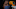In rural Auckland, Marco Canegallo is sore in his bones, short of breath, pain in his chest and nursing a fever.
It began on Friday. On Monday he rang Healthline. It took some hours before he, his wife and their four children are parked up outside a medical centre.
In that parking lot, Canegallo was a long way from his native Italy, yet waiting on a test for Covid-19 brought the events of the past month frighteningly close to his chosen home, New Zealand.
Today, Italy has had more than 31,000 cases and 2503 deaths. It has 2060 people in intensive care. The horror it has experienced and the prospect it might unfold here is awful.
A figure emerged from the medical centre wearing apron, gloves, mask and goggles and carrying swab equipment to carry out a Covid-19 test.
For Canegallo, he's thinking back to the event he attended at which Patient Two and Patient Four were present. He's thinking of a visit from a businessman from Italy last month. But that was too early. No, it must have been his visit to Melbourne.
"I'm so scared," Canegallo said in a conversation during which he had to stop, on occasion, to sob. "Not for me … but if I think of all the people I came into contact with." If he has the virus, how many others did he infect?
Before Canegallo became a successful entrepreneur with cleaning chemical imports and food production companies, he studied as a scientist with microbiology part of his degree. When Canegallo reads about Covid-19, he reads deeply and understands more than many might.
And so his fear of what may come is greater than others might have.
As Canegallo fell ill over the weekend, he read more and became increasingly worried. He started listing in his head those he had met and places he had been.
Italy is a horror story, and this is why Canegallo is speaking. He left his home country more than 10 years ago to create a new life in New Zealand, and he's terrified the same narrative will unfold here.
READ MORE:
• Coronavirus in NZ: Eight new cases, Jacinda Ardern says don't panic
• Hello from Italy. Your future is grimmer than you think
• The Conversation: Coronavirus looks less deadly than first reported, but it's definitely not 'just a flu'
• Coronavirus in NZ: Tourists to be deported after failing to self-isolate upon arrival
Canegallo wants more done. Actually, he wants everything done. It's the least ideal situation for anyone - he reads with enough knowledge to comprehend the possibilities against a backdrop of the tragedy unfolding in his home country.
He wants the border closed, businesses closed, schools shut and for life as we know it to simply shut down. That means bars and restaurants closed, public swimming pools, gyms - anywhere people meet. How long? Until we control the virus, not the other way around. That means stopping the surge, flattening the curve so the health system can take it.
A friend called from Italy: "Make sure your country can still avoid this. Make sure people understand and act now. We sealed off the country one week too late."
Canegallo has been on a campaign for days now, emailing officials and politicians to insist more be done.
He has no criticism of health workers. He is worried for them, having to deal head-on with a contagion all of us are trying to avoid. He wants greater political urgency, to stop the virus and to use that time better equip health workers on the frontline.
He said the current steps were not enough. "I cannot accept it. You have no idea how many people will die because of these delays."
If that's true, we will know soon enough. The proof of it will be stark. In its widespread state, Covid-19 offers just two pathways at the moment - maintaining the status quo as long as possible, or watching it explode across New Zealand.
Long haul to safety
The status quo is a long haul. The alternative is deadly. Otago University professor Michael Baker, an expert on pandemics says Covid-19 is contained in New Zealand and we need to focus on staying at that stage.
Too much, too soon, would overwhelm any health system, he says. "We've consistently underestimated this pandemic around the world. The new norm is going to have to apply for at least a year."
Baker says most activities can continue "in a normal sort of way" but stepping up social distancing, closing school unless needed for children whose parents are essential workers, are among other steps that should be taken.
During this time, he says we need to test and test and test to understand whether it is spreading in our communities. It's not permanent, but it helps understand what we're dealing with.
"You're doing this for a purpose and that's to get the vaccine. We need to do what we're doing, but more so."
"Do you know how grim this will be if it sweeps through the country?" Consider, he says, Covid-19 in New Zealand at a 60 per cent infection rate with 1 per cent mortality.
"It is tens of thousands of people dying," he says. "I hope people appreciate that."
A typical flu season kills about 500 people, he says. "This is like stacking 20 or 30 or 40 flu seasons.
Look at the lessons learned from other countries. There are those who locked down and appear to have been successful at containing it, like Singapore and Taiwan.
Then there's those that did not - Canegallo's beloved Italy - and the virus ran rampant.
It doesn't need to get that bad, says Baker. But if it does, there's a plan.
Getting through together
"If a pandemic came, we would get through it," begins the Ministry of Health document, Getting Through Together - Ethical Values For A Pandemic.
Written in 2007, and still current today, the plan describes a framework for society when dealing with the impact of a pandemic. The framework is a set of values that should be incorporated into our response, written for public understanding.
It is, in effect, a citizen's charter which - if followed - offers a pathway to surviving a pandemic with our humanity, if not our population, intact.
The introduction to the report, written by then-chairman of the National Ethics Advisory Committee Andrew Moore, says: "When faced with difficulty, ordinary people do extraordinary things.
"If we make it clear in advance that we expect a lot of ourselves and from each other, this will help more of us to do extraordinary things. It will also equip more of us to give honest answers when future generations ask us, 'what did you do in the pandemic?'."
It breaks down two sets of values - core ethical principles to guide which decisions we make, and those values needed for good decision-making.
Moore, who is an associate professor in philosophy at the University of Otago, says the research and thought that went into the report aimed to identify values that would speak to New Zealanders.
In deciding what decisions to make, the report offers this:
• Minimising harm: not harming others, protecting each other and accepting restrictions on our freedom for the protection of others;
• Respect/manaakitanga: that each of us matters and should be treated as such;
allowing others to make their own decisions; supporting those who make decisions for others, restricting freedom only as is necessary.
• Fairness: A fair go for all, fair prioritisation when resources are scarce, helping others get their fair share;
• Neighbourliness/whanaungatanga: being there for family, friends and neighbours, working together to meet needs;
• Reciprocity: helping where we can, contributing specialist skills, supporting those who carry extra responsibilities for others;
• Unity/kotahitanga: committing to getting through it together.
And when it comes to the way we make decisions:
• Inclusiveness: working out a decision-making process agreed to by all, taking everyone's contribution seriously and including all - particularly those affected by decisions;
• Openness: letting others know how, what and why decisions need to be made;
letting others know what has been decided and what comes next, being seen to be fair;
• Reasonableness: accepting alternative ways of thinking; reflecting cultural diversity, being fair and making decisions on shared values and best evidence;
• Responsiveness: incorporate others to contribute and to be innovative, being willing to change when the situation changes, allowing decisions to be challenged;
• Responsibleness: Accepting responsibility for decisions and actions, helping others to do likewise.
Ask Moore why such guidance is necessary, he explains: "When we are frightened or alarmed, our impulses are not always our best ones."
The ethical framework was able to be applied to all phases of pandemic response but specifically for a scenario in which "official health services were being overwhelmed" and "if things had to be done, they would get done through community action".
We're not there yet, but neither was Italy when it was able to count cases in double-digits.
Already, transmission of the virus into New Zealand has differed from what the committee expected. It had envisioned a clear separation between "keep it out" and "stamp it out" - the phases during which the pandemic is either simply threatening or in isolated spots.
Watching it unfold, Moore sees both phases happening simultaneously and agrees with the proposition that one folds into the other for as long as community transmission is avoided.
At that point, the speed of transmission is key to preserving our ability to respond to all who need help.
As Moore wrote in the report: "If we were not able to keep out or quickly stamp out a pandemic, it is likely we would make overwhelming demands on our health services as we tried to manage the pandemic."
That scenario plays out in the hypothetical case studies in the ethics committee's report that are so grim they make its plain language even clearer, spelling out life in a pandemic beyond our ability to manage.
Helping, house by house
Volunteers have been ringing houses in an inner-city suburb. This scenario follows a team of four volunteers visiting houses where people could not be reached by phone. It describes their journey door-to-door checking on houses in an inner-city suburb during an influenza pandemic. They are distinctive in reflective jackets with face masks and goggles, carrying thermometers with paracetamol and hand sanitiser.
A notebook records the visits:
First house: Single parent with two preschool children. No influenza symptoms … mother worried about her parents on the other side of town as they are not answering her phone calls. The team leader … says the team does not have the resources to make enquiries for her;
Second house: Elderly couple, husband very ill, wife unable to cope after several sleepless nights. Team calls the 0800 advice line. No ambulance or doctor is available. Team … administer an inhaler … give him fluids and paracetamol … show the wife how to sponge her husband to reduce his fever. A doctor visits later that day with antibiotics. The husband survives and recovers.
Third house: No response to doorbell or knocking, but a dog can be heard barking inside.
Fourth house: Husband, wife and teenage daughter. Both parents are ill, the daughter is coping well … she tells the team the neighbour in the previous house is an elderly man living alone. The team seek police assistance to enter the third house, but no help is available. Two volunteers break in and control the starving dog. They find a male occupant dead in bed. No doctor is available to certify the death, so the team leaves the body where it is for the time being.
Fifth house: Family of recently arrived refugees who speak very little English and have no reserves of food or medical supplies. The wife is very ill, but her husband refuses to let her be examined in bed for religious reasons. A female team member persuades the husband to let her administer fluids and paracetamol … The wife later dies.
Sixth house: Big family living in a small house. Four influenza cases are in two bedrooms. The family has no reserves of food or medical supplies. The parents and teenagers are feeling unwell and not coping.
Seventh house: Professional couple … no influenza. The couple refuse to open the door and talk with the team through the cat flap. They insist they are fine, with ample stocks of food, water, paracetamol and so on and intend to isolate … The team leader asks if they could help the large family next door, but the couple refuse.
And so on, through to House 21. The scenes described were modelled from the 1918 influenza pandemic, but many reflect the stories coming from Italy - the anxious and worried, those left sharing a house with the body of someone they love, shortages of medical help and supplies.
Do we have enough? Does anyone?
Our resources are already stretched. Director General of Health Ashley Bloomfield acknowledged as much when the pressure on Healthline was revealed. He said on Wednesday it was taking seven times the number of calls it did at the same time last year. Staffing numbers are being scaled up but even then phone lines will only triple against the higher demand.
Testing capacity is also under pressure at a time when many thousands of results are needed to properly identify community transmission. There were 500 tests carried out across the country on Wednesday, up from 100 tests a few days earlier. There is capacity to push it up to 1500 tests a day but Bloomfield said doing so would require an extra shift, and there's concern about exhausting lab staff.
Bloomfield said it was expected more cases would be found - and that they needed to be found. Keeping on top of the individual cases avoids the big spike seen in other countries.
It's that surge which threatens our ability to respond. We need time for a vaccine, and time to allow our health resources to cope. Already, said Bloomfield, hospitals are identifying other beds other than those in intensive care units (ICUs) where people can be ventilated. If elective surgery is stopped, it opens up post-operative beds. Additional staff are being trained to bolster ICU staff - it's not just the bed numbers, but those who know what to do when they're filled.
ICU specialist Dr Craig Carr has been stretching resources in Dunedin, where he is Southern District Health Board's intensive care clinical director. He's speaking as chairman of the New Zealand branch of the Australian and New Zealand Intensive Care Society, the role he used when writing to the Government on behalf of ICU specialists, urging greater action.
The travel changes announced last weekend were welcomed by ICU specialists, he says.
At his workplace, there are normally 10 ICU beds. By opening the as-yet-unfinished new hospital extension, it will increase to 22 beds. If elective surgery was cancelled, they become free to handle coronavirus patients.
"If it's more extraordinary than that - and this is why it's so important to keep the (infection) curve flat - we can also start using the theatre recovery unit."
That would give another 10 beds in which patients could be ventilated. And then more from gastroentology, ultimately with a total three or four times the number of beds available. Hospitals across the country, he says, are seeking out every ventilator they can, and trying to get more made.
Carr: "When you face extraordinary circumstances like has happened in Italy, you act differently. Surge capacity can cope with quite extraordinary things.
"The public can do lots for themselves and one another by following the advice - stay home, don't go out and see people, have good hand hygiene, sneeze into the corner of your arm. That will reduce the number of people in the community that have this at any one time."
But that's not all they have discussed. Even with the expanded bed capacity, the unknown is how well, and for how long, we will keep the surge at bay.
If we don't, the surge will overwhelm the healthcare we can provide. As one ICU specialist at a Wellington hospital explained on social media: "ICUs keep people alive who would otherwise die. If ICU capacity is exceeded, people with all types of critical illnesses will die."

At that point, Carr says decisions get made about who gets treated, so as to "do the best you can for the greatest number of people with the resource you've got".
That includes making judgments about who is going to benefit most from treatment, with age and other conditions being part of the decision-making. Moore's ethics committee recommended its framework for these tough calls, too.
Carr: "It's not something we take lightly. The best you can do in the circumstances is to minimise the surge."
Time. We need time for our medical specialists. We need time for a vaccine.
'I just want someone to listen'
Like the ethics plan says, it's "Getting Through Together".
"I think we have to remind people that we as a population have faced adversity before and learned how to deal with it," says Dr Maureen Mooney, a philosopher at Massey University. "There is an end point. People have dealt with situations like this before."
And remember, she says, "after most disasters, you don't go back to what was before, because it's changed".
How much change, asks Canegallo, sick at home, devastated about his home in Italy and worried his new home in New Zealand.
His swabs went to the lab on Tuesday. By today, he still hadn't received his results. It should be faster but it's not. "No one has even called me."
He thinks he feels better than he did a few days ago, but that was to be expected, he says. He's fit and healthy, and informed - he knows what warning signs to look for and when to call for help.
Others do not, he says. Pandemic data shows poorer communities, indigenous communities, are hardest hit. He worries what will happen if coronavirus settles into the most vulnerable parts of our society and wreak havoc.
He runs calculations around transmission and mortality, with curves that rise exponentially. It doesn't take long - as Italy has shown - for that infection rate to outstrip a country's ability to deal with it.
Shut down the country, he urges Ardern. Keep people in their own homes. Close schools. Work from home. Protect vital industries.
"I'm so scared. I'm so ****ing scared because this country will go through its darkest hour in its history.
"We can not waste so many lives. And for what? The economy? The economy is ****ed, it is finished.
"I just want someone to listen to me."
• Canegallo's test result came back on Thursday. It was negative. He is relieved, exhausted and still wanting New Zealand to accelerate its response.