In Her Head is a Herald project to help women get better medical care. Health reporter Emma Russell investigates what's wrong with our current system and talks to wāhine who have been made to feel their serious illness is a figment of their imagination or "just part of being a
In Her Head: Women's health - Mum Monique's traumatic births and failed operation

Subscribe to listen
Monique Cross remembers feeling like she wanted to die after two life-threatening births and a failed operation. Photo / Michael Cunningham
"I felt like I had failed as a parent and I was being punished for it," Cross told the Herald.
"I used to say to my husband 'wouldn't it be better if I was dead?'."
After years of suffering, Cross complained to the Health and Disability Commission (HDC) but the agency found no wrongdoing as they felt hospital staff had done all they could to provide her with appropriate care.
Cross decided to speak out as part of the Herald's In Her Head project because she wanted all mums to feel listened to and have their health concerns taken seriously.
Her story starts six years ago when she was pregnant with her first baby, Charlotte.
After initially being told she would need a caesarean because her placenta was covering the cervix, at 37 weeks her obstetrician advised that was no longer the case and she would instead have a natural birth.
Despite her feeling like something was still wrong, she said she was repeatedly ignored by her obstetrician and midwife.
Two weeks later, her waters broke and she had back-to-back contractions for 10 hours with very little progression. She pushed for a further two hours until the obstetrician had to intervene and "yank her baby out", she said.
"I started to bleed out, it was pretty horrendous. I remember doctors shouting and I was just naked on this bed out to it, with this obstetrician's hand up there and so many people around me. I had absolutely no dignity, it was like I was a piece of meat."
She said the worst part was when she woke up no one acknowledged the trauma she'd been through and she wasn't given any support.
"I just got given a new baby and that was it ... I started to think it was all in my head so I just tried to make everything perfect," Cross said.
Despite trying to be the perfect parent, she found herself becoming angry and resentful all the time.
Two years later, she fell pregnant with her second child, Hannah. She said she and her husband sought medical advice and begged for a planned caesarean because they didn't want to go through the same trauma as they had with Charlotte, and Cross was worried about her own mental health.
She said she was so worried she would bleed out again that her GP sent her to the hospital to see an obstetrician.
"[The obstetrician] said there was a one in a million chance that would happen again and I was being ridiculous," Cross said.
The obstetrician denied this, saying haemorrhage recurrence was common, which was why he recommended a hospital birth with "special precautions".
There was no record of what was said in the consultation so HDC was not able to reach a finding on that part of Cross' complaint.
An independent obstetrician told HDC the decision not to offer a planned caesarean was justified as it would not have prevented her from bleeding out and in fact could have made it worse. Cross said she was never told this at the time and if she had known, it would have helped her cope.
Cross ended up bleeding out four litres of blood after giving birth to Hannah.
"I was again rushed into surgery and had a balloon insertion because they couldn't stop the bleeding and I had to be resuscitated," Cross said.
A Bakri balloon is used in the management of excessive bleeding after childbirth (postpartum haemorrhage).
"The nurses said I was lucky to be alive," Cross said.
However, she didn't feel lucky because that trauma still haunts her today.
"I was depressed, I didn't sleep, I lost heaps of weight and I neglected myself. I wasn't coping and I just didn't want to be alive," Cross said.
The independent obstetrician told the HDC if an obstetric consultation had happened sooner it is possible Cross would not have lost so much blood. Overall however, she found the care appropriate.
"Although you experienced a significant postpartum bleed on this occasion too, the circumstances were different to the [first birth] and could not necessarily have been anticipated," the HDC report said.
Cross' nightmare didn't end there. After her two traumatic births, she opted to get a tubal ligation, an operation intended to stop her getting pregnant. However, two years after the surgery she fell pregnant again.
"I felt like I was being punished. I felt like a piece of s***, that I couldn't talk to anyone about it because no one could help me," Cross said.
While ACC said there was likely an error in the procedure, HDC accepted it as a "normal complication".
"Medical evidence showed that on the balance of probabilities there was likely an error in the procedure that saw a clip misplaced resulting in the pregnancy," ACC acting chief operating officer Gabrielle O'Connor said.
The Herald put this to HDC, which did not specifically say why findings differed. Instead, Health and Disability Commissioner Morag McDowell said the agency was confident the processes undertaken in the assessment of Cross' complaint were robust and fair.
A letter from Whangārei Hospital's chief medical officer Michael Roberts to an HDC complaints assessor said he also had conducted an inquiry and didn't feel the evidence supported Cross' allegation of neglect or any need for disciplinary action.
"There was clearly however an unfortunate series of normal complications and what she perceives as poor and dismissive communication for which I apologise sincerely," Roberts said.
Cross said the outcomes of her complaints were very hard to bear.
"I remember when I had got the email I was pretty broken and wished I hadn't complained at all, reinforcing the view that we should just grin and bear it," Cross said.
McDowell said the agency was sorry to hear Cross didn't feel the HDC decision brought her closure.
She was welcome to ask for a review of the assessment process and decision.
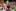
"But it is not appropriate for HDC to provide further comment on the specific details of the findings of our assessment process in a public forum, given the privacy of all those involved."
Around the same time, Cross received a letter from her obstetrician, which was not included in the HDC report, acknowledging the emotional and mental impact her traumatic births had on her.
"Throughout, you have needed practical support, which at times you did not feel you received and I regret this and have apologised that we have fallen short in that respect," he said.
Above all, Cross said she didn't feel her concerns were listened to and she hoped this would change.
To women who were struggling after a traumatic birth she said she would tell them "it's not your fault; every mum matters".
Monique's seven steps to overcoming trauma:
1. My GP asked if I was okay and realised I wasn't. I hadn't told anyone as I was so ashamed so she made me acknowledge my feelings and suggested I get some counselling. I'm very grateful for her recognition of my trauma. She validated it was really bad and I deserved to feel angry, and she actually said the words "it's not your fault". She also talked about the physical effects the trauma was having on my body and that made me tune into the things that were triggering me to feel bad, and the physical reactions I was having were acknowledged.
2. Through discussion with this GP and my counsellor I realised I had to change my thought patterns around myself as a mother and a person and acknowledge that my hatred towards myself was unwarranted and that I didn't need to continue to punish myself as I was doing through my actions. Slowly I started to practise gratitude and see bit by bit some of the good around me and gave myself some credit. I also worked on my self-talk and tried to think about talking to myself as I'd want someone to talk to my daughters. I did this with them too, and together we said good things about ourselves and each other that made us feel good.
3. Recognition of the role nutrition and exercise have on my mental well-being. I started looking at proper nutrition, getting in some exercise every day and also having enough sleep - this was a game-changer. Living on two hours of sleep, caffeine and sugar was really self-destructive, but again it was a form of punishment.
4. I also had some time to myself to do things I enjoyed, and time with my partner without the girls (thanks to my mum) and tried not to feel guilty or ashamed of asking for it. Then I started to feel more like myself. I started to talk about my feelings more and to show my girls it's okay to be sad, mad, scared etc and doing positive things to try and change those feelings. This also meant taking a step back from my career for a bit, which was high pressure, making me realise the trauma affected my ability to cope with stress. I couldn't cope that well and I needed to have some downtime. Financially it was tough, but we just had to make a change.
5. Being everything to everyone isn't possible and we all need to know that it's okay to ask for help, and that is not failure or being useless, it is just being human. I try to model resilience and respect for myself and my body now too, so that my girls know this is okay, especially around medical issues. We should have the right to be listened to. If I'd spoken up and been listened to by the specialists, I may never have been through what I did.
6. I also had to let go of needing a physical apology, as it wasn't going to change what happened. Northland DHB is a very big machine and the avenues I tried to get some answers all ended up being more hurtful than helpful, so I just had to let it go.
7. Speaking up about the changes that could be made make a difference, especially to women who think we need to do it all, do it perfectly and smile while we do it. I was really good at looking okay, even though I really wasn't. It's made me feel uncomfortable speaking out, but that's a small part of being brave and slightly vulnerable. I am excited to hopefully be part of this much-needed change.
Where to get help:
• Lifeline: 0800 543 354 (available 24/7)
• Suicide Crisis Helpline: 0508 828 865 (0508 TAUTOKO) (available 24/7)
• Youth services: (06) 3555 906
• Youthline: 0800 376 633
• Kidsline: 0800 543 754 (available 24/7)
• Whatsup: 0800 942 8787 (1pm to 11pm)
• Depression helpline: 0800 111 757 (available 24/7)
• Rainbow Youth: (09) 376 4155
• Helpline: 1737
If it is an emergency and you feel like you or someone else is at risk, call 111.
Follow women's personal stories of poor healthcare in our interactive grid below. Click on a face to go to the full story.