The Covid-19 crisis has brought the country's top experts to the fore. The virus has now been squashed down to nearly nothing in New Zealand, but scientists are busy working on a range of fascinating projects aiming to help the global effort – and better prepare our health system for
Covid 19 coronavirus: 10 amazing projects - Kiwi ingenuity vs the virus

Subscribe to listen
Global demand for them remains at an all-time high and many countries are scrambling to produce and manufacture as many they can.
Major players like Ford and Dyson have rushed forward overseas, but New Zealand's effort has been one of nimble ingenuity in the Kiwi tradition.
One project by Hamilton-based ES Plastics aims to pump out 100 units of a prototype per day.
Remarkably, the firm's managing director Jeff Sharp managed to develop and manufacture his machine, the RESPirator, within a week.
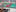
Sharp sought clinical input into the design from two emergency medicine specialists, Dr Martyn Harvey and Dr Giles Chanwai, who also happened to be his neighbours in rural Waikato.
The RESPirator design is based on an old-style pneumatic ventilator that was used in Waikato Hospital until around 2008, and development has been boosted with a $457,000 Government grant.
A grant of $150,000 has also been awarded to another ventilator project with the potential to double capacity in intensive-care units.
That prototype has been designed and tested on mechanical lungs by a group of scientists led by the University of Canterbury's Distinguished Professor Geoff Chase.
After testing and proving it, he aimed to make the software and designs freely available so other countries can make their own.
"We believe this can, and will, save countless lives internationally by doubling ventilator capacity and sparing doctors from having to make terrible end-of-life care choices," Chase said.
"It will provide time for health systems to weather the Covid-19 pandemic storm when major outbreaks occur by increasing intensive care capacity."
In New Zealand, a doubling would mean hospitals could, in the short term, provide mechanical ventilation to something like 460 patients, he said.
The new technology used mechatronics and modern manufacturing like 3D printing to create a system able to support more than one patient at a time.
A new model for Covid-19-hit lungs

Although a ventilator might be life-saving for a Covid-19 patients, the treatment doesn't come without risks.
One University of Auckland scientist is working on a way for doctors to better monitor the lung function of patients hooked up to the machines.
Ventilation can cause lasting lung injury, especially if it's required over a long period.
Yet doctors can't get a precise picture of how patients are responding. "It means they can only respond to significant changes in a patient; without more precise monitoring, the greater the risk to the adverse effects of mechanical ventilation, which can affect the patient for life," said Dr Haribalan Kumar, of the Auckland Bioengineering Institute.
What he and colleagues Professor Merryn Tawhai and Dr Alys Clark have been working on allows imaging of the lungs inside the chest wall, by measuring signals from a belt of electrodes placed around the chest.
Known as electrical impedance tomography, or EIT, it offers an imaging solution for continuous monitoring.
"But EIT has not been taken up widely because it has much lower resolution than other established imaging methods and it can be difficult to interpret," Kumar said.
He pointed out that differences in patients' physiology – be it their age, size, height or underlying health conditions - meant that one lung was not like another, which complicated the translation of measurements into a meaningful image.
But his project, backed by a $150,000 Health Research Council grant, had the potential to personalise the imaging information and improve its clinical value.
"We hope our research will transform EIT from a potentially useful but difficult to interpret technology, to one that is personalised and easy for clinicians to use and interpret."
Unravelling every NZ positive case
New Zealand's tally of confirmed Covid-19 cases stands at just over 1500 – and now scientists want to explore the genetic make-up of all of them.
Through unravelling the genome, or genetic jigsaw, of the Sars-CoV-2 virus, scientists have gained crucial insights into the origin and spread of the virus, and pointed vaccinologists to specific parts of its protein structure to target.
ESR scientists have been sequencing virus genomes at incredibly fast rates – typically within 48 hours – with help from hand-held technology designed for swift processing.
A year-long collaboration between ESR and Otago University will generate virus genomes from every Covid-19 case in the country.
The scientists don't just want to reveal the evolution of all of the cases, but also where they sat inside our known transmission chains.
"When combined with geographic information we will be able to reveal pathways of viral spread - including from the global population - domestically and at the community level," project leader Dr Jemma Geoghegan said.
"These results can be used to direct public health interventions such as quarantine."
Until recently, studies of viral outbreaks have been retrospective - or where spread within a population was only realised after the fact.
"Now however, advances in the next generation sequencing can generate whole viral genomes directly from patient samples within hours of the sample being received."
The Ministry of Business, Innovation and Employment has awarded the project a $600,000 grant.
From grapes to hand sanitiser

What does wine-making have to do with Covid-19?
Scientists are exploring whether grape marc – the skins and seeds remaining after pressing – can be converted into hand sanitiser.
"Using winery waste to produce ethanol for hand sanitiser is untested in the New Zealand context with our varietals," said M.J. Loza, chief executive of the Bragato Research Institute, a wine industry group.
"We haven't had the capability to conduct a study like this in New Zealand until now, with our new research winery opening in February."
The eight-month study, supported with an $84,700 Government grant, aims to deliver ethanol-based hand sanitiser, which will be bottled and donated.
Longer term, the project explores the business opportunity for the industry to turn waste into this new product, including more information on costs, infrastructure needed and technical findings specific to grape marc produced in New Zealand.
The value of wine industry exports are climbing towards $2 billion annually, so the industry is facing a growing challenge to deal with grape waste – Marlborough alone produces about 46,000 tonnes of grape marc each harvest.
"Managing grape marc has probably been viewed as a disposal issue. However, the marc is increasingly being studied for other properties," Loza said.
The industry was continuously looking at alternative uses for grape marc, and the Covid-19 crisis presented an opportunity to learn more about its properties while exploring a potential business case for a new product, he said.
"We know that grape marc is rich in valuable compounds. The challenges lie in finding a new economy for grape marc without creating a bigger environmental footprint, as well as finding a financially viable market for a new product."
Laser-cut face shields

Kiwi researchers have turned to a simple but effective design to make and distribute thousands of face shields for front-line medical workers.
Comprised of a plastic frame and transparent plastic sheet, the shields were developed by Auckland Bioengineering Institute engineer Dr Paul Roberts, with support from MedTech CoRE collaborators and industry partners.
Roberts and his team sprang into action after local clinicians expressed concerns about the lack of personal protective equipment (PPE) in the healthcare sector.
"Face shields are not typically held in stock as part of normal personal protective gear, so clinicians were driving to Mitre 10 and Bunnings to find something to use as face shields."
Roberts used plastic glasses deployed in some hospital EDs as a starting point.
"By mid-March, some EDs were already seeing cases coming through, and wanted a shield that would help protect their whole face."
The face shields provide another layer of protection, to be worn over surgical face masks, to reduce the viral load that healthcare workers can be exposed to.
But, as Roberts cautioned, they "aren't perfect", and in an ideal situation more consultation with users would have enabled design refinements.
"These could also be used by people in a range of contexts, such as ambulance workers, GPs and police."
The face shield was originally prototyped by laser cutting the plastic shield and retrofitting to frames of safety glasses available to some DHBs.
High and urgent demand prompted them to switch to injection moulding frames and stamping the plastic sheet, allowing production volumes of 10,000 per day.
Rapid-fire testing

New Zealand will face a new headache when it eventually re-opens its borders – which is where Ubiquitome's Liberty 16 device could come in handy.
The Auckland company's chief executive, Paul Pickering, said the mobile device would be ideal for use in places like airports, pre-screening international travellers once borders reopen.
Passengers could be tested and would get the result before their flight, indicating whether they should travel or not.
"Covid-19 is the virus of the moment, but there will be others in the future that we'll need to protect ourselves from, so I'd see pre-flight health checks being normalised the same way more stringent security processes were normalised following 9/11," Pickering said.
"We can test and get results in under an hour with the Liberty16. We aim to show appropriate airport or border control personnel could be trained to run the device.
"The Liberty16 software interprets the data so airport personnel just get a result that shows if the person is positive for Covid-19 or not."
The Liberty16 is a real-time PCR (polymerase chain reaction) device that connects via Bluetooth to its own proprietary iPhone App for run set-up, real-time observations and post-run data analysis.
It is battery-operated and, weighing 2.5kg and with a footprint of just over one third of an A4 sheet of paper, it was one of the smallest real-time PCR systems on the international market.
Ubiquitome has already sold Liberty16 into research and clinical labs in Japan, US, Canada, the UK and Germany.
Its latest project has won a $528,927 Government grant.
Pest control to pandemic

A low-cost, smart thermal camera system designed for tracking predators threatening native birds has been repurposed to monitor crowds from a safe distance.
The Cocophany Project, bringing together specialists from the University of Canterbury, the Auckland Bioengineering Institute and Callaghan Innovation, aims to create a device that can measure forehead temperature to within half a degree.
And all without a person having to operate it.
Canterbury mechanical engineers Julian Phillips, lecturer Tim Giffney and Professor Mark Jermy have developed a temperature reference to give a constant check calibration of the devices, which are now under trial and may be rolled out shortly. "If thermal imaging cameras are deployed for temperature screening, this stable temperature reference can help with accuracy," Giffney said.
"We hope this stable in-frame temperature reference could be useful as a simple, rapidly deliverable approach."
Phillips explained that, by putting a stable temperature source in view of the camera, the system could continuously check its reading, and make adjustments.
About 30 soldiers from Burnham, as well as police officers, have been used to test and calibrate the cameras, which could be deployed at airports, hospitals and supermarkets around the country.
A separate project, led by University of Auckland's Associate Professor Nick Gant, is working towards a matchbox-sized body sensor that can be worn under the arm to monitor whether someone has a fever.

The temperature-reading device, dubbed "Nightingale", is designed to protect those most at risk and avoid cluster outbreaks of Covid-19 in places like rest homes.
Gant said it also drastically cut the need for physical contact between frontline medical staff and patients such as rest home residents.
The Cacophany Project received a $914,500 Government grant, and work on Nightingale is being supported with $264,124.
Dropping the bomb

It's called Bomb – and it's helping countries meet ever-growing demand for Covid-19.
Early last year, Otago University's Dr Tim Hore, with Cardiff University colleague Tomasz Jurkowski, showed scientists how to purify genetic material from a wide range of sources using self-made magnetic nanoparticles.
They called their platform bio-on-magnetic-beads - or Bomb – and pitched the do-it-yourself system as a cheaper and more flexible method that could be scaled for processing hundreds of samples at once.
A year later, Canterbury Health Laboratories scientist Dr Kylie Drake was looking for ways to purify the genetic material from the Sars-Cov-2 virus, so that it could be tested for diagnosis.
Typically, this would be done using using reagents supplied in a proprietary kit sold to testing labs.
"This works fine under usual circumstances," Hore said, "but we now know that when a pandemic like this hits, companies are unable to keep up with demand, panic-buying occurs as countries try to secure testing for their people – and inevitably stocks run out.
"Because of the limited reagent supply from companies and precipitous drop in air-travel it was harder and harder to get the required reagents in and New Zealand's ability to test for Covid-19 testing was severely threatened."
So, Hore adapted one of the protocols to isolate genetic material from the virus, before Drake carried out the testing and validation needed to make it a diagnostic test.
The result was a locally developed, efficient and validated diagnostic method to purify the genetic material of the virus that did not rely on foreign life-science companies for supply.
"It gave DHBs a backstop, so that if the supply chain for reagents failed, we were still going to have a method to purify the genetic material from the virus so that it could be tested in patients."
Fortunately however, the supply-chain has held up in New Zealand so the protocol has only been used in limited capacities, testing some frontline healthcare workers that needed rapid turnaround.
Instead, the biggest impact of the work has been outside of New Zealand. Hore and Drake published their protocol on the Bomb.bio website in early April and international interest has been steady since.
"Researchers and clinicians from at least West Virginia and Oklahoma in the US, Cardiff, the Isle of Man, London, Norway, Estonia and Colombia are either using this protocol or modified Bomb protocols to undertake Covid-19 research or to do diagnostic testing," Hore said.
"We have also been invited by the UK's National Health Service Covid-19 Novel Testing Solutions Team to participate in web calls to improve resilience in diagnostic testing and there is even a team implementing mobile testing facilities from shipping containers that uses our method."
Sewer science

As foul as it might sound, what we flush down the toilet has already enabled scientists to capture of glimpse of Covid-19 in our communities.
An approach called wastewater-based epidemiology, searching for traces of certain biomarkers within sewage, has already been used in New Zealand to study other viruses, and even illegal drug use.
Recent studies have shown that live Sars-Cov-2 – the virus that causes Covid-19 – can be isolated from the faeces and urine of infected people, and can sometimes survive for up to several days after leaving the body.
Samples collected in April by ESR were from sites around New Zealand with significant numbers of Covid-19 positive cases in the population, so finding the virus was not unexpected.
But fortunately, only very low levels of the virus were detected in the samples.
By testing wastewater for the Covid-19 virus, scientists will be able to provide information to better understand the virus' presence, prevalence and distribution within our population.
This discovery demonstrates that, although it's possible to detect the virus, more work needs to be done to improve the concentration and detection methods, and design appropriate sampling strategies.
The use of wastewater to detect the virus offers an opportunity to develop an early-warning monitoring tool designed specifically for New Zealand's conditions.
Because New Zealand's infection rates are different from many other countries, ESR's research will also be contributing to the global effort to learn more about the spread of the virus within communities.
ESR is already using data obtained through testing wastewater for a range of other viruses, pathogens and substances to provide communities with their insights.
A home-grown vaccine?
Globally, snpiy 100 candidates are in the works for potential Covid-19 vaccines – and now several Kiwi groups have joined the race.
One, led by start-up Covid-19 Vaccine Corporation, or CVC, is being chaired by the head of New Zealand's largest pharmaceutical company, Jeffrey Douglas.
The group has won a $488,000 Government grant, and also secured $1m in private company funding, with an aim to complete its first human trial of the new vaccine by the end of next year.
"With funding in place, the company is ready to start immediately to develop a vaccine candidate using unique nanobead technology developed right here in New Zealand," CVC chief executive Dr Robert Feldman said.
"This technology will enable us to manufacture the vaccine much faster and more cost-effectively than other methods. The vaccine avoids traditional egg-culture and uses no animal cells in its manufacture."
Feldman said the group wasn't aiming to be the first on the market, "but we are aiming to be better, with an improved response rate and easier, more cost-efficient production".
It's part of a wider vaccine effort in New Zealand, to which the Government this month steered much of a new $37m fund.
Alongside the fresh funding, the Government has unveiled its long-awaited vaccine strategy, which aimed to secure enough doses of a safe, effective vaccine for New Zealand at the earliest possible time.
A key part of that strategy was building capability for making and distributing a vaccine here if it was needed – which Kiwi biotech company Avalia Immunotherapies has already been exploring with a pre-awarded $100,000 grant.
Malaghan Institute director Professor Graham Le Gros – who has been working with top Kiwi scientists and industry partners Avalia and South Pacific Sera on a home-grown effort – said the investment ensured New Zealand and its Pacific neighbours were well positioned.
His group was already eyeing potential candidates, including a virus-inactivated vaccine approach led by Otago University's Professor Miguel Quiñones-Mateu, and a recombinant spike protein vaccine being developed in Dr Davide Comoletti's Victoria University lab.
"Between us and our partners and collaborators we have well over $100m worth of science infrastructure alongside commercial intellect that can be put to good use towards the Kiwi Covid-19 vaccine effort," Le Gros said.
