found in 1983, but two decades of vaccine work had led to one disappointment after another. The standard ways to train the immune system to recognize a virus failed when it came to HIV.
Barouch decided to try something different: a vaccine made from another virus. They chose adenovirus serotype 26 — Ad26, for short — a relatively rare virus that causes mild colds but is very effective at invading human cells.
To create the vaccine, they worked with Crucell, a Dutch company bought by Johnson & Johnson in 2011. The researchers disabled the Ad26 virus so that it could only invade cells but not multiply in them.
Then they added a gene from HIV. Cells infected with Ad26 would make HIV proteins that drifted in the bloodstream, priming the immune system.
In experiments on monkeys, the vaccine offered protection against HIV. In trials on people, the vaccine was safe and triggered a strong immune response against the virus. But the trials to see if it effectively protects against the virus are still underway.
In 2016, amid the Zika epidemic, Barouch and his colleagues retooled their Ad26 vaccine to make Zika viral proteins. They got as far as trials that showed the vaccine was safe in people and generated an immune response, but shelved the project when the Zika epidemic retreated.
As the new coronavirus began to spread in January, the lab already knew how to make a vaccine for a sudden outbreak. What they needed now was a way to target the new virus.
Previous research on Sars and other coronaviruses made the choice clear. They would prime the immune system to attack the so-called spike proteins that cover the surface of the new coronavirus.
'A war we could win'
As January wore on, Barouch realized that Covid-19 was going to be a far graver threat than SARS.
"We would not be able to stop this virus by traditional public health measures," he said. "It was absolutely clear that we needed a vaccine."
He emailed to Johan Van Hoof, the head of vaccines at Janssen. "I am writing today because the coronavirus outbreak in China is looking bad," Barouch wrote. "Are you interested in making a rapid Ad based vaccine like we did for Zika in 2016-2017?"
Two minutes later, Van Hoof replied, "Would a call work now?" Four days later, they signed an agreement to collaborate.
The Center for Virology and Vaccine Research has a staff of dozens of researchers, including medical doctors, senior scientists, postdoctoral researchers, grad students and assistants just out of college. Barouch's team turned away from projects on HIV and other diseases, and divided up the work to make a coronavirus vaccine.
Mercado and his colleagues fashioned copies of the coronavirus gene that directs production of its spike protein. They came up with 10 variations to see which would produce the best immune response.
Meanwhile, Katherine McMahan, a research assistant at the centre, worked on the team building a test for spike antibodies in the animals that would receive the vaccine. Creating it took up most of her waking life. On some days, she didn't get around to eating lunch till nighttime.
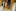
In late February, researchers injected the spike genes into mice and then sent McMahan blood from the animals. McMahan's test confirmed that they were making coronavirus antibodies.
McMahan was near tears: "It began to feel like a war that we could win."
Outside the lab, though, there was no sense that a war was coming. She urged family and friends to stock up on food and other supplies, without much luck.
"Many of us were having a Chicken Little experience," she said. "You're saying, 'Look, you've got to take this seriously,' and getting blown off."
Soon enough, people desperately ill with Covid-19 flooded into Boston's hospitals, and the city began to shut down. Barouch's team shifted from studies on mice to monkeys.
The nasal swabs that Mercado examined revealed that some versions of the vaccines only partly protected the monkey; others worked much better. As the investigators reported in the journal Science, they couldn't detect the virus at all in eight of the 25 monkeys who got experimental vaccines.
The results gave Barouch hope that one of his team's vaccines — or one of those developed by another group — might work. "It's the real deal," he said.
More monkeys were injected with the Ad26 virus, now equipped to produce the spike gene. Barouch predicts that this vaccine will induce higher levels of antibodies than the prototypes did.
The experiment will also provide crucial clues about how the immune system responds to the Ad26 vaccine. Some vaccines confer protection mostly by triggering the body to make antibodies that attack a virus. But others can stir virus-hunting immune cells to join the attack.
The results of the latest round of experiments will be published within a few weeks.
For all the progress made by Barouch's team, the Ad26 vaccine has its skeptics. John Moore, a virologist at Weill Cornell Medical College, said other types of vaccines tested in animals had produced higher levels of antibodies. These vaccines, made of viral proteins, would be his choice for a weapon against the coronavirus.
Six companies have already begun human safety trials of their protein vaccines. "That's what I'd be doing," Moore said. "It's freaking obvious."
One drawback of viral-protein vaccines is that they take more time to produce in huge quantities. Other vaccines, like Johnson & Johnson's Ad26, will come more quickly; Moore acknowledged that they might work well enough to provide protection.
If so, there may not be a need for a better but slower vaccine. "If Plan A works, then you don't need a Plan B," Moore said.
A virus seed
While Barouch and his colleagues were testing the vaccines in the United States, a team of Johnson & Johnson researchers was gearing up to make them in the Netherlands. They have experience with Ad26, which they have used to make vaccines for HIV, Ebola and other viruses.
Making an Ad26 vaccine requires remodelling an adenovirus and then creating vast quantities of the new version. But Ad26 cannot multiply in ordinary cells. It must infect specially engineered ones.
Johnson & Johnson's technicians produce batches of these cells in huge vats filled with a nutrient-rich broth kept at a constant temperature and stirred to pull in oxygen.
"It's to make the cells feel happy and comfortable, to make product," said Paul Ives, the senior director of drug development at Janssen.
Once a batch of these nurturing cells has grown sufficiently, Ives and his colleagues infect them with the modified Ad26 viruses. Each cell churns out thousands of new viruses, which are removed and purified so that they can be used as vaccines.
Ives' team has been measuring how quickly various versions of the revamped Ad26 cell can multiply. Some reproduce more easily than others, they have found.
Even a slightly slower reproduction rate could leave Johnson & Johnson with a huge shortfall in vaccine doses. "It can mean you have 300 million vaccines or 30 million," said Paul Stoffels, chief scientific officer at Johnson & Johnson.

Ives and his colleagues recently chose the best virus for the vaccine and turned it into their "master virus seed." A batch of this seed will become the vaccine used in the clinical trials.
And if those trials show that the vaccine is effective, the factory will use the same master virus seed to make an emergency supply that would be distributed at the start of 2021. "We can theoretically produce 300 million vaccines," Stoffels said.
The company has partnered with an American vaccine maker and is also setting up two plants in Asia and Europe, "so that we can come to a manufacturing capacity north of a billion vaccines," Stoffels said.
Florian Krammer, a virologist at the Icahn School of Medicine at Mount Sinai, wonders if Johnson & Johnson can live up to that promise, given that it has never made Ad26 at anywhere close to this scale. "Making a couple of million doses over several years for clinical trials is very different than producing hundreds of millions of doses within months for the market," he said.
Johnson & Johnson has said it will distribute the vaccine on a nonprofit basis. Speaking in March to Belgian newspaper De Tijd, Stoffels calculated a cost of US$10 per vaccine. In a follow-up interview, he said that the price would not be set until the company finished making an initial supply.
Amid a pandemic, critics say Johnson & Johnson should not be allowed to set the terms. "If we get a vaccine, it should be free and available to everybody," said the Rev. Dr. William J. Barber II, the president of the North Carolina NAACP and a critic of Johnson & Johnson's drug pricing. "How do you get these big, massive awards to produce a vaccine without any rider on the money saying it must be used in a way that it's affordable to everybody?"
For now, no one knows if the vaccine will actually work. Barouch and his colleagues are getting ready to inject the Ad26 vaccine into hundreds of volunteers in Boston in late July. Researchers will not only observe whether the vaccine is safe but also look at the antibodies it prompts the volunteers to make. If those trials produce promising results, Johnson & Johnson will run a march larger one in the fall.
Barouch and his colleagues are planning a third round of experiments on monkeys. They want to inject them with antibodies against the coronavirus and then infect them. By giving different monkeys varying doses, the investigators hope to figure out what level of antibodies in the humans are required to prevent Covid-19.
And so, Barouch and his colleagues continue to work nights and weekends.
"I keep a series of Post-it notes at my desk, which I update each day with the number of lives lost to Covid," McMahan said. "When I'm feeling drained, I look at that number."
Written by: Carl Zimmer
Photographs by: Tony Luong
© 2020 THE NEW YORK TIMES
