Doctors Owase Jeelani and David Dunaway have worked together for more than a decade at Great Ormond Street Hospital. Their latest operation, which made headlines last week, was their most challenging yet: separating conjoined twins Safa and Marwa over 50 gruelling hours. They tell Hilary Rose how they did it.
It was a day like any other for Owase Jeelani, consultant paediatric neurosurgeon at Great Ormond Street hospital in London, when his phone rang back in April 2017. At the other end was a fellow neurosurgeon in Peshawar, Pakistan. He had an interesting case, he told Jeelani. Two healthy girls, identical twins called Safa and Marwa, born three months previously to a woman from rural northern Pakistan. There was just one problem. They were conjoined, fused together at the head. Could he help?
"My reaction was, 'Yes, of course,' " says Jeelani, "and that's where it all started."
Jeelani's phone rang because he, along with his colleague Professor David Dunaway, had performed successful separations on two sets of conjoined twins, in 2006 and 2011. In other words, they were well on their way to becoming the leading experts in the procedure after only two successful surgeries, an irony not lost on them. A Skype conference was convened, when Jeelani, 44, and Dunaway, 63, could see that the twins had a similar vertical configuration to the previous sets. Their skulls, says Dunaway, were like stovepipes, with the brains joined at a spiralling angle. They could lie on their backs, or their fronts, but they couldn't walk, crawl or sit up. They were physically joined together, yet they'd never set eyes on each other. Getting to the join between the two brains, they realised, and accessing the blood vessels they shared, was going to be difficult. Then there was the question of ethics. Could both twins theoretically survive without the operation? Was there a good chance for one, but not the other? Might either or both of them die? Working simply on the principle of "do no harm", Jeelani says he would turn down any hypothetical case that would effectively kill one twin to save the other.
"Except," he adds, "if we know that by not doing anything, we lose both."
So he worries about playing God? "Indeed."
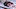
"Our initial feeling," says Dunaway, a plastic and craniofacial surgeon and head of the unit at Great Ormond Street, "was that there was a good chance they'd be able to be separated. But I never thought they'd get to us. They lived in rural Pakistan. There didn't seem to be any prospect of funding their surgery."
Their mother, Zainab Bibi, 34, is a housewife. Her husband, a taxi driver, died of a heart attack two months before the twins were delivered by caesarean section. It was a difficult time, Zainab says with considerable understatement, but she had the support of living in a compound with extended family. As for Jeelani, this felt personal. He was born in Srinagar in Kashmir, barely 320km as the crow flies from where the twins were born. He and Dunaway were prepared to act pro bono, but Great Ormond Street, and the NHS, would need to be paid. The best outcome depended on operating as soon as possible, ideally before the twins turned one. The clock was ticking. So for 15 months, in his every spare moment, Jeelani tried unsuccessfully to raise enough money. Eventually, almost exactly a year ago, they took the decision to fly the children to the UK even though there was still a shortfall of cash. The twins were now 19 months old. If the doctors were going to operate, it had to be now.
At this point, fate intervened. The twins arrived in London one Friday in October 2018, with their mother, uncle and grandfather. Zainab's seven other children were left behind in the care of extended family, and she hasn't seen them since except via Skype. The following week, Jeelani happened to meet a friend for lunch. He was worried, he told her. There were these twins, they needed an operation, but there wasn't enough money. The friend picked up her phone, made a call and handed it to Jeelani. "Tell him about the twins," she said. So he did.
"I said, 'I'm Mr Jeelani, I'm the head of neurosurgery at Great Ormond Street and we have these conjoined twins from Pakistan.' I thought I had to do my five or ten-minute spiel. Literally two minutes in, he said, 'Doctor. Let's cut a long story short. How much money do you need?' I told him and he said, 'Fine, you'll have the money by Monday,' and put the phone down."
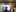
The man was a wealthy oil broker called Murtaza Lakhani, who travels widely and splits his time between London and Vancouver. Great Ormond Street declines to say how much he donated.
"The twins are from Pakistan, which is where I am from originally," Lakhani later told the BBC. "However, the true reason for me helping them was because it was an operation that was going to save the lives of two children. For me, it was an easy decision. It's how you build the future."
The planning was already done. Separating conjoined twins used to be done in one marathon operation, says Dunaway, "And generally it was a disaster, and everybody ended up with brain damage."
Building on the work of two surgeons in New York, Jeelani and Dunaway planned a three-stage operation, which would minimise the "insult" to the brains and give them a chance to recover between operations. It would be, Dunaway says, a process of "chipping away" at the problem. A 100-strong team including bioengineers and 3D modellers set to work. The surgeons used virtual reality headsets to explore 3D models of the girls' brains, although Jeelani, used to working from CT and MRI scans, found it to be a slight case of information overload.
The first operation began on October 15, 2018, and lasted 20 hours. The second, a month later, lasted 11, and the final 15-hour surgery took place in February this year, when the twins were physically separated. In total, there had been 50 hours of major operations, plus another dozen minor procedures of an hour or so: applying skin grafts or inserting saline sacs into the girls' foreheads, which would slowly expand, creating new skin that could later be harvested to cover their wounds. Technically, says Jeelani, the surgery itself isn't too difficult. He trained as a doctor in Nottingham and Southampton, before undergoing specialist training in Canada and the UK in neurosurgery and craniofacial surgery.
"I'm not being facetious," he says, "but we do supercomplex surgeries here on a weekly basis. We take out brain tumours. We deal with children who have malformed faces and heads. We reconstruct skulls. What's difficult for me and David, and the team, is that a lot of what we do [with conjoined twins] is, at best, a guess. It's an educated guess, but it's still a guess, and if we get it wrong, we will cause a problem. That's the hardest part."

It helps that he and Dunaway, who are both married with children, have a professional bond so close that they liken it to a marriage. They've operated together thousands of times, for more than a decade, and can instinctively read each other's body language in theatre. Jeelani says that he has absolute trust and confidence in Dunaway's abilities, "and that enables you really to push it out, to work at the limit knowing that somebody's got your back".
"There is something about the chemistry between us that works really well," agrees Dunaway. A father of three, he qualified first as a dentist, before going back to read medicine at Manchester University. He took up the post at Great Ormond Street in 2000 and commutes there from a small village near Loch Lomond, close to where he used to work in Glasgow.
"People say we're such an unlikely couple – they use the word couple! – but he has strengths where I have weaknesses, and I have strengths where he has weaknesses. We can challenge one another without feeling like it's criticism, or being negative, and that's really important in this kind of surgery. It's an extraordinary relationship."
The first operation went without a hitch. Jeelani followed his usual routine of rising at 4.30am, going for a half-hour swim, timing every stage of the operation in his head and arriving at the hospital at 6.30am. He felt good, he remembers, and optimistic. They set to work finding and separating blood vessels, deciding which twin should get which when they were shared, and putting temporary clamps on arteries to see if it made the brain look, in Jeelani's word, "bothered". It's about the colour and texture, he explains. If that particular part of the brain is only fed by the artery you've clamped, the brain goes pale and starts to swell. This is bad news, and five minutes is usually long enough to tell if it's happening. The next day, the twins came round quickly, "without really batting an eyelid". The second operation was not so smooth.
"We were thrown right from the onset," Jeelani remembers, "because they started bleeding from the start. This was not expected. Both girls had formed clots in the blood vessels in their necks after the first operation. As a result, the blood pressure in their heads was very high, but there was no way for us to be able to tell this beforehand. It wasn't until we opened, and they started hosing blood, that David and I were like, 'Woah, what's going on here?' "
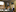
The anaesthetist, who was usually completely unflappable, said that she was losing control. "That did make me worry, that she'd raised a real alarm," says Dunaway. "When things go wrong, you slow down and force yourself to be calm. The worst thing you can do is panic and do things quickly."
They debated whether to abandon the operation, regroup and return another day, but decided that delay might make their jobs harder. Eventually, 11 hours later, at 6.30 in the morning, they finished stage 2 and went straight into their routine morning meetings. It was 2pm before Jeelani got back to his home near Epping Forest, physically exhausted having had no sleep at all. He crashed out, woke up two hours later and called the hospital to check on the girls. He was given what he later found out was incomplete information but, at the time, groggy and disorientated, it tipped him over the edge.
"I was standing at the kitchen counter and I was told, 'Safa's not looking too good. She's making no attempts to breathe and she looks mottled.' No attempts to breathe and mottled is dead. That's what happens when you die. That was it. I had nothing left in me. I broke down. My wife helped me sit down, gave me a glass of water and said, 'Call David.' I could see the panic in her face. She'd never seen me like this before. It's never happened in front of her, or in front of others. I could see the fright on her face and I almost feel guilty now for what I put her through at that stage."
He and Dunaway raced back to the hospital. They didn't leave for another three nights. Safa, they discovered, had had a stroke. During planning for the operation, they had decided that a particular blood vessel should be given to Marwa, because she was the weaker twin, while Safa, they felt, could better survive its loss. The girls' anatomy made it impossible to divide everything 50-50, so you have to slightly favour one over the other in some decisions about shared blood vessels. There is, Jeelani concedes, an element at that point of playing God.
Meet the amazing team behind Safa and Marwa’s treatment. Their care demanded close collaboration between more than 100 experts at @GreatOrmondSt – one of the only places in the world with the skills and facilities for this procedure. https://t.co/aKrOCMGu3q 🙌🔬 pic.twitter.com/SvDQaCvvBn
— Great Ormond Street Hospital (@GreatOrmondSt) July 15, 2019
"We got the decision wrong," he says. "Safa's left arm and left leg were now weak. I felt awful. What we don't know is, had we done it the other way, had we given Safa the advantage of that vessel, would Marwa have suffered a similar injury, or worse? How I deal with it is by saying, OK, given the knowledge we had, we did the best we could."
"You have a strategy," says Dunaway, "and by and large you stick to that. But there are always surprises."
Theoretically, when they're operating together, there is a separation of labour – Dunaway does all the plastic surgery work, Jeelani does all the neurosurgery. The reality, says Jeelani, is that they work interchangeably, in total collaboration. They spent hours and hours working out how the blood vessels in the girls' brains joined together, which way the blood was flowing in them and in what order they would separate them. It was the most complex operation of Dunaway's career, not because of the actual surgery, but because of everything else.
"Each individual manoeuvre is something we do every week. None of the steps in themselves is terribly complex. What's complex is putting them together in a sensible order, which allows you to separate twins, and all the problems that come with having two people joined together."
What he means is that most surgery doesn't involve two patients at once. With conjoined twins, any drugs you give one are transmitted to the other. Every decision you make about one has a knock-on effect on the other. The moment when they're successfully separated is euphoric, enough to bring a tear to Dunaway's eye, but it isn't job done.
"I was lost for words," says Jeelani. "It was such a huge relief."
Zainab says she wept with happiness and is indebted to the surgeons and Great Ormond Street. Safa and Marwa, now aged two and a half, are having to start from scratch, doing things that most babies began 18 months previously. They've never sat up or crawled, and their muscle tone is practically non-existent. While normal babies weigh around 6.5kg when they start sitting up, Safa and Marwa have 13kg to try to haul into a sitting position, and toddler-sized heads to try to hold up. It's one of the reasons why these surgeries need to be done when the children are as young as possible, along with the fact the younger the child, the better the chance that the brain will completely recover. Dunaway thinks that in the future, possibly even in his lifetime, separating conjoined twins might best be done in the womb.
We’ve an incredible story to share with you: conjoined twins Safa and Marwa have been successfully separated – the first such procedure at @GreatOrmondSt since 2011! Discover their extraordinary story. https://t.co/aKrOCMGu3q 🎉🏥 pic.twitter.com/zePGMMrdIt
— Great Ormond Street Hospital (@GreatOrmondSt) July 15, 2019
Jeelani reckons he's spent more than 1,000 hours of his own time on the case, much of it trying to raise the money. Both he and Dunaway carried on with their normal practice at Great Ormond Street throughout, performing the same number of operations as they did the year before. But they're aware that about a dozen sets of twins are born conjoined around the world every year, and nobody knows what happens to most of them. It's why the pair have now set up a charity, Gemini Untwined, which they hope will raise funds to operate on future sets of twins, as well as becoming a global database of knowledge about them. Around 60 separations have been performed since 1952, he says, but many are never reported and there is no central bank of information about what happens to them. All the data that surgeons usually use to calculate the risks and benefits of surgery simply isn't there: what happens to the children that are never separated? Do they die early? How early? How many go on to lead full, independent lives?
"What happens to the next set of twins we see?" asks Jeelani. "This case took me to the limit. Trying to raise funds seemed like the hard bit, and surgery the easier part. We don't want to be in that position again. We will be asked to help again, and we don't want to help by dealing with bureaucracy and fundraising. We want to be able to help by being surgeons."
The future looks bright for both Safa and Marwa. After their final surgery, they began their recuperation at @GreatOrmondSt – here they are enjoying ‘Twinkle, Twinkle, Little Star’ during a playful physio session! https://t.co/aKrOCMGu3q 🌟🌟 pic.twitter.com/fk3jKbpukr
— Great Ormond Street Hospital (@GreatOrmondSt) July 15, 2019
Safa and Marwa are making progress, and have the potential to make a full recovery. In spite of the stroke Safa suffered, the rest of her brain seems healthy. But progress is slow. They're not yet walking, and Jeelani fears that if they're still not starting to crawl or sit up without support in three months, then things are going to be "difficult". Safa can count to ten and speak short sentences in Pashto, her mother tongue. Their mother hopes to take them home to Pakistan early next year. While her brother and the twins' grandfather stayed in a flat nearby, she slept every night at the hospital. Safa and Marwa have never met their siblings, the eldest of whom is 15.
"They talk to each other over FaceTime," says Zainab. "All the children gather round and we speak to one another. Safa is more lively and chatty than Marwa. Marwa is happy on her own."
The next three months, says Jeelani, will be crucial. But the hope is that, one day next year, Safa and Marwa will go home.
Written by: Hilary Rose
© The Times of London
