
Pam Abraham's diabetes restricted the flow of blood to her leg so severely that the agony left her "clawing at the walls". Surgeries claimed the toes on her left foot, and an infection nearly killed her. Sadly her case is no longer unusual. Diabetes now causes close to 1000 amputations a year in New Zealand - a loss of legs, feet and toes largely unknown in wealthy suburbs, but increasingly common in other areas. In part two of a three-part Herald Fair Care investigation, Nicholas Jones examines Abraham's case and finds systemic problems in Northland linked to growing amputation numbers and associated deaths.
Her toes had been cut off and she couldn't bear to look.
Pam Abraham's foot was wrapped with bandages, around and around until it resembled a white club. As the dressings were changed, she turned away.
"I couldn't look. If it had been someone else I could have. But it was me, and I couldn't."
Abraham spent more than three months in Auckland City Hospital for problems caused by poorly controlled diabetes, and surgeries eventually claimed each toe on her left foot.
Her trauma is increasingly common. The number of toes, feet and legs amputated because of diabetes is almost 1000 a year, an increase of more than 40 per cent over a decade.
The procedures are the sharp end of a diabetes epidemic swamping the public health system, and the vast majority are avoidable through relatively cheap measures such as fast access to podiatry care and surgical services.
There are bright spots: changes at some DHBs have prevented hundreds of amputations.
However, a special Herald investigation has found basic services elsewhere buckling as demand grows, with years-long delays and other patients simply turned away.
In Northland, where Abraham lives, the health board's own hospital podiatrist complained to the Health and Disability Commissioner and DHB after coming across cases where people died shortly after amputation. One man who wasn't properly referred later showed up with bone showing through a toe. A hastily-arranged amputation came too late.
"I was the last person to see the patient alive before he went home and died," the podiatrist and head of Whangarei Hospital's high risk foot clinic, Steve York, wrote to management in a blistering email.
"So that I know that you are aware of the consequences of these failings, I invite you to come sit in on one of my clinics to look at the impact of these diabetic foot complications, otherwise I can provide you with patient or whanau details so that you can explain to them what improvements have been made."
Abraham narrowly survived her seven surgeries. Her story shows how amputations happen, and what can be done to stop them.
'I didn't have a clue what was wrong'
The pain started on a morning walk. Abraham's daily circuit around Dargaville took her and her dog Spottie twice around the park by the mud-coloured Wairoa river, then back up the hill. Discomfort turned to pain, and the walks shortened.
"I didn't have a clue what was wrong. I thought I could have strained my legs, or I was just getting too old," Abraham recalls. "It was such a short period of time from doing a loop right around Dargaville, to next thing I know I'm on a walker."
The dying tissue was caused by type 2 diabetes, a condition usually brought on by lifestyle and which Abraham has battled most of her 65 years.
The number of Kiwis living with the disease has soared to about 246,000, and another 100,000 are estimated to have the disease but not know it. The epidemic is driven by obesity rates that have trebled since the 1970s. Almost one in three adults are obese, and a further third overweight.
Diabetes happens when the pancreas stops making enough insulin, or it can't be used properly by the body. Without the hormone, glucose (sugar) from food can't get from the bloodstream into cells to make energy.
Too much glucose in the blood eventually ravages nerves, organs and tissue, risking heart attack, stroke, kidney failure and blindness.
Collagen levels in the skin fall, making it more fragile and prone to breaking open. Nerve damage in the feet dims or silences pain, the body's warning system. As a result, patients don't notice injuries like blisters, which fester because reduced blood flow delivers fewer infection-fighting cells.
About eight in 10 diabetic amputations are preceded by a foot ulcer, and are done as a last resort to stop infection becoming fatal.
The other reason for amputation is ischaemia, when a lack of blood supply starves tissue of the oxygen it needs to live. This is what blackened Abraham's toe.
A decade of hospitalisation data shows how amputations concentrate in some communities, but are largely unknown in others. Twenty people have suffered amputations in Dargaville and surrounds since 2008. Thirty-seven in the Far North.
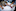
The path to amputation
By August 2017 Abraham's worsening pain saw her return to her GP at the Dargaville Medical Centre again and again, sometimes twice a day. Her blood sugar was too high, her feet icy cold and the GP couldn't feel pulses, a sign of poor blood circulation.
In mid-September her toe was infected and had black edging - her tissue was dying. "Went to bed last night crying in pain," her medical notes summarised. "Presents this morning due to new complete numbness of L lower leg. Pain completely gone, as well as light touch and sharp sensation."
She needed to see a vascular surgeon, but a note in her file was made: "referred to vascular but 3m WL (thought to mean 'three-month waiting list')". Her doctor sent her to a private surgeon, who saw her at the end of September and noted her "black and dusky" big toe and suspected critical ischaemia (obstruction of the arteries).
On October 3 the DHB received a request for a CT angiogram, a test that uses X-rays to show narrowed or blocked blood vessels. In the meantime, her GP had an ambulance take her to Whangarei Hospital emergency department, partly to try to get the CT scan done. She arrived just after midnight but, unable to walk, was discharged at 2.26am on October 11.
The CT scan was done on October 24, and confirmed an extremely dense calcium build-up blocking the largest artery in her thigh.
On the night of October 30 Abraham's husband Bob called 111. The operator heard screaming. Her leg was starved of oxygen-rich blood, and Abraham recalls "literally clawing at the walls".
An ambulance took her to Whangarei Hospital, and she was booked for surgery in Auckland on November 3, but a communication mix-up meant she wasn't sent down.
A visiting vascular surgeon assessed her four days later, and determined the lack of blood flow was critical. "She has been transferred down [to Auckland] urgently," he wrote in her file.
Auckland
Abraham had surgery to bypass the blockage in her femoral artery, but her wound became badly infected and wouldn't heal. Surgeons dropped a bombshell - they might need to amputate the whole leg.
"I was scared. They have told you the news, they have gone on to do their rounds. But it takes you a while to process," she says. "I looked at Bob, sort of, 'What do I do now?' He didn't know. You've just got to do what the doctors tell you."
She avoided full-leg amputation, but soon lost her little toe and some of the foot as lack of blood flow killed tissue. More surgeries followed. (At least half of diabetics who have an amputation will have another within five years.)
Abraham got through with the support of her husband, who took leave from work operating a processor in the Kaipara pine forests. He stayed in Auckland for three months, returning to their son's place in Te Atatu only to sleep and shower.
The couple's story began when Māori boy met Scottish girl on a night out in Auckland. More than 40 years later, they were back in the same city and, with Abraham bandaged and holding on to life, finding new intimacy.
"He was there eight, nine, 10 hours a day, seven days a week," Abraham says. "Everything you do for a newborn baby, he did for me."
Sometimes Bob would slip away and return with a wheelchair. One evening they sat by the carparks and watched the Auckland Domain fill with people and light for Christmas in the Park.
On December 25 lunch was chicken teriyaki from Subway. Bob ate the hospital meal. They felt far from home.
"I actually said to Bob, 'I think this is going to be my last Christmas.'
"I had been there several weeks by then, and I just had this horrible feeling. At that stage I had so far to go in terms of healing. I just thought, oh, I've run out of energy and strength. It's too hard a job."
Four days later Abraham lost the last toes on her left foot.

Avoidable tragedy
Research has estimated more than 80 per cent of diabetic amputations are preventable, if problems like ulcers are detected and treated early - before they get so bad as to need amputation.
All diabetics should have an annual foot examination to check for loss of feeling and any wounds like blisters, and those at high risk should be checked every time they see a health professional.
If a problem is found, the patient should be fast-tracked to see specialists who can get wounds healing and assess issues like lack of blood flow.
Podiatrists remove dead tissue to promote healing, educate patients and families on how to prevent wounds, and contact vascular surgeons if blood flow is critical. Special surgical shoes, insoles, moon boots or casts might be arranged to take pressure off the foot.
Improvements save lives. In Counties Manukau, for example, dialysis patients have avoided amputation after an overhaul slashed the average wait time to see a podiatrist from 42 to five days.
However, in areas including Northland amputations have surged amidst claims of inadequate services and years-long delays.
Documents obtained using the Official Information Act reveal repeat warnings to Northland DHB management by diabetes podiatrist Steve York.
A main concern is the fact that half of type 2 diabetics in the North didn't get their foot check in the past year, including about 1600 people who are at high or moderate risk. Without checks, people generally seek help only when their ulcer or foot disease is well along the way to amputation.
More than three-quarters of Northlanders who had amputations in the past 12 months weren't previously known to York's Whangarei Hospital high risk foot clinic, or were sent for surgery within seven days of being seen because their cases were so urgent. People who need treatment are turning up too late, or not at all.
The result, York recently told a DHB operations group in charge of diabetes care, is busier operating theatres: amputation procedures on Northland residents boomed by more than 50 per cent in the last financial year, up to 72.
That burden isn't equally felt, he warned - the number of Māori having amputations jumped by 58 per cent compared to 12 per cent for non-Māori.
Harm wouldn't be reduced until someone took responsibility, York wrote in a July 2017 email to other diabetes group members: "No one really is accountable because it remains the responsibility of a faceless acronym - it is all our responsibility, but no one is responsible."
Triage problems and delays
Another problem is people not being referred properly, or facing lengthy delays.
Abraham says nurses checked her feet on two occasions several years before she ended up in hospital, but she wasn't sent for podiatry or vascular assessment despite blood circulation problems.
She has now complained to the Health & Disability Commission (HDC), an independent agency set up to investigate complaints about treatment.
Abraham acknowledges her diabetes hasn't been well controlled, particularly in recent years as it became more insulin resistant. However, she believes steps in her treatment came too late.
A Herald investigation has found hers is one of several cases sent to the HDC from Northland alone, including incidents where patients later died. Some complaints have been lodged by York, a member of the Podiatrist Board and a highly respected health researcher.
York's hospital clinic treats diabetics with worsening foot ulcers. Patients judged at high or moderate risk of ulcers, but who don't have one yet, are sent to community podiatry services managed by the Te Tai Tokerau primary health organisation (PHO), which is contracted by the DHB.
Emails show York has repeatedly raised concerns about "commercial interests" leading to "shortcuts or shortcomings".
One complaint centred on two patients York said were referred for community podiatry care in 2015, but not processed until 2017 - over two years later in one case.
York wrote to the chair of the DHB group overseeing diabetes care in August last year, slamming the "repetitive and hollow" claims about fixing patient safety issues that he said had persisted for years.
Audits showed one contracted podiatrist failed to act on 28 patient referrals ranging from 166 to 751 days, York stated. He offered to put the manager in touch with families devastated by amputations, including:
• Whanau of a 39-year-old whose referral to community podiatry was rejected because she had an ulcer, but an oversight meant she wasn't referred to York's clinic. A month later she went to the emergency department three separate times, before being taken to Auckland City Hospital for a foot and later lower leg amputation. She died soon afterwards in hospital.
• The partner of a man whose rejected referral to community podiatry was not re-referred to the high risk foot clinic. He was eventually sent to York by another hospital clinician. Bone showed through a toe, and it was later cut off in Auckland. Three weeks later he returned for follow-up treatment, York wrote: "I was the last person to see patient alive before he went home and died."
Needy patients were being turned away because they had "used up" their allocated treatments, York warned, and he wasn't able to take up the slack.
New guidelines for how patients were treated were a cost-saving measure, he wrote, and failed to put enough focus on the higher risk to Māori.
"Equity and equality are not the same and it's best to ask those who really know the difference ... do what's best for the patient, than for the organisation or yourself."
'Woefully insufficient' care
In response to York's concerns, a DHB-ordered review of community podiatry was done last October by Auckland DHB diabetes specialist podiatrist Michele Garrett and Northland DHB dental officer Neil Croucher. The findings were damning.
Funded podiatry sessions "are woefully insufficient, especially for the high risk group", the review found, and podiatrists - who included recent graduates - were working in isolation and without oversight or support. In some cases they lacked proper equipment, and there wasn't monitoring to make sure their work was good enough.
"We did note however the high level of goodwill amongst the contracting podiatrists, who seemed to be providing additional sessions for the high risk group at greatly reduced private fee rates or sometimes without any remuneration," the reviewers wrote. "This we felt was a clear sign the current publicly funded model of care was not delivering."
Like York, the reviewers were critical of the new treatment guidelines, concluding "they do not appear to be evidence-based", with no treatment strategies such as referral for footwear and surgery.
The workload for York "has reached a point where additional hospital [staffing] is urgently required", the review found, and "variable and dysfunctional" referral processes needed revamping.
GPs needed to be more aware "about the urgency required for an active foot issue to be seen by the hospital podiatry service", reviewers wrote, and new foot screening efforts were needed ASAP.
Te Tai Tokerau PHO says a vast number of changes have been made to improve the service, including strict timeframes for processing referrals. The organisation wrote to the DHB in December 2017 about the two patients sent for podiatry care in 2015, but not processed until 2017. In both cases contact had been lost with the patient, meaning an appointment couldn't be arranged.
"Analysis identified a general systemic failure which was allowing these unfortunate events to occur, often unbeknownst to the PHO," chief executive Jensen Webber wrote, in a letter released under the OIA.
"The future process to allocate, accept and commence treatment will be timely and transparent and patients who have been unable to be contacted will be highlighted quickly ... it is anticipated that this remodelling will eliminate the repeat of patients being 'lost' in the system."
Webber didn't respond to Herald questions about fixing problems highlighted by the review. In releasing the documents, Northland DHB said an action plan and recommendations for podiatry services were being drawn up.
In regards to Abraham's case, the DHB said it didn't believe there were any shortcomings in its care. In a letter to Abraham, it apologised for the "confusion and miscommunication" between hospitals over her transfer to Auckland. However, earlier surgery was unlikely to have made a difference, given "already established necrosis of several toes which would likely have required amputation anyway. The priority was to treat the infection."
The Dargaville Medical Centre declined to answer questions about her case, saying to do so would be inappropriate, even with a privacy waiver.
Asked for an interview, York asked for one to be arranged through his employer, according to the DHB's media policy. He was not made available.

A life changed
Abraham hopes her story will stop someone else suffering.
When the Herald visits her home midweek it is quiet after the happy chaos of grand and great-grandchildren over the holidays. Framed photographs cover the walls - her now-grown boys playing rugby and at the beach, one beaming and holding up a kina.
She makes her visitors tea in a series of careful movements. Each goes against a lifetime of habit and instinct.
"It's your big toe that does your balancing. If I lean where the big toe should be, I just keep going," Abraham explains as she pours. "Simple things, like I open the fridge and go to look down to the bottom shelf and I carry on going, 'Donk', into the fridge."
Bob still helps her shower, and pushes her in a wheelchair around the supermarket. She misses her walks, gardening and the "hundred little things" now impossible.
Still, there's much to be grateful for. Her pain is better. Those children, grandchildren and great-grandchildren whose photographs fill the house. Spottie at her feet. Bob home soon from work.
"We recently had our 44th wedding anniversary," she says. "Well, at one stage I thought, 'I'm not going to have another anniversary, or another birthday, another Christmas'.
"It's been a nightmare. I hope this doesn't happen to anyone else."
Read more
Part One: Our hidden amputation shame
Tomorrow: Revealed - who suffers most

