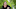Every hour at least one New Zealander dies from cancer.
That's more than 180 every week, or 9500 a year.
Close to 800 New Zealanders who die of cancer each year could be saved if we had Australia's survival rates.
Bowel cancer is a tragic example. Three-quarters of cases are curable if caught early, but only 60 per cent of Kiwis diagnosed with the disease survive – about 1200 Kiwis diagnosed each year will die.
One will be a young Auckland mum who did everything right but was let down by the system at least seven times, including her symptoms being dismissed as "girl problems".
If Kim Girbin hadn't used her mortgage money to pay for a $3500 colonoscopy it's likely she'd already be dead.
"I was young, fit and healthy so I was put on an eight-month waiting list unless I paid, which I did and was seen the next day."
But even then it was too late.
"Literally, they couldn't even get the camera into my bowel, the tumour was that big."
READ MORE:
• Premium - Cancer: $15 million paid to cancer sufferers let down by public system
• Cancer disgrace: DHB, radiology service slammed after 67yo dies after near six-year delay
• Premium - Breakthrough research: Kiwi study finds osteoporosis drug also reduces heart disease and cancer
• Government unveils national cancer agency and $60 million injection into Pharmac
On June 29, 2016, Girbin was diagnosed with stage four terminal bowel cancer.
But that's just part of her story.

For three years the young Auckland mum of one and grandma of three was visiting her GP at least once every month complaining of stabbing pain. She was desperate for answers.
Instead, she was given painkillers and was told by her GP it's "just girl issues".
As the pain began to get worse, to the point where no drug made the slightest difference, she asked her GP for an ultrasound.
The 42-year-old was told the wait would be 10 months as there wasn't anything else wrong with her.
"From the outside, I looked like a fit and healthy person but on the inside, I was in a world of pain."
The former personal trainer paid $350 for an ultrasound. The test results came back normal and it was later discovered the doctor had scanned her pelvis, not her bowel area.
She was sent a letter of apology - but still no answers.
By then, she started to get other symptoms including toilet abnormalities.
"I was a gym person. I'd go for at least an hour and a half each day and suddenly I couldn't walk for more than five minutes on the treadmill and that was at grandma pace."
In June 2016, nearly three years after she first began visiting her GP, she was finally referred for a colonoscopy - but the letter bounced back saying it would be an eight-month delay just to get on the waiting list.

Fearing for her life, Girbin used cash her flatmate had given as rent to pay off her mortgage for a $3500 colonoscopy. She was seen the next day.
She was told she had 18 months to live and began making funeral arrangements.
"It was a huge shock. Being told there's no hope when you've done all the right things, it's devastating."
The failures didn't stop there. She waited a further two months to start palliative chemotherapy and paid $60,000 for life-extending medicine that was publicly available in Australia but not New Zealand.
Surgery to try to remove some of the tumour wasn't an option, she was told.
"They took away my options. No one wanted to touch me despite me wanting to take the risk. Once you fit into their flow chart that's it.
"But I knew my body and I knew it wasn't the end. I wanted to fight."
After she made her case in front of a District Health Board cancer committee, one brave doctor stepped up to perform her surgery.
Part of Girbin's tumour was removed without any significant complication and as a result, her pain lessened.
More than three years later she is still fighting, though she knows her days are numbered.
"I don't know how long I've got left. It might be days, it might be months. I'm basically living in limbo."
Girbin's story is not isolated. In the past 10 months, the Herald has spoken with dozens of patients, many of whom have died or are dying. They shared anguish about similar letdowns. Health advocates say they hear stories like this nearly every day.
Today, the Herald starts a new series examining New Zealand's cancer care, which has been spotlighted by patients-turned-advocates like the late Blair Vining, and is set to be overhauled through a new national agency.
Our reporting will explore:
• How New Zealand's cancer treatment can catch up to countries like Australia and Canada - something that would save about 800 lives a year.
• What will be done to try to close gaping holes in cancer care in some parts of the country that Health Minister David Clark calls "embarrassing for some DHBs", and which mean residents of one region are three times more likely to die from bowel cancer surgery than Aucklanders.
• Concerns from the Cancer Society that an ambitious new national cancer agency could be held back by funding shortfalls.
• What New Zealand's cancer care will look like by the end of next year - and the gaps that are promised to be closed in 10 years' time.
Cancer is New Zealand's biggest killer and is believed to cost our health system more than $1 billion every year.
In the last two decades, our country's cancer control progression has stalled while in countries like Australia and Canada it has accelerated.
New Zealand has one of the worst rates of improvement for cancer survival (75 and under) in the developed world.
This year the Government has come under immense pressure to take action, including a powerful public movement started by Southland dad Blair Vining.

The 39-year-old lived to see the response - a new cancer agency that Prime Minister Jacinda Ardern and Clark promised would help save lives and end weaknesses in our health system.
Advocates, including Cancer Society of New Zealand medical director Chris Jackson, applauded the announcement but are concerned about the lack of detail.
Jackson told the Weekend Herald that the entrenched problems the agency faced should not be underestimated.

Those include workforce shortages escalated by years of DHB's hiring freezes, Māori being 20 per cent more likely to get cancer and twice as likely to die from it, and so-called "postcode healthcare" that means you are three times more likely to die from bowel cancer surgery if you live in Whanganui compared to Auckland.
There have been previous efforts to fix these problems, including the first cancer plan in 2003 and major reforms in 2011.
Without the funding and resources to support the agency and plan, improvement will continue to be stalled, Jackson said.
"We've tried several times to get this right with past health reforms - and now it's third time right for cancer control."
Real targets and timeframes were needed to ensure the Government and DHBs were accountable for delivering goals of the plan, Jackson said. Another condition: a whole lot more money.
"The plan has hit the mark with equity-led, knowledge-driven, and outcomes-focused principles," said Jackson, who's worked as an oncologist at Southern DHB for 15 years.
"But we can't lift outcomes without spending in the key areas identified in the plan to reduce the number of Kiwis affected by cancer and improve survival for those who get cancer."
Clark could not specify how much funding would be allocated to the agency but promised more would be earmarked in Budget 2020.
In an exclusive interview, he said some of the gaps in treatment around the country were "a little bit embarrassing for some DHBs" and must be closed.
Clark also signalled a potentially major overhaul of the DHB structure to help save lives.
"The system is good at doing local stuff and responding to local demands and pressures but it's not as good as it could be, in my view, at sharing learning across the system."
The minister also didn't rule out radical measures like highly specialised centres for complex surgeries, such as pancreatic cancer, that could see patients flown to different parts of the country.
Diana Sarfati, who was chosen as the interim head of the new cancer agency because of her international experience in improving cancer care, told the Weekend Herald this method had made a real difference in Canada, United States, Europe and the United Kingdom.
However, she stressed it was still very early days and nothing had been set in stone.

"The biggest issues when you look at centralising cancer services are ensuring all patients have access to that care and building that into the service is crucial."
She said there was a balance between addressing local needs and taking a more centralised approach.
"The way we would approach this problem is focusing on making sure all outcomes are the same but the way they achieve those outcomes may differ because of population variances or geographic."
Responding to Girbin's experience, Sarfati said it was horrendous and "absolutely tragic", and showed some of the systematic weaknesses that must be overcome.
"I am personally absolutely committed to improving the way that New Zealand manages cancer."
Girbin agreed to tell her story in the hope it will stop others from suffering the same failures.
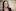
Daily life is a struggle, and one often endured alone. She cannot work, or do other things she loves, like go to the gym.
Her daughters and grandkids are the only family she's got in Auckland and she can't be around them due to her low immune system.
"I rely on my friends for support but they are all working so even that's hard.
"Even getting out of Auckland to stay with friends is a challenge because I am just too exhausted.
"If they found my cancer when I first started to get symptoms I wouldn't have been left with no options, and I wouldn't be spending half my days in bed."