Pain is the No 1 reason we visit the doctor, according to a new study. A University of Otago researcher says pain is a big problem in New Zealand: we have little research on the condition and patients have difficulties accessing treatment. Causes of pain are wide-ranging and treatments can
Are you in pain? You're not alone - so what hurts and what helps?
Subscribe to listen
Memphis Robson-Frentz has lived with pain for 20 years. PHOTO / GEORGE NOVAK
Pain was isolating and depressing, she says.
"You feel like the only person in the world with pain ... you feel selfish, limited in your capacity to do life, to have to say no to things you want to say yes to."
Still, Robson-Frentz says she's strong-willed and pushes through pain. She opened a backpacker's in Tauranga, mostly delegating management to staff.
She moved to Katikati and says the peace she feels in the countryside with her horses has helped her health. So has a low-dose of nortriptyline, which is used to treat nerve pain, plus a whole-foods, low-sugar diet, massage with Reiki, hot baths with Epsom salts and meditation and Cannabidiol, or CBD oil.
CBD is a prescription medicine in New Zealand. "If it provides relief, you'll do it," she says.
Despite medications and non-drug therapies, Robson-Frentz says life is still a struggle.
"It's a mental battle every day between your body and your mind. Your mind says you have this and that to do, and your body says no, you're not. You force yourself to do the things you need to do, but it comes at a cost."
'Stealing People's Lives'
An editorial in the December 2018 New Zealand Journal of Medicine attempted to raise awareness of pain as a societal problem. Dr Nicola Swain, Associate Professor in the Department of Psychological Medicine at the University of Otago, says pain is the number one reason why people visit their GP.
"Pain is stealing people's lives. As we live longer and are more healthy, pain is an increasing issue."
Swain says the World Health Organisation lists pain as six of the top eight health conditions causing the most loss of life – including lower back pain, arthritis, migraine and various musculoskeletal pain.
Researchers including Swain say pain is a big problem in our ageing population, and persistent pain, defined as pain lasting at least six months, affects about 20 per cent of New Zealanders. She says patients often struggle to be heard by health practitioners.
"You can't see pain – two injuries that look the same on scans can cause completely different levels of pain," she says.
Swain and her colleagues outline key factors about pain, including that pain is always real, despite the fact patients continue to be characterised as "malingering" or "attention seeking" and judgments are made about drug seeking or illness behaviours.
Other factors include:
• Persistent pain and acute pain need to be treated differently. There have been calls for persistent pain to be considered a disease in itself.
• Biomedical treatment has limited effectiveness.
• There are ethnicity and gender differences in perceptions and experience of pain. Pasifika and Asian populations are less likely to report pain than Europeans. There are also differences in the way men and women experience pain.
• Pain education is lacking.
Research about pain is lacking as well, according to the study's authors.
Not in her Head - Alison's Story
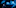
Alison Waa says she's been on medication for chronic pain in her left elbow since 2004.
The Rotorua caregiver says repetitive motion from her job at a Wellington supermarket caused her injury. She saw one specialist who recommended an operation. Another referred her to a pain clinic.
"He said, 'I'm going to touch your arm exactly where the pain is.' I started frowning and sweating. He said, 'You do have pain, it's not in your head'."
Waa says during those first eight months, she struggled to get health care providers to accept her pain as real, despite the fact she dropped from size 12 to size 8 in two weeks and could barely sleep or eat.
"My arm was blue and cold. I said, 'Is my arm dead?' because it doesn't do anything. If it's dead, cut it off because it's not going to help me; it's just more weight."
Waa kept her arm and says she endured a series of cortisone and lignocaine injections that didn't help, but a prescription medication called gabapentin, often used to treat nerve pain, did. She gradually lowered the dose because at higher levels, Waa felt sick, tired and fuzzy.
Her son was 8 years old when she started her pain journey, and she needed to be present for him. She used to study Tikanga Māori, but says concentrating was difficult. "With pain, it can stop me being able to think."
Today, the 47-year-old works as home help for elderly clients, many of whom have Alzheimer's and dementia. She does everything from changing bags of waste to supporting patients who need to be moved.
"There is no light duties in my job."
Waa says her own pain helps her relate to clients. "I get told all the time I'm the most gentlest carer they've ever had, and I go 'it's because I understand pain'."
Waa says a pain specialist in Rotorua 12 years ago asked if she wanted to try medicinal cannabis. She did, but couldn't afford the $400 price tag. These days, pain is unpredictable and the way to get through it, says Waa, is keep going.
She's also a cancer survivor and has found help through Aroha Mai Cancer Support Services. Beyond that, Waa knows not to use her left hand to hold anything heavy or fragile. And she never misses a dose of medication.
"It's taken me the next 13, 14 years to be able to live with it where it doesn't control everything anymore. As long as I play by the rules, it'll behave."
Pain Specialists in the Bay
The Bay of Plenty District Health Board schedules three chronic pain management programmes (PMP) per year. Numbers from last year show a rise from 2013 - 29 patients were involved with the PMP programme in 2018, compared with 23 five years ago. The PMP is three days a week for three weeks, followed up with two refresher days and phone consultations.
Acting business leader - surgical, anaesthesia & radiology services Dorothy McKeown says the current approach towards managing chronic pain is the bio-psychosocial model of pain management.
"This means that, along with biomedical treatments (medication, operations, injections), the psychological and social aspects of chronic pain are also managed."
In addition to pain specialists, physiotherapists, psychologists, nurses and occupational therapists are also involved in care.
"Strategies such as relaxation techniques, mindfulness, massage, yoga, cognitive behavioural therapy and exercise appropriate to the patient are used."
McKeown says new evidence shows virtual reality programmes can also be beneficial.
McKeown says medication continues to be important in pain management to allow patients to function. Primary drugs used are simple analgesics (paracetamol/ibuprofen) and another class of drugs which act on neurotransmitters.
"These drugs, which were originally anti-depressants (amitriptyline/nortriptyline) and anti-convulsants (gabapentin/pregabalin), have been found to also work on neurotransmitters, which affect transmission of pain."
While new programmes and over-the-counter supplements claiming to help pain are multiplying, DHB clinicians advise patients to use treatments that have a valid scientific basis.
McKeown says, "The more that is understood about pain the more complex we realise it is."
She says even though there's a lot of interest in medicinal cannabis in New Zealand, evidence is insufficient to recommend it as a treatment for chronic pain.
Another provider, Habit Group, provides pain management services for ACC clients alongside the DHB throughout the Bay of Plenty. Habit also takes a multidisciplinary approach, working with specialists including social workers, dieticians, registered nurses and pharmacists, in addition to other medical specialists and care providers.
Habit Lower North Island clinical services manager and physiotherapist Naomi Faulknor says the service emphasises early intervention to avoid potentially harmful approaches including unnecessary opioid or other medication as well as unnecessary surgery.
She says evidence shows for most chronic or persistent pain conditions, an effective management programme includes physical activity, sleep assessment and intervention, psychological approaches, relaxation/mindfulness and mentoring.
"There is no one technique but a combination of interventions, specific to the client's needs that is the most effective approach."
Faulknor cites statistics showing about 30 per cent of people say they get pain relief from opioid medication for non-cancer pain, with a 30-50 per cent pain reduction at best, the same level of pain reduction as paracetamol and ibuprofen. That's taking pain from a 7 out of 10 (with 10 being the worst pain) to a 5 out of 10.
She says no evidence supports opioids long-term for chronic, persistent non-cancer pain.
"Evidence also shows that for most people opioids are not safe due to significant side effects in addition to the social costs associated with the increasing use of opioid medication."
About 50,000 people die each year in America from opioids, causing President Donald Trump to declare an epidemic. Drugs in the opioid family include morphine, codeine, tramadol, fentanyl, methadone and heroin (the last one is illegal).
Figures released by the New Zealand Ministry of Health earlier this year show 530 people aged 60 or over are getting opioid substitution treatment. Experts say many more people likely have dependence but have not sought help.
Tauranga-based clinical pharmacist Pauline McQuoid, who works with Habit, tells Bay of Plenty Times Weekend our region has some of the highest rates of opioid use per capita.
McQuoid analysed national data from the Health Quality & Safety Commission which pulls information based on prescriptions dispensed by pharmacists.
"We have the highest rate of prescribing for oxycodone and the second highest of fentanyl."
McQuoid says it's unclear why the rates are so high. She says some doctors have said it's because we have a hospice, cancer patients and a higher-than-average population of older people, but other regions have those factors, too.
"Until you can pin down the data and say no, you are prescribing this much, they tend to think that it's someone else's problem."
McQuoid says medications such as opioids work differently for acute pain like a broken than in someone with chronic, long-term pain, because the two types of pain behave in distinct ways.
"We also know if we keep people on these things [opioids] longer than they should be on them, then a: the effect wears off and they don't work as well and b: we create a problem by getting people dependent on them."
'It's given me my life back'
One woman's success story
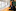
Many pain sufferers we've spoken with say they've tried a range of non-drug treatments for pain. Belinda Hansen of Te Puke is one of them.
Hansen was diagnosed with fibromyalgia seven years ago. She says chronic pain is exhausting, isolating and limiting. Widespread pain caused her to quit her job as a youth worker and stop studying mid-way through a degree in public health.
"Sometimes just touching my skin would hurt. The best way I've been able to explain to friends is it's almost like having either a toothache or earache in your whole body."
She tried prescription pain medication, but Hansen says it was short-acting and she didn't want to keep taking drugs. So she saw a naturopath, osteopath, had massage, went swimming and did acupuncture.
"I spent thousands of dollars over the years to try and find relief - long-lasting relief to an illness I didn't understand. There were times I was really low and had some suicidal thoughts, because it felt …" Hansen's voice catches and trails off.
Fibromyalgia has no cure, and for a while, the 35-year-old saw no way out.
"I felt like it [suicide] was the easier option. At least I wouldn't be in pain any more. But luckily, I'm quite a strong-willed person and they were only ever fleeting thoughts."
Hansen sought counselling when she was in despair. Eventually, she turned to a programme she'd heard of several years ago.
She got a grant from a community trust to attend a three-day workshop for something called the Lightning Process. It's brain therapy Kiwi providers advertise online costing around $1300 to $1500.
The treatment is unfunded in New Zealand and the UK. The scientific community has been skeptical of the programme, though one UK study of 51 children with chronic fatigue syndrome aged 12 to 18 found the method reduced fatigue and increased attendance at school. The process focuses on using simple exercises, movements and gestures to help stimulate recovery.
The UK study's lead author says more research is needed to learn if the same results could be achieved again.
Hansen, however, says the programme changed her life.
"After day three of training I walked around the Mount, feeling like I'd come alive again. I got to the end and burst into tears and said, 'I've got my life back.' I'm surfing again and rock climbing and going on trips with friends and kayaking. It's given me my life back."
She's starting a floristry business and pastors at her church, things she felt she couldn't do before.
"Now when I have pain I'll say my back feels strong, I feel strong, my back is comfortable and I'll say the positive things I prefer to be feeling and over time my brain has gone, oh, that's how I feel."
Hansen says she no longer feeds negative thoughts but doesn't want anyone to think pain is "all in their head".
"You haven't made this up. At some point, there was a trigger that created unwellness ... over time the way we think about illness keeps us stuck."
Clinical pharmacist McQuoid agrees the mind holds the key to unlocking us from pain.
"Pain is in the brain ... the answer is almost always not on the outside. People don't want that - they want an operation or a medication or injection, but they're going to be disappointed because none of those really help chronic pain.
"Once you come across people who can see things differently and change the relationship with their pain, that's a massive shift."
The Gender Pain Connection
Research on gender and pain the past 20 years shows women are more likely to live with chronic pain than men. Doctors say genetics, social status, exercise and information processing in the brain play a role in how we process pain. And for women, hormones, puberty, reproductive status and menstrual cycle also affect pain and perception.
The National Institutes of Health (US) cites many studies including one with 85,000 participants, showing occurrence of chronic pain is higher among females than males. Other studies from Europe and Australia also indicated chronic musculoskeletal pain is more common in females than males. Musculoskeletal pain includes back pain, whole body pain, fibromyalgia and osteoarthritis. As women age, they experience more compression fractures and vertebral changes, such as scoliosis, loss of bone mass and osteoarthritis than do men.
Studies find more women than men suffer abdominal pain. The NIH reports that there is approximately a 3-to-1 female-to-male ratio in the diagnosis of irritable bowel syndrome in the United States.
A review of more than 60 studies found women had more headaches and migraines than men. The one-year prevalence of migraine in the US was 18 per cent in women and 7 per cent in men.
Chronic Pelvic Pain (CPP) is defined as pelvic pain on most days for more than six months. It's estimated to affect 25 per cent of New Zealand women. Absent a physical injury, intimate partner violence has significant potential to contribute to chronic pelvic pain.
Sources: https://health.clevelandclinic.org/women-are-more-likely-to-have-chronic-pain-heres-why/
https://www.pelvicpain.org.au/pelvic-pain-in-women/
Treating End-of-Life Pain
Waipuna Hospice medical director Dr Murray Hunt says there are many parallels between treatment of chronic pain and treating pain from something like end-stage cancer.
Dr Hunt says people as a whole are living longer with significant medical illnesses, and hospice patients could be in care for months or longer than a year. Because of that, he says clinicians must be careful when prescribing medications, taking a patient's history and type of pain into account.
"We have a strong symptom-control focus that would involve utilising pain medications along with other interventions for pain."
Dr Hunt says cancer-related bone pain is sometimes treated with radiotherapy aimed at alleviating suffering. He believes opioids are prescribed responsibly, and say local providers don't feel hindered in their use.
"My team of hospice doctors, and I think it's true of the medical community as a whole, that I don't think we're prescribing with any concept or fear or Big Brother looking over our shoulders."
He says pain transcends the physical body. "We look at the context of psycho-social well-being and understanding the fullness of a patient as we hone into specific symptoms."
Where to get help
• Lifeline: 0800 543 354 (available 24/7) • Suicide Crisis Helpline: 0508 828 865 (0508 TAUTOKO) (available 24/7) • Youthline: 0800 376 633 • Kidsline: 0800 543 754 (available 24/7) • Whatsup: 0800 942 8787 (1pm to 11pm) • Depression helpline: 0800 111 757 (available 24/7) If it is an emergency and you feel like you or someone else is at risk, call 111.