This week junior doctors accepted a new pay settlement, signalling an end to their collective agreement disputes. It included a pay rise in line with other multi-employer collective agreements - for a two-year term from April 2019 - and a lump sum payment. Their five strikes in the first half
Lakes DHB staff strike 10 times in five months, 226 procedures postponed
Subscribe to listen
The Lakes District Health Board was faced with 10 strikes in the first five months of the year. Photo / File
In the first five months of the year, the DHB was faced with 10 separate strikes as employees negotiated their employment terms and conditions.
The board area covers Rotorua, Taupō, Tūrangi and Mangakino.
Five strikes carried out by Resident Doctors Association's junior doctors, and one by midwives in the Midwifery Employee Representation and Advisory Service Union, were held nationally.
The other four strikes were carried out by anaesthetic technicians in the Apex union and were limited to the Lakes DHB area.
Senior medical officer overtime and costs from other clinical staff, supervisors, meals, stationery and advertising contributed to the bill.
The health board had not recorded specific costs relating the other union strikes so was unable to say how much had been spent.
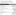
One hundred patients were affected during the anaesthetic technicians' strikes (11 from January 23 to 24, 15 from January 25 to 26, 53 from February 18 to 23 and 47 from April 8 to 16), as well as 126 during the resident medical officers strikes (24 from January 15 to 17, 30 from January 29 to 30, 27 from February 26 to 28 and 19 from April 29 to May 4).
These were patients with confirmed dates that were postponed and not necessarily the total patient volume affected.
During the technicians' strikes, nine patients were transferred to an alternate healthcare provider including the Bay of Plenty DHB, Waikato DHB, and Southern Cross Hospital Rotorua.
The health board was unable to provide the cost of the transfers or how much it had spent trying to settle with anaesthetic technicians, medical officers, and midwives.
The health board's February financial report to board members stated revenue from inter-district flows of patients (IDF) were down on budget by $237,000 "at least partly attributable to anaesthetic technician and RMO [junior doctor] strikes".

This report also said industrial action that month partly contributed to treatment disposable costs being $102,000 less than budgeted and costs from implants and prostheses being $94,000 less than budgeted, due to lower surgical volumes.
Health board chief executive Nick Saville-Wood said it was "very pleased that a number of the health-sector claims have been settled in recent weeks".
"Industrial action is stressful for all parties and during such action, the over-riding priority for the DHB is to ensure that all patients who present to the hospitals with an acute illness are cared for in as safe an environment as possible."
He said for other patients (presenting for non-urgent care), the "industrial action required extensive rescheduling of outpatient appointments and reorganisation of theatre schedules in order to allow procedures on some cancer patients to proceed".
"Some of the catch-up work on elective surgery and outpatient clinic appointments arising from strike action in the first half of this year is still being progressed."

Jill Ovens, the spokeswoman for the midwives' advisory service, said their one-day strike in February followed two weeks of two-hour strikes twice a day in November and December, two days of mediation and weeks of facilitation in the Employment Relations Authority.
"During the strikes, midwives continued to provide life-preserving services. Because midwives can't be replaced by other health professionals, most midwives who were rostered on during the strikes were available on-site to work."
She said this approach balanced patient safety with employees' right to strike, "but midwives were frustrated that so few were able to participate".
Ovens said that because most births cannot be postponed, the DHB was unlikely to have incurred additional costs as a result, besides some elective inductions of labour and elective caesarean sections that may have been postponed.
"The biggest impact was on senior staff who had to manage rosters during the strikes to meet agreed life-preserving staffing standards."
Neither the doctors' association nor Apex responded to multiple requests for comment from the Rotorua Daily Post.
This month, the Rotorua Daily Post reported the health board's overall deficit was forecast to grow to $10m in the upcoming financial year reports.