Disability bosses say their services are so stretched they have begun to refuse complex clients, adding to a crisis in which an estimated 15,000 eligible people are missing out on funding entirely. In a new report, the providers have identified a funding shortfall of at least $500 million, and are
Disability funding crisis: 'Exhausted is actually an understatement'

Subscribe to listen
Steve and Lisa West with their daughter Ocean, 12, who suffers several disabilities including cyclic vomiting syndrome. Photo / Mike Scott
The most debilitating, however, is cyclic vomiting syndrome, which can see her vomit up to 1000 times in a day.
"When she's sick, not only do we have to clean the house, clean her bed, and try to keep her fluids up, but in that period she wants 20 baths a day as well," Steve says. "And if she doesn't get what she wants, she screams the house down."
The family get some help - a few nights' respite service and a carer for six hours on the days Ocean is at home - but they say every bit has been an uphill battle, and it still barely touches the sides.
While the carers are hard-working, they're not qualified. And because Ocean barely sleeps - and refuses to sleep without Steve next to her - there's hours and hours when the couple go it alone. They say it's caused a huge strain on their marriage, and their life.
"Exhausted is actually an understatement," says Steve. "We are barely functioning. But no one wants to know this stuff. It's awful."
The Wests are among the 60,000 families in New Zealand supported by disability services who, according to a new report, represent a fraction of those who really need help - and who get only a fraction of the help they need.
The New Zealand Disability Support Network (NZDSN) briefing – Enabling Good Lives Sooner Rather Than Later – has estimated at least 15,000 more families are eligible for disability services, but aren't on the books.
It is likely they are disproportionately Māori, Pasifika, poor and rural - excluded by a system which is "complex" and "focused on rationing demand", instead of reaching out and helping people, the report said.
"This has got to stop," said NZDSN chief executive Garth Bennie. "It's high time the Government delivered on its promise to put wellbeing at the heart of all its decision-making when it comes to disabled people, their families and those organisations providing support services."
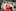
The estimates were based on pilot programmes in Christchurch, Waikato and the Manawatu, which made it easier to access and use the system, and therefore saw more people coming forward.
The number of those missing out on support is one of three major conclusions from the document, which references the Government's disability strategy "Enabling Good Lives".
It also argues there is a $574 million gap in disability funding; and that providers are struggling to keep afloat in an environment that doesn't allocate enough money to meet clients' needs.
Bennie said there was repeated evidence of where clients' needs went up, but their funding stayed the same; and conversely, where their needs stayed the same, but funding was dropped.
Equally, contract pricing had plateaued for two years, while provider costs had gone up.
"It's an impossible dilemma for providers," Bennie said. "Their own boards are getting increasingly strident about taking on people where they maths doesn't add up; or where there will be quality and safety issues."
But at the same time, providers did not want to turn people away. "They know if they do that they're contributing to unmet need. They're completely compromised. Many are saying, 'We don't want to do some services any more'."
The report follows a turbulent year for the disability sector.
In April, the community was horrified when the Herald revealed officials had been asked by the Ministry of Health to find savings of $90m.
They proposed drastic measures including limiting meals and showers for the disabled before ministers caught wind of it and intervened.
In the Budget in June, the Government made a fanfare of the largest-ever increase of $76m to disability services - but it was quickly revealed that it wouldn't even be enough to cover the $83m overspend from the previous year.
Bennie said he was aware there was not a bottomless pool of money, but it seemed only fair to try to right a system that had been neglected for so long.
"We are asking, what is a reasonable taxpayer contribution to a system that does indeed enable a good life?"
Ministry of Health head of disability Adri Isbister said it was correct that more people were accessing disability support and services.
"It's also correct to say cost pressures on disability support services will continue," she said.
The ministry was looking at how it could manage that pressure "into the future".
Isbister said costs had increased for a range of reasons, including more people accessing disability supports and services, availability of new equipment and technology, and legislation changes including pay equity, as well as travel and health and safety requirements.
"We are continuing to work with disabled people, their whānau, carers and providers on opportunities to build a sustainable disability system and ensure services are responsive and relevant for disabled people and their families' needs," she said.
For the Wests, that assurance is no comfort. They have spent more than a year trying to get a door to separate the front of their house from the back, to provide some respite for the parent not "on duty".
It was approved by one agency, and then measured up by another. But then the first agency said the family actually had to go through another agency, at which point Steve gave up.
"That's basically the system," he said. "It's a fight. And you run out of time and energy for fights."
Ideally, says Steve, a scaffolder, he would like to stay home and look after Ocean and get paid for it, with some support. But that's not an option under the current system.
So the family will keep on keeping on - taking Ocean to the pool when she can, helping her make costumes, singing and dancing with her when she's well, and hoping eventually the promise of "a good life" comes true.
"It sounds fantastic on paper, doesn't it?" Steve said. "Our question is - when's it going to happen?"