In a hospital at the centre of the crisis, nearly 200 babies have arrived since March. Some pregnant women have fallen extremely ill, but doctors are winning battles for their lives and their children's.
The worried doctors stood together after their rounds, weighing the risks. A 31-year-old pregnant woman was in peril, her lungs ravaged by the coronavirus. If they delivered her baby now, it might reduce the strain on her body and help her recover.
But it was more than two months before the due date, and the infant would probably have difficulty breathing, feeding and maintaining temperature and be at risk for long-term health problems. The surgery itself, a caesarean section, would be a stressor for the mother.
READ MORE:
• Covid 19 coronavirus: Around the world - New York 'as terrible as it gets', WHO says it's 10 times deadlier than 2009 flu
• Covid 19 coronavirus lockdown: 5 deaths, 19 new cases, 75 recoveries - Ashley Bloomfield, Jacinda Ardern with latest updates
• Watch Live: Covid 19 coronavirus - How NZ compares to Australia and Singapore; Finance Minister fronts committee
• Covid 19 coronavirus: The six most pressing questions
In the end, the three obstetricians agreed: Neither the mother, on a ventilator, nor the child in her womb was getting enough oxygen, and the best chance to save both was to bring the baby into the world. Today.
"We needed to do something," said Dr. Erroll Byer, chairman of the department of obstetrics and gynaecology at the Brooklyn Hospital Center, reflecting on that morning nearly two weeks ago.
The woman, Precious Anderson, was one of three critically ill expectant mothers at the same time in the community hospital, an unusual circumstance. Byer walked back and forth between the maternity floor and the intensive care unit, checking on her.
Hope, and New Life, in a Brooklyn Maternity Ward Fighting Covid-19This New York City hospital has been one of the hardest hit by the coronavirus. But on the maternity floor, the staff is still welcoming new life. Read the full story: https://nyti.ms/3b1RPN6
Posted by The New York Times on Sunday, 12 April 2020
The obstetrics unit, which delivers about 2,600 babies a year, is typically a place of celebration and fulfilled hopes. But amid the pandemic, it has been transformed.
Nearly 200 babies have arrived since the beginning of March, according to Byer. Twenty-nine pregnant or delivering women have had suspected or confirmed cases of Covid-19, the disease caused by the virus. They have been kept separate from other patients, and medical workers wear protective clothing when attending to them. Hallways where women walked as they endured labor are empty, with the mothers-to-be confined to their rooms. Multiple doctors and nurses in the department have fallen ill.
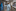
Even healthy pregnant women are anxious. "They don't feel the happiness and joy that many people experience" at this time of life, Byer said. Worse, some pregnant patients who become sick are so scared of coming into the hospital — citing fear of the virus or of being alone — that they have delayed doing so. A few of them have become dangerously ill.
As at other New York hospitals, the surge of new patients with Covid-19 flattened this past week. But the intensive care unit at the Brooklyn hospital had to keep expanding, to nearly three times its original size, and deaths remained high. Nearly 90 patients confirmed or suspected to have the virus had succumbed since March 1. From Monday to Friday last week alone, 30 died. Five staff members have also died. The crisis is not over, Byer and other physicians warned.
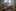
But he is grateful: So far, not one mother or baby has been lost. There have been no confirmed cases among newborns, though doctors are awaiting results for one, according to the chair of paediatrics, Dr. Noah Kondamudi.
Anderson's case has been particularly harrowing. She had been a patient of Byer's for years. He counselled her on getting pregnant after a miscarriage and delivered her sister's children. Day after day, as she struggled for survival, he kept asking himself: Is she going to lose the baby she tried so hard to have? Will her child be left motherless?
During her ordeal, her mother, Doris Robinson, came to Byer's office. "Do you think she's going to make it?" she asked. "Please be real with me."
A doctor and his community
When Anderson, a substitute teacher, finally got pregnant, prenatal visits became a family affair. The baby's father — David Cirilo, who works in security — and often Anderson's mother joined her to watch the ultrasound examinations. The baby was due in June.
Byer was fond of his patient — "a beautiful personality," he described her — who asked questions about her health and how she could address several issues, including obesity, that could affect her chances of getting pregnant. "She was very diligent," he told a reporter.
On Thursday, March 26, when she was feeling sick, she called Byer. He asked her to visit the obstetrics clinic, but she said she was frightened to come to the hospital. Besides, she told him, it was probably just her asthma acting up.
A day later, she had little choice. She arrived at the hospital coughing and labouring to breathe, unable to get out a full sentence. Byer told her she probably had COVID-19 — "she was classic" — and admitted her to a special area of the labor and delivery unit where four rooms at the end of a hallway had been designated for pregnant patients who were infected with the coronavirus or believed to be.
By the next day, the maternity team was unable to keep her oxygen levels high enough, and she was transferred to the ICU. "She was just getting too short of breath," said Dr. James Gasperino, head of critical care. Within 24 hours, she was on a ventilator.
"She tried for so many years, and now she's finally pregnant and happy and things are going well, and it just happens that this pregnancy takes place with this epidemic," Byer lamented. "Those are the things you have no control over."
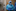
Byer, 51, is the son of an obstetrician-gynaecologist with whom he delivered babies and operated many times, starting when he was a resident at the nearby Long Island College Hospital, where his father practised. His mother is a nurse. One of his sisters is a midwife. His wife is a pharmacist.
He studied at Howard and Syracuse universities and has worked at the Brooklyn Hospital Center for 20 years. He was drawn by its academic programs, he said, and because he "liked being part of the community." Growing up, he had attended a high school for a while near Fort Greene Park, just around the corner from the hospital.
Byer wakes up at 5:30am, preparing for his day dealing with the coronavirus crisis. On his iPad, he checks what has happened overnight — looking at the websites for the Centers for Disease Control and Prevention, Johns Hopkins University and the New York Health Department to see if there are any new recommendations and assess whether the city is reaching its peak patient load.
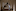
He keeps an eye on the data. Several small studies have been published about the coronavirus in pregnancy. Babies have been found to be infected in a small minority of cases but have generally fared well. While some hospitals separate new mothers with Covid-19 from their infants, others, including the Brooklyn Hospital Center, allow mothers to be with their newborns and nurse them; the virus is not believed to be transmitted through breast milk. They are instructed to take precautions such as wearing masks and gowns and keeping their hands clean when having contact.
Pregnant women are thought to be at a similar risk for severe illness from COVID-19 as other people. But Byer said that more research was needed — particularly in communities, like Brooklyn, where obesity, diabetes and hypertension are common among expectant mothers.
The sound of a heartbeat
Last Monday, three doctors in his unit were out sick. One tested negative for the virus and would be back soon.
Byer and others discussed whether they had enough staffing and supplies, particularly protective equipment. "It's this constant feeling: Is this shipment going to be enough for the next few days?" he said. "It's really a day-to-day thing."
He had two operations that Monday: a planned C-section and assisting with surgery on a patient with a large mass in her abdomen. Before that he had rounds, on which all the cases in the obstetrics and gynaecology service were discussed.
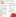
One of the inpatients on the maternity floor with Covid-19 was Basharrie McKenzie, who had been on a ventilator in the intensive care unit, overlapping with Anderson and a woman who was 28 weeks pregnant and later recovered without an early delivery.
McKenzie, 36, was born in Jamaica and came to the United States as a teenager. She has three children and works in medical coding at another Brooklyn hospital, where she believes she picked up the virus. At first, she thought she had a cold. Her 11-year-old daughter brought her juice made from carrots and beets to treat it.
Nearly three weeks ago, on a Tuesday, she was having trouble breathing. Like Anderson, she was prodded by her obstetrician to come to the hospital when she fell ill, about three months before her due date. The physician, Dr. Amber Ferrell, was alarmed when McKenzie called and was so short of breath she could barely speak. Ferrell alerted the intensive care team.
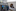
McKenzie was admitted to the hospital and was scared to sleep for fear of never waking up. She watched staff members go in and out of the room next door for a patient she believes died.
By that Friday, she had developed acute hypoxic respiratory failure — not enough oxygen was getting into her blood, which meant the same was true for her baby. She was put on a ventilator.
A day later, drifting in and out of consciousness, she felt certain that the medical staff was trying to kill her. In a panic, she pulled out her breathing tube. The doctors decided to see if she could maintain her breathing off the ventilator.
In Room 11 of the ICU two days later, she saw a physician in a white coat, Gasperino, pass by and give her a thumbs-up. It gave her hope. She returned the gesture with two thumbs and a smile. But she was still breathing rapidly and had a tube under her nose delivering a high flow of oxygen.
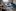
"I'm a little worried," one of the ICU doctors told Gasperino when the team gathered to review patients that morning. The physicians agreed to give McKenzie another day to improve in the ICU.
McKenzie praised God, she later said. Her sister, a pastor in Toronto, asked for prayers to be said for her. Slowly, her condition improved. She eventually left the ICU, where the great majority of Covid-19 patients have not survived, and was moved to a special isolated room in the maternity ward.
Alone — no visitors were permitted except for women giving birth, who can have one — she kept herself occupied by browsing Instagram and FaceTiming with her children, including her 3-year-old, Aaliyah McKenzie. It had been a tough year for the family, with four relatives dying in the previous six months.
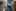
Last Monday night, Angela Lewis, a maternity nurse who has worked at the hospital for three decades, put on an N95 mask, a blue plastic gown, gloves, bootees and a face shield to enter McKenzie's room. She said she had received no specialized training for caring for coronavirus patients. "Years ago, we were taught how to use the PPE and the hand-washing and everything. Covid is the same; you have to apply it. You just be a little bit more careful," she said. "And pray, pray."
The nurse strapped a monitor around McKenzie's belly. The sound of her baby's heartbeat filled the small room.
Lewis returned 30 minutes later, put on protective gear again and checked McKenzie's vital signs. She was breathing without assistance. Her temperature was normal. "No contractions? No cramping?" the nurse asked. She folded up the printout of the baby's heart rate.
The next afternoon, McKenzie gathered her belongings. As she headed out of the unit to go home, one of about 80 coronavirus patients discharged last week, she caught sight of Byer and the nurses.
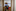
Keena Samuels, the charge nurse of the maternity postpartum unit, said goodbye as McKenzie wept. "You're going to be just fine," Samuels said. "You're going to come back and deliver a healthy, beautiful baby." She added, "You made it!"
'What more can we do?'
In the ICU, Anderson's condition was tenuous.
"You're seeing her not really getting significantly better, even though she's intubated and ventilating, and we had to figure out what we could do," Byer said. He conferred with two other doctors, specialists in both obstetrics and maternal-fetal medicine. Continuing her pregnancy, they concluded, could further compromise her lung function.
"I was thinking: 'What more can we do? Is she going to see her baby?'" Byer recalled.
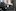
The ICU doctors also believed that delivering the baby might improve Anderson's condition. "My gut feeling was that she would have more of her lungs to fight with," Gasperino said. They prescribed two doses of steroid medications, given 12 hours apart, to help reduce the risk of breathing problems in her baby.
At the ICU morning report two weeks ago, a doctor presented her case: "She's going to go for C-section." The surgery took place around midday. Not long after she was wheeled in, Anderson became a mother. Her baby boy weighed 3.7 pounds.
A team from the neonatal intensive care unit immediately began tending to him. He could not breathe well on his own and required a ventilator.
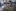
Anderson, unconscious all the while, was taken back to the ICU. There was no significant improvement for days. Byer and Anderson's family were deeply worried.
"Because Covid is such a new and novel virus," the doctor said, there is no way to know what the outcome will be in an individual patient, "even though you've tried everything you possibly could."
The ICU staff received special approval to try the experimental antiviral drug remdesivir with Anderson, according to Gasperino. In a study of 58 severely ill patients published last week in The New England Journal of Medicine, the majority of those given the drug showed improvements, but there was no comparison group, so the significance was unclear.
Last Monday afternoon, Byer went to see his patient in the ICU. "How's Ms. Anderson doing?" he asked one of the critical care doctors.
• Covid19.govt.nz: The Government's official Covid-19 advisory website
She no longer needed the ventilator, which had just been removed, he was told. "Very nice," the obstetrician responded. "Very, very nice."
When he stood outside Anderson's room, she opened her eyes and patted her belly as if she thought she was still pregnant. He gave the still-groggy patient a wave.
He called her mother, Robinson, to report the good news. "She knows she had a baby, right?" Robinson asked.
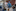
Two days later, Anderson would tell Byer her baby's name: David, after his father. On a tablet, Byer connected her from the ICU by video to the neonatal intensive care unit. The infant's condition had been improving.
"Oh!" Anderson said. "He's asleep."
"He's taking the bottle well, sucking well," Mary Godineaux, senior director of nursing for maternal-child health, said from the baby's bedside. "He's so handsome, Precious."
Anderson asked when he could go home, and Byer said he had to gain weight.
Looking at her son, the new mother smiled and cried at the same time. "Hey," she said. The child opened his eyes and wriggled. "There you go. Hi."
Written by: Sheri Fink
Photographs by: Victor J. Blue
© 2020 THE NEW YORK TIMES
