The senior doctor who accused Te Whatu Ora of a ‘conspiracy’ to avoid disclosing serious safety issues tells ALEX SPENCE he had an ethical duty to take a public stance and that the problems are not confined to his department.
Wearing a white lab coat and gas mask, Dr Bryan Wolf threw his hands in the air and tried to catch the attention of the heavily armed police massing around him.
“I am a doctor!” he shouted. “These are students!”
It was June 2020 and Wolf’s home city of Portland, Oregon, like many across the United States, was being convulsed by civil unrest in the aftermath of the murder of George Floyd.
Every night for about a month, Wolf, then a 37-year-old radiologist and assistant professor at Oregon Health & Science University, joined the protesters from the Black Lives Matter movement, many of whom were students at his university.
When the police began using force — including tear gas and rubber bullets — Wolf helped arrange water, masks, and other safety equipment for the protesters and provided medical assistance to the injured.
He tried to position himself physically between the students and the police, hoping the officers would hesitate to open fire on a medical professional. Wolf was hit multiple times by crowd-control munitions, the projectiles leaving painful marks on his hip and calf.
The violence traumatised Wolf, he would later tell a hearing on police reform at the Oregon state legislature. More than that, he was deeply disillusioned by what he saw as the authorities’ blatant disregard for civil safety and human rights.
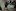
Three years later, Wolf now lives in Hawke’s Bay, where he is a consultant radiologist at the regional hospital and has thrown himself passionately into another cause: Exposing safety risks in New Zealand’s public health system.
As the Herald first reported last month, Wolf is the doctor who accused Te Whatu Ora-Health New Zealand of a “conspiracy” to avoid publicly disclosing unsafe practices after it refused to release a damning report about the radiology service where he is a senior medical officer.
Wolf’s stance against his employer has reverberated explosively across Te Whatu Ora, prompting scrutiny from the news media and external agencies and a flurry of conversations at the top of the organisation. Te Whatu Ora says has taken Wolf’s concerns seriously and is putting significant effort into resolving them.
This week, Wolf had a two-hour meeting with Te Whatu Ora’s chief executive, Fepulea’i Margie Apa, and chief clinical officer, Richard Sullivan, where he challenged the executives to transform what he describes as a system-wide culture of secrecy and denial about patient safety.
It is “common knowledge” among clinicians and health officials that defective systems and processes are putting people at risk in health services across the country, not just in his department, Wolf tells the Herald in his first media interview since blowing the whistle. “But it is not being accurately represented in the public domain.”
Wolf says he told his bosses it would be another “institutional betrayal” if Te Whatu Ora does not become more open about these problems and the consequences for people who rely on health services.
“I think they received it really well,” he says.
Decade of poor performance
Wolf, who is now 40, moved to Hawke’s Bay with his young family in 2021, seeking respite from the conflict they witnessed in Portland. One of the reasons they were attracted to New Zealand was the Ardern government’s handling of the early phases of the Covid-19 pandemic.
At Hawke’s Bay Hospital, he joined a radiology department that was understaffed and overworked. It had an IT system riddled with problems that caused radiologists immense frustration, forced them to adopt risky workarounds, and on some occasions caused significant harm to patients.
In one incident before Wolf arrived, a man in his 70s was found by a CT scan to have a potentially cancerous growth on one of his lungs, but the radiologist’s report did not show up in the electronic system. It was not read by a doctor until more than a year later. The man died soon after.
In September last year, Wolf read an article on the RNZ website about safety risks in radiology IT systems that were occurring in hospitals across the central North Island.
The article was based on a memo by a Te Whatu Ora manager in Wellington, who said there were several common and persistent risks that had a high likelihood of causing “patient death or life-changing delay to treatment”. These included radiology reports not being sent to the doctors who ordered them, and illnesses being missed because scans of different body parts were not linked.
Wolf was alarmed that the response from Te Whatu Ora quoted in the RNZ article said the risks had been mitigated and that it was not aware of any “adverse patient outcomes that may have resulted” from the systemic faults.
That was contrary to Wolf’s experience in Hawke’s Bay, he says, and suggested to him that Te Whatu Ora’s leadership didn’t appreciate the seriousness of the situation.
In October, Wolf sent a detailed 49-page report to Te Whatu Ora’s senior national executives asserting that the IT problems in Hawke’s Bay had not been resolved and that “harm is ongoing”.
Over the next several months, he submitted four more lengthy reports expanding on his concerns and calling for “urgent, serious attention and commitment”.
In response, Te Whatu Ora commissioned a review of Hawke’s Bay’s radiology service. Completed in April, the review found a host of serious technical, cultural, and governance problems that resulted in documented harm to patients and severely affected staff morale.
“Clinicians have endured more than a decade of poor performance, frequent workstation crashes, and unsafe processes within the radiology department,” the reviewers found.
Their report said staff had raised these problems with hospital managers numerous times, but it did not improve. Eventually, staff accepted the unsafe conditions as normal and a culture of “learned helplessness” took root in the service.
The reviewers made 18 recommendations to improve the technical problems, oversight, and workforce shortages. They urged Te Whatu Ora to investigate the impact on patients and the extent to which these issues were happening in other hospitals.
Sullivan, in a written statement, told the Herald six of the recommendations have been completed and the others are in various stages of implementation. A working group has been meeting monthly to oversee progress, which has included upgrading technical systems and reviewing governance measures.
To quantify the extent of harm, Te Whatu Ora is reviewing patient records going back years. “When a sufficiently representative sample has been reviewed, we will be in a position to explain the relative rates,” Sullivan said.
But Wolf wasn’t satisfied. He believed the authority was too slow to act on his concerns, focused too narrowly on radiology in Hawke’s Bay (rather than taking it as an opportunity to root out similar problems across the system), and should have informed the public about what he exposed.
Between April and July, he alerted numerous external agencies to his reports, including the Health and Disability Commissioner, Health Quality & Safety Commission, IANZ (which accredits medical imaging services), and the Chief Ombudsman.
When Health Minister Ayesha Verrall visited Hawke’s Bay Hospital, Wolf handed her a ring binder containing his reports — to the evident embarrassment of his hospital managers. (Verrall has confirmed the encounter and said she asked to be kept informed by officials and expected Te Whatu Ora to implement the reviewers’ recommendations in full.)
As a result of Wolf’s disclosures, IANZ suspended the accreditation of Hawke’s Bay’s radiology service, a largely symbolic step that does not stop it from operating. The HDC wrote to Te Whatu Ora urging it to take “urgent, immediate and transparent action” to resolve the problems Wolf exposed. But all of this was happening out of the public eye.
In May, a journalist at RNZ heard about the review and asked Te Whatu Ora for the report under the Official Information Act. On June 29, Te Whatu Ora declined RNZ’s request on the grounds that releasing the report would identify a whistleblower.
Wolf insists he made it clear on several occasions that he did not expect anonymity and was furious that Te Whatu Ora did not release the report to RNZ. He wrote to the Chief Ombudsman Peter Boshier asking him to investigate what he described as a “conspiracy to defraud the general public of their knowledge and health”.
The Herald obtained Wolf’s correspondence with the Ombudsman and published an article about it on August 14. Te Whatu Ora denied there had been a deliberate attempt to mislead the public and said it acted on legal advice when it rejected RNZ’s request. The authority said it was committed to transparency and reconsidered its decision to withhold the report.
On August 15, it released the document to the Herald and RNZ, making it public for the first time.
In an interview at the time, Sullivan praised Wolf for bringing important safety matters to the public’s attention and said Te Whatu Ora was determined to fix the problems. Sullivan said he was confident Hawke’s Bay’s radiology systems were now “safe and stable”.
Asked about Wolf’s disclosures at a press conference, Verrall said she had been advised by health officials the “immediate safety risks have been addressed” and similar issues were not present at other hospitals that used the same software.
On the extent of harm to patients, Verrall said she had been told four cases had been referred to the HDC for investigation.
Public’s right to know
Watching Verrall’s remarks online, Wolf was again exasperated.
He believed there had been some improvements to Hawke’s Bay radiology systems, but the longstanding cultural and workforce problems identified by the reviewers were still present. And radiologists in other hospitals said they were also experiencing problems with their systems.
Wolf believed it was not just Hawke’s Bay, and not just radiology services, having major problems with defective information systems, and that many more than four people had been impacted.
On August 28, Wolf escalated again, writing to Prime Minister Chris Hipkins and others saying Te Whatu Ora’s public statements had “incorrectly isolated systemic issues to Hawke’s Bay, which victimised a department willing to be an example of reform”. Wolf urged Hipkins to back a public inquiry into what he described as an institutional failure to be transparent about patient safety. (The Prime Minister’s office did not respond to a request for comment.)
On September 8, another IT incident was discovered at Hawke’s Bay Hospital. Because of a problem with transcription software, clinical letters were not sent to GPs in the area for about a month — delaying the release of around 3600 documents. Te Whatu Ora says it notified GPs as soon as it found out, offered support to practices hit by a sudden influx of letters, and has asked to be informed if any patients were harmed by the delays.
Since then, Wolf has kept pushing — including at the meeting with Apa and Sullivan this week.
It is a crusade that some of Wolf’s colleagues, after years of feeling that their concerns were not being heard by management, believe is futile. But Wolf says he is hopeful that it will eventually result in substantial changes.
“They did listen,” he says of the latest meeting. “They do seem to have an intention.”
“I think they’re going to have to publicly admit that their systems are a problem.”
Wolf is not alone among medical professionals in having grave concerns about patient safety. In recent months, we have spoken to many doctors and nurses who fear that the mounting pressures on public health services, including severe workforce shortages, are putting them and the people they care for at risk. Some have gone on the record to express these views. But none have publicly confronted the health authorities as boldly as Wolf.
It is not how he wanted it to play out, he says.
Wolf says he hoped Te Whatu Ora would initiate a “safe” and “compassionate” national conversation about patient safety in response to his disclosures, led by clinicians. He insists he only reached out to external agencies, ministers, and the media when he felt the serious problems he exposed were being minimised.
“I don’t want to be talking to journalists,” he says. “But this is all I have. This is the only way forward right now. It’s very frustrating. It’s sad.”
Wolf worries that there could be professional consequences for taking a stand. But he says he firmly believes doctors have an ethical duty to speak up when their patients are at risk.
As Wolf sees it, he is defending the public’s fundamental right to participate in government decisions, a cornerstone of the democratic ideals he saw being eroded in his home country. He is still the lone figure in a white coat, arms in the air, screaming at the authorities in the name of social justice.
“When you start misinforming the public and taking away their ability to advocate for themselves, that becomes very dangerous,” Wolf says. “It’s a slippery slope.”
Alex Spence is a senior investigative journalist based in Auckland. Before joining the Herald, he spent 17 years in London where he worked for The Times, Politico, and BuzzFeed News. He can be reached at alex.spence@nzme.co.nz or by text or secure Signal messaging at 0272358834.

