How an email to a scientist in her pyjamas began an astonishing story — the creation of a groundbreaking vaccine in less than 12 months. Report by Matthew Campbell.
Andrew Pollard is fascinated by the effects of oxygen starvation on the body. The Oxford University professor is a keen mountaineer and once took part in a British expedition up Everest, only to get hit by a storm just short of the summit and be forced to turn back.
That was more than a quarter of a century ago. Over the past year Pollard, director of the Oxford Vaccine Group, has been tackling just as daunting a mission: to develop a life-saving vaccine against Covid-19. It involved "the same logistics, teamwork and resilience", he says.
Approval of the vaccine for use in the UK, which was granted on December 30, was in some ways the summit denied him on Everest in 1994. "It was fantastic, an amazing boost," says Pollard, 55. "It might have been a great moment to hang up our boots and go on holiday, but that isn't the nature of it."
The struggle to conquer a virus doesn't always have a single summit or simple ending. In recent weeks scientists have found the Oxford vaccine is less effective than hoped against a South African variant of coronavirus.
Pollard's team is now climbing a new mountain, striving to refine its vaccine by autumn to get on top of this mutation.
Nevertheless the story of how the vaccine was developed and rolled out at world-beating speed remains extraordinary.
The Oxford team achieved what had never before been attempted: the creation, testing and manufacture of a vaccine at the same time as a pandemic raged. Amazingly it began little more than a year ago.
Part one: Is this 'Disease X'?
Fireworks crackled over London as a new decade dawned on January 1, 2020. People celebrated unaware of the virus taking hold in China and the darkness the coming year would bring.
Sarah Gilbert, a vaccinologist, was at home in Oxford. On New Year's Day, looking at a website dedicated to infectious disease outbreaks, a report on an illness in the Chinese city of Wuhan caught her attention. Working at the University of Oxford's Jenner Institute, Professor Gilbert had been tracking viruses around the world for a long time, hunting for "Disease X" — the unknown virus that might cause the next pandemic. Was this it?
It was not clear at first, she says. "But it looked interesting; a developing story." She kept on checking the website for updates. The disease, it emerged, was a new coronavirus — "even more interesting". Gilbert had already pioneered a vaccine-delivery "platform" that could be adapted to combat many infections. Perhaps its moment had come.
Before trying to develop a vaccine, though, she and her colleagues needed to know the genetic code of the virus. But China had told its scientists not to publicise data and had failed to acknowledge the evidence of human-to-human transfer of the virus — let alone the threat it might pose to the world.
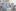
Even so, on Saturday, January 11, Teresa Lambe, one of Gilbert's colleagues, was awoken by a ping on her phone: Zhang Yongzhen, a defiant Chinese researcher, was determined to alert colleagues in the West and had sent them the virus's genetic code. The information had just popped up in Lambe's inbox.
"The genetic code was a bit like the recipe we needed for creating a vaccine," says Dr Lambe, an immunologist and associate professor at the Jenner laboratory. Still in her pyjamas, she got to work on her computer. Her husband, 12-year-old daughter and eight-year-old son did not see much of her for the next two days — or indeed for the rest of the year. "It's all a bit of a blur at this stage," she says. "Working a weekend isn't really anything new any more."
By Monday she and Gilbert were confident they knew what ingredients they would need to create a vaccine. But with no deaths from the disease being reported yet outside China, nobody seemed particularly concerned. That day Kate Bingham, a British venture capitalist with a first in biochemistry from Oxford, was in San Francisco attending a JP Morgan conference on emerging biotech companies. "People then were talking quite dismissively about it," she recalls. "I didn't expect it to become a global threat. It soon did, though."
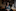
That same week Pollard and John Edmunds, a professor of epidemiology at the London School of Hygiene and Tropical Medicine, were attending a conference on biological standardisation in France — "A slightly unusual group of people," Pollard laughs. He recalls being stunned by what Edmunds, a member of the government's Scientific Advisory Group for Emergencies (Sage), told him about the new virus as they shared a cab to the airport.
"He said this is going to be like 1918, a terrible scourge on humanity," Pollard says. That was a reference to the Spanish flu, which spread around the world at the end of the First World War to kill between 20 million and 50 million people in four waves. "That was the tipping point for me," Pollard continues, "the moment when I realised that this was going to be big."
He called Gilbert, renowned in the field of vaccinology but — in those days — little known outside of it. She told him that she was already working on a vaccine and they agreed to collaborate on clinical trials.
By March Gilbert's team had made a first batch of vaccine. "It's like making dough, but a bit more sophisticated," says Lambe. When they tested it on pigs at the Pirbright Institute, a veterinary facility in Surrey, the results were promising. "We saw that if you give a second dose of the vaccine you get a significant boosting effect," says Simon Graham, an immunologist who conducted the animal trial.
Part two: The first shot is fired
Testing on humans began in April, when the first wave of Covid was at its peak in the UK and some 10,000 volunteers had signed up in a single day. Two Oxford postdoctoral researchers — Elisa Granato, a microbiologist, and Edward O'Neill, a cancer specialist — were the first to receive the jab. "That was a big deal for me," Lambe says. "I walked home feeling a bit overwhelmed. Sometimes it just hits you in the face what you've managed to do. But you can't spend too long thinking about it because your inbox explodes."
Over the next two days the team checked that their human guinea pigs had not suffered ill effects before vaccinating six more volunteers. But then, two days later, a report surfaced on the internet that Granato, the first to be injected, had died. It wasn't true. "Nothing like waking up to a fake article on your death," she wrote on Twitter. "I'm doing fine everyone."
Fake news has been circulating on social media that the first volunteer in the Oxford vaccine trial has died. This is not true! I spent several minutes this morning chatting with Elisa Granato via Skype. She is very much alive and told me she is feeling “absolutely fine” pic.twitter.com/iWAtYaSkRZ
— Fergus Walsh (@BBCFergusWalsh) April 26, 2020
The team accelerated testing. The 400th person to receive the shot was Dan McAteer, 23, an Oxford history student. "There was this weird thing," he remembers. "We had done a week on pandemics in November and the lecturer warned that there would be one coming in the next few years."
At the time the NHS was coming under enormous pressure, and even Boris Johnson, the prime minister, had been among thousands hospitalised with the virus. "I thought I have no skills to offer, I cannot be helpful in that way," says McAteer, "but volunteering is a very minor thing that I could do. You want to feel like you've helped in some way."
Andrew Lloyd Webber, the composer, was another of the volunteers. "I'll do anything to prove that theatres can reopen safely," he wrote on social media.
In the past it could take years, if not decades, to put vaccines into circulation. Now speed was essential. "Nobody had really planned how to develop a pandemic vaccine during a pandemic. That was something we had to do," says Gilbert, the 58-year-old mother of triplets — all of whom are studying biochemistry.
She likes to go out for walks when thinking through problems — "It helps to activate the brain," she says. She went on lots of walks in the first quarter of last year. The big question then, she recalls, was: "How do we go really quickly? What's the fastest route to get into clinical development?"
Maheshi Ramasamy, an infectious-diseases specialist at Magdalen College, Oxford, understood better than most how urgently a vaccine was needed. She was treating Covid patients at Oxford's John Radcliffe Hospital. "They were dying really quickly — and there was nothing we could do," she says. "They were having quite miserable deaths. Alone. It was awful."
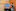
Pollard was gripped by the same sense of urgency. Reports of coronavirus sufferers dying of asphyxiation in some parts of the world reminded him of the oxygen starvation he experienced on Everest. "When you're changing your oxygen bottle," he recalls, "it feels like someone's got their hands round your neck. You can't breathe."
In the middle of April, with the virus spreading around the world and Britain under lockdown after suffering thousands of deaths from it, Patrick Vallance, the government's chief scientific adviser, called Bingham, the biochemist turned venture capitalist. He asked whether she would like to run a task force the government was creating to develop and acquire vaccines against Covid. Chris Whitty, the chief medical officer for England, put it bluntly: "We just need to stop people from dying," he told her.
Part three: How to beat a virus
The history of vaccines goes back more than a thousand years: Buddhist monks in 7th-century India were said to drink snake venom to make them immune from bites. In the UK Edward Jenner, the 18th-century physician after whom the Oxford institute is named, pioneered the "attenuated" vaccine by inoculating an eight-year-old boy with cowpox, a mild virus from the same group of viruses as smallpox, to give him immunity from the latter. Nowadays what was once a tricky process of trial and error has been simplified by scientific breakthroughs.
Two American corporations, Pfizer and Moderna, have backed a new synthetic technology using messenger RNA (mRNA), a molecule that stimulates an immune response. Oxford's vaccine, though also the result of relatively new research, is different. Known as a "vector vaccine", it uses a disabled, genetically modified version of a virus — in this case an adenovirus that causes colds in chimpanzees — as its messenger, or "vector". This "Trojan horse" is used to implant genetic material in human cells, producing antibodies that neutralise the virus. As Lambe puts it: "What happens when the vaccine is injected into the arm is your body thinks, 'That's foreign, that's unusual, I'm going to mount an immune response against it.'"
The Oxford vaccine's advantage is that, unlike the Pfizer vaccine, and to a lesser extent the Moderna one, it does not need to be stored in Arctic temperatures. A normal fridge will do.
The problem in April, though, was how to make enough of it. To save time the Oxford team had begun running tests in parallel, which meant a growing demand for doses that their own manufacturing facility could not keep up with. It was decided to outsource some of the production to Italy.

By the time the first Italian batch was ready for delivery, a European-wide lockdown meant scheduled flights to Britain were grounded. "So we had to charter a plane. It was the only way of getting the extra doses in," says Pollard, who was managing the trials.
That wasn't the only hurdle. The Italians had used a different technique for measuring the concentration of the vaccine, which led to a miscalculation back in Oxford. Volunteers ended up being given what was discovered later to be half a dose of the vaccine rather than a full one. But it didn't seem to matter. The results for that group suggested that a half dose followed by a full one worked better than two full doses.
In fact production delays had meant a longer gap between doses for that group, which turned out to be a blessing. Scientists believe it was not the half dose that made the vaccine more effective but the longer interval between doses. This assured regulators that spacing out the two doses, as the UK has done, would make them more efficient while having the added benefit of allowing more people to be vaccinated with one dose swiftly.
While puzzling over the science, Gilbert and Pollard needed to address logistical problems. If they were to produce enough vaccine for the whole world they would need a commercial partner — and one who would not exploit the pandemic for profit.
Another condition was that production had to start immediately — even before it was known if the vaccine worked — "And that isn't how businesses normally work," Pollard says. They held fruitless discussions with several manufacturers until April 30, when AstraZeneca, an Anglo-Swedish company, agreed to a partnership.
Pascal Soriot, AstraZeneca's suave Parisian CEO, says there was never any question of making money out of a vaccine while the pandemic was raging. "It only works if we do it at no profit," he says, "so we can bring it to as many people as possible around the world."
Even so, profits might be made once the pandemic is over, if annual vaccinations against Covid are needed. In that case the University of Oxford may benefit too. Louise Richardson, the vice-chancellor, was apparently keen not to repeat Oxford's mistake in the 1940s, when it failed to make money after scientists at the university worked out how to turn penicillin, discovered by Alexander Fleming, into a drug that could cure bacterial infections. That work led to the world's first antibiotic.
In May the Oxford team received more good news when the government agreed to buy 100 million doses and chipped in a further £65.5 million to take its total funding of the project to almost £90 million. A complication arose in the early summer, however, when the infection rate in the UK began to fall. Although this was good news, it complicated trials, which relied on people being exposed to the virus.
Part four: 'Viral one-upmanship'
Preliminary results on July 20 had been positive — the vaccine had produced the desired immune response. Even more encouraging was the first evidence, reinforced recently by a new Oxford study, that the jab might prevent people who were already infected but displaying no symptoms from transmitting the virus to others.
The team decided to expand testing to the rest of the world. Soon thousands of people in America, Brazil and South Africa were participating in trials. But the scientists decided not to test the vaccine among large groups of over-65s — who are most at risk of severe illness from Covid — until there was sufficient data showing it was safe in younger people. It was a decision that would come back to haunt them.
While the scientists argued that vaccine development was not a race but a global, collaborative effort, national leaders were scrambling over each other in an increasingly ugly game of viral one-upmanship. On August 11 Russia's president, Vladimir Putin, who was isolating at his residence in a forest outside Moscow, announced in a video conference that he had approved use of the Sputnik V vaccine. The name evoked the superpower rivalry in space during the Cold War. Sputnik was the world's first satellite, launched by the Soviet Union in 1957 — and officials were not shy about wanting Russia to be first with its Covid vaccine. "Americans were surprised when they heard [the satellite] Sputnik's beeping. It's the same with this vaccine. Russia will have got there first," Kirill Dmitriev, CEO of the Russian Direct Investment Fund, told CNN. A Russian TV anchor proclaimed: "Just like 60 or so years ago, headlines around the world again feature the Russian word 'Sputnik'."
Russia was not alone in crowing. Donald Trump, the American president, had set the tone when he announced in May that America was pursuing "the most aggressive vaccine project in history. There's never been a vaccine project anywhere in history like this."
Not to be outdone, Emmanuel Macron, the French president, invoking the "genius of Louis Pasteur", the 19th-century microbiologist, hailed France as a "great vaccine country".
Britain, too, was trying to get to the finish line first. The vaccine task force was backing Oxford and several other contenders in the race. It had infuriated Macron by persuading Valneva, a French biotech company, to manufacture its vaccine in West Lothian, Scotland. Franck Grimaud, the company's chief business officer, says that it contacted several governments when its vaccine project was launched and that "the UK responded the fastest".
Britain also convinced Novavax, a US company, to manufacture in England, a triumph for "little old UK", says Bingham, considering the billions on offer to drug companies under Trump's "warp speed" push for a vaccine. "It was a really big deal," she adds. "The government bent over backwards to enable us to act quickly. We got the deals done early."
As the race intensified, so, allegedly, did the dirty tricks. In September suspicion grew that the Oxford vaccine was being targeted by a campaign to undermine its data and delay approval in America. There was no evidence of rival vaccine manufacturers being involved, but big money was at stake. Shares of Moderna, one of the American flag carriers, rose by more than 700 per cent during the course of 2020 as investors realised that the world would need vast supplies of vaccines.
On September 6 the Oxford team had been forced to halt trials when a participant developed a rare neurological condition. Volunteers often become ill during trials, Pollard explains, and trials are often halted, pending an independent investigation into whether the illness is connected with the vaccine. "It's such a normal thing in trials," says Pollard. "And yet it suddenly became a global news story."
The review did not find any reason to suspect the vaccine was at fault and within days regulators in Britain said the trials could resume. But it took almost another six weeks for the US to do the same.
Then in October Russia was accused of mounting an internet campaign ridiculing the "monkey vaccine". Images appeared of people — including the prime minister — with monkey heads. "It was an unwelcome distraction," Gilbert says, "and just so ludicrous. I can't see why anyone would take them seriously."
Dmitriev, the Sputnik champion, bats away talk of Moscow's involvement. The internet jokes might have resulted from "translation issues", he claims, adding: "It's true that AstraZeneca uses chimpanzee adenovirus [to make its vaccine] and we use human adenovirus. We don't want to comment on them. But we are very proud of the human adenovirus approach."
Part five: 'Jubilation and relief'
In November Pfizer and Moderna announced trial results. Their jabs were 95 per cent effective, prompting jubilation and relief around the world. "That was monumental," says Lambe, "because it gave us a lot of hope that we would be able to get a vaccine and there would be a lot of vaccines, a family of vaccines. It was never really a race to produce a vaccine but a race against the virus."
Oxford's results, released on November 23, were more complicated. The vaccine was 90 per cent effective on the volunteers who were given the half dose followed by a full dose four weeks later, but less so (62 per cent) on a larger group that had got the two full doses. The average effectiveness was put at 70 per cent.
The news, though perplexing, was hailed as a triumph in Britain. Lambe was in her pyjamas again on a Sunday morning when a statistician from the office called to give her a detailed and confidential read-out before the official announcement: "I said 'just tell me if we have efficacy or not' and she said 'yes we do' and I didn't hear a large portion of what came next. It was a bit like the moon landing for me." Dr Ramasamy was ironing her children's school uniforms when the news came through. Her children did a jig around the kitchen table.
On December 2 Britain approved the vaccine manufactured by the American pharmaceutical giant Pfizer, nine days before the US authorities did. The world's first authorisation of a vaccine prompted one of the bluntest expressions of vaccine nationalism when Gavin Williamson, the education secretary, proclaimed on December 3 that Britain's faster approval made it a "much better country" than others.
Then came the moment the Oxford team had been waiting for: on December 30 its vaccine was authorised for use in the UK. "That was incredible for me," Ramasamy says. "At the beginning of the year we had this disease. Then at the end of the year we had the vaccine approved and in people's arms." Another reason to celebrate that day was her husband's birthday — but it had to wait. "I was at work in the hospital."
As a key health worker Ramasamy was offered a vaccine — but she received the Pfizer jab instead of the one she had helped to make. "I felt a bit disloyal," she says. Later her husband got the Oxford shot. "I'm very jealous of him," she jokes.
After more than 100,000 deaths from Covid-19 in Britain and huge damage to the economy, the rapid development and rollout of vaccines offered real hope — and redemption, perhaps, for a government accused of bungling other aspects of its coronavirus response. By the end of January more than nine million people had received at least one jab as sports stadiums, car parks and even Salisbury Cathedral were turned into mass vaccination centres.
The UK-EU spat
Then, on January 25, a virtual meeting of AstraZeneca's senior managers was interrupted by bad news: Handelsblatt, a German newspaper, was reporting that the Oxford vaccine was ineffective in people over 65. AstraZeneca dismissed this as "completely incorrect" and UK regulators say current data does not show the vaccine is ineffective in older people, though at the same time there's only limited data showing it is effective. The earlier lack of testing on over-65s had proved to be a weakness.
The spat came amid a growing row between Britain and the EU over vaccine supplies. On January 22 AstraZeneca told the EU that because of manufacturing problems it could not supply the amount of vaccine it had promised. Already facing criticism for their slow rollout of vaccines, EU leaders were furious, threatening to halt exports of vaccines from manufacturing plants in their territories — the Pfizer vaccine is manufactured in Belgium and while Oxford's is produced at three plants in the UK, some is made in the Netherlands.
As the Oxford team awaited results from trials in America, there was worrying news on February 7 from South Africa, where researchers found that the vaccine provided only "minimal protection" against mild to moderate illness from a virulent new variant first detected there. The study was very small and therefore its findings needed to be treated with caution. Nevertheless, Shabir Madhi, professor of vaccinology at the University of the Witwatersrand, who led the study, called it a "reality check", adding: "We've been somewhat euphoric about the early results of vaccine efficacy. It is unfortunately time for us to recalibrate our expectations."
For Lambe the result was disappointing. "My first thought was 'well, that's a whole lot of work coming my way' and I'd best get on with it. It's another puzzle and we've had a lot of those along the way, so I approach it as before, one step at a time, with speed but also clarity about what we want to achieve — a vaccine that can be used worldwide. That's the end game. Also this time we don't have to look for a partner to help, that's already set up, which is a huge advantage."
Gilbert also is upbeat about the new challenge. "It's easy to adapt the technology, develop a new vaccine, which will have to go through a small amount of clinical testing, not nearly the same amount as we had to go through last year," she told Andrew Marr on his BBC show soon after concerns surfaced about the Oxford vaccine's effectiveness against the South African variant. And there was good news on February 10, when the WHO said the vaccine can be used on over-65s.

The team is also busy with other tests, including a trial designed to see if different vaccines can be used in conjunction with each other, eg whether one dose of the Oxford vaccine followed by a dose of the Pfizer one — or vice versa — creates an even stronger immune response. "My inbox is still constantly pinging," Ramasamy says.
Ramasamy, who grew up in Sri Lanka in a family of scientists, found herself juggling an increasing workload while caring for three young children. "I've been a bit of a rubbish mother over the past year," she tells me, adding that her husband, a full-time cancer specialist with the NHS, had been "brilliant" and taken over "a lot more of the mundane household tasks". Even then, she adds, "I am sometimes conducting conferences on my phone from the car after collecting the children from school".
Lambe, for her part, is looking forward to seeing more of her family this year. "Neither of the children really saw me at all during the first lockdown," she says.
Her daughter's teacher told her recently to "tell your mum 'well done!' ", Lambe says. "My daughter said, 'Thanks, but it was a whole team of people who did it.' It wasn't to put what I did down, but recognition that there's a lot of superheroes out there."
Whatever the coming months bring, the team that produced a vaccine at such speed and under such pressure is unlikely to be forgotten. "When history looks back," says Bingham, who has now moved on from being the government task force leader, "we'll come out very positively as far as vaccines are concerned."
As Stuart Neil, a professor of virology at King's College London, puts it: "We should avoid being jingoistic, but there's a lot to be proud of. It's an amazing good news story"
Additional reporting: Madeleine Spence and Sabah Meddings
Written by: Matthew Campbell
© The Times of London
