When Calie Coppinger received the call no one wants to receive, she had no idea she and her family would soon be faced with two major decisions. Now, as Manawatū Guardian editor Merania Karauria discovers, Calie's story, and that of her late husband Steve, is one more New Zealanders need to know, and talk, about.
Calie Coppinger had never thought about organ donation.
That was until her husband Steve died of a massive brain bleed.
Calie says her urologist surgeon husband was a healthy and active man.
When she arrived at Palmerston North Hospital after being called to say Steve had collapsed, she never expected she would soon be faced with the donor option.
Steve was clearly in pain, holding his head and saying "BP", but Calie, despite having a medical background, was unsure if BP meant more than blood pressure.
The hospital staff swung into action and Steve was taken for an MRI scan.
The scan showed bleeds throughout his brain.
Calie understood that to revive Steve would have been, what she heard someone utter under their breath, barbaric.
"I knew what I heard was true. Steve would have hated to have been revived."
She was faced with a heartbreaking decision.
Her husband, a vibrant and dynamic man who lived life to the full, who loved his life; who was adventurous and wanted to continue to explore the world; who loved diving in the depths and photographing the sea creatures that lived there; who captured the joy on people's faces and published them in a book.
Her husband, who had come to New Zealand with Calie and their three sons, loved what he discovered and settled here and never wanted to return to his native Canada.
Her husband would never again be the surgeon who helped people to live a better life, be the doting father to his sons, and the husband with whom she'd shared many happy years.
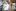
In a moment, Calie knew what she had to do for her husband, who was on a ventilator.
Then, one of Steve's colleagues asked Calie if she had ever thought about organ donation.
Those who knew and worked with Steve raised the suggestion because it was something they knew he would agree to.
"Giving the gift of life," says Calie, though there was no space to think so rationally while she waited for their three sons who were on their way to Palmerston North from Wellington.
"[Son] Brooke scooped up Charles and Dominick and they were here in two hours."
The family was taken into a room.
The family sat around a table with charge nurse Sue, Dr Chachi, friends Gill and Steve Welch, and Steve's photographer friend David Lupton.
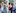
Calie said she asked each of their sons what they thought about donating their father's organs. Time was of the essence.
Following his death Steve was on a ventilator while the family considered donating his organs.
Calie and the boys had questions to ask the surgical staff.
Even though Steve was on a ventilator and clinically brain dead, would he be given an anaesthetic? Yes, was the response.
The boys wanted to know if they would get to meet the people who received their father's organs.
No, they were told.
The family agreed, and Steve's corneas, a kidney each to two different people, his liver and skin, were donated.
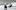
Organ Donation New Zealand (ODNZ) donor co-ordinators manage all aspects of the organ retrieval including co-ordinating the retrieval teams, chartering planes, flying with the retrieval teams to the donor hospital and carefully packing and bringing the organs back to Auckland for transplant.
ODNZ says there are up to two retrieval teams that fly to the donor hospital and each team consists of a surgeon, an anaesthetist and a nurse, plus the ODNZ donor co-ordinator.
"At the same time as the donor co-ordinator is organising the retrieval, the transplant teams will be contacting recipients and arranging for them to travel to Auckland for their transplant operation."
The next morning the team arrived into Palmerston and within 48 hours Calie was called to say a kidney transplant was functioning successfully.

Months onward, Calie says the family feel happy to know Steve's organs gave someone the gift of life.
ODNZ says the biggest message they would like to get across is to encourage people to "talk about organ donation".
"The most important thing that we all can do is have a conversation, talk about organ donation with our families, whānau, or those people closest to us.
"So that if we are ever in a position where donation is possible, they will know what to do."
ODNZ clinical director Stephen Streat says organ donation is a measured and respectful process.
"We support the hospital staff in ensuring families have the opportunity and time to consider donation, whenever it is a possibility."
Organ Donation New Zealand
Organ donation is a relatively rare event because donation is only possible when someone is in an Intensive Care Unit (ICU), on a ventilator (breathing machine) and usually has a devastating brain injury.
Fewer than 1 per cent of all deaths in NZ occur this way.
However tissue donation is possible in most circumstances when people die (at home, in a hospice, on a hospital ward).
ODNZ responded in writing to questions asked by the Manawatū Guardian about organ donation in New Zealand:
Manawatū Guardian: Are a lot of people waiting for organs?
Yes we need more donors. There are on average 550 people waiting for organs at any one time. The longest and largest transplant waiting list is for kidneys.
What organs are required?
Heart, lungs, liver, kidneys and pancreas. However there is also a need for body tissue – eye tissue to repair eye damage and restore sight, heart valves to help babies with genetic heart conditions and skin to repair severe burns.
Is organ donating in New Zealand accepted by the community at large?
Fifty-three per cent of New Zealanders have ticked 'yes' to being a donor on their driver licence. However it's really important to remember that ticking 'donor' on your driver licence is an indication of your interest only. It is not a donation register or legally binding decision.
The most important thing you can do is to tell your family, talk to them about your decision and let them know what you would want to happen.
If you are in a situation where donation is possible doctors will ask your family or whānau if they know your wishes regarding donation and what organs and tissues you would want to donate.
What are the barriers, if any?
Many people say that families are a barrier to organ donation. This is not usually the case.
Where there has been a conversation about donation, most family members follow through on what the person wanted.
It's where there has never been a conversation about donation that families can struggle to make a decision about organ and tissue donation at such a difficult time.
Organ donation - the process
Brain death assessment
Two separate sets of brain death assessments are carried out by two different doctors to confirm that the patient's brain has died.
The time when the second brain death assessment has been completed is the time of death of that person.
This is the time that will be recorded on the death certificate.
Discussion about donation
Some time after the family has been told that their loved one has died, the intensive care doctor will discuss donation with the family.
After the family has been given information about organ and tissue donation and what is involved, they will be given time to make a decision.
If the family agrees to donation, a written consent form will be obtained for the organs and tissues they are comfortable with donating.
Donor co-ordination
Following a family's agreement to donation, the donor co-ordinator for Organ Donation New Zealand is contacted.
The donor co-ordinator obtains the medical information about the patient who is donating, liaises with the transplant teams and organises the organ retrieval operation.
Organ donation operation
The surgical teams travel to the hospital where the patient is being cared for.
The patient is transferred to the operating room while the ventilator (breathing machine) continues to supply oxygen to the organs until they are surgically removed.
The operation is carried out as it would be for any other surgical operation, including the stitching and dressing of the incision(s) at the end of the operation.
After the donation
The family may spend time with their loved one if they wish, following the donation.
Organ and tissue donation will not interfere with the funeral arrangements, including an open coffin, or having their loved one at home.
The health professionals involved in the donation operation ensure that the patient is treated with care and respect at all times.
Support for donor families
The donor co-ordinator provides information and support to the family of the donor and will often meet the family prior to the donation.
The family receives a letter of thanks that includes general information about the recipients - for example -"the heart was transplanted to a man in his 40s and the liver recipient is a woman in her 20s".
The family also receives a booklet providing information about brain death, organ donation, transplantation and the grief process.
Communication is continued for many months or years for some families.
Finding out about the progress of recipients
Donor families can contact the donor coordinator at any time to find out the progress of the recipients.
For some families, this is not something they choose to do, but for others it is important and they request this information for many years after the death of their loved one.
Although confidentiality is maintained, recipients are able to write an anonymous letter of thanks to the donor family.
These letters are forwarded through Organ Donation New Zealand to the family of the donor, if they wish to receive them.
Donor families are also able to write to recipients and these letters are handled in the same way.
The follow-up for donor families has increased over the years.
ODNZ says it is aware that there will be families who donated in the past but received little or no acknowledgement or information.
If you would like to receive information and support now or at any time in the future, please contact Organ Donation New Zealand on 0800 4 DONOR (0800 436 667) or here.
Why I'm a donor

Manawatū Guardian editor Merania Karauria recounts her own heartbreaking story.
Richie was aged three when he complained of a sore back.
However, the doctor sent Richie home saying it was his mother who was over-dramatising his complaint.
But the back pain became more severe and Richie was now crying a lot.
Finally the diagnosis came back that Richie had something wrong with his liver.
It was cancer.
After tests and treatment Richie was put on the waiting list for a liver transplant.
However, transplants were carried out in Brisbane.
It was an agonising wait for Richie's family and my 17-year old son who was Richie's "godbrother".
Finally the call came that Richie could go to Brisbane for his new liver. We were all so hopeful.
But it was Christmas Eve when Richie's father called us to say, although the transplant was successful, the cancer had spread. Richie had only weeks to live.
The family returned and we visited.
Richie and I went window shopping.
He was so happy, but I was heartbroken, especially when he asked me if I was coming to his fifth birthday.
"Of course," I said. Instead I went to his funeral.
Richie would be 22 if he had lived.
When I renewed my licence last year, there's a special note that reads "Donor".
Donor recipients on how their lives have changed
• "I like how my new liver takes care of me and I'm not sick anymore."
Elliott, liver recipient (age 6)
• "In the days after my transplant I was overwhelmed at the enormity of what had happened.
"Not just that my life had changed forever, but that my life had changed because a life had ended.
"The impact of this has been profound; I am changed forever in ways I can't explain.
"There are no words to explain the gratitude I have for my life and the experiences I will have because of this second chance."
Heidi, heart transplant recipient
• "I am now 17 years into my transplant journey, living each and every day with gratitude and heartwarming love for my gift.
"As a transplant recipient I am focused on making my life count and honouring my donor and those who have changed my life and the lives of so many individuals fortunate enough to receive transplants.
"Life is truly precious."
Anna, kidney transplant recipient
• "Where I am today is possible due to the 44 years of world class medical care I have received (too many teams to list) and, of course, the brave and generous decision of my donor's family to allow their loved one to become a donor.
"Thanks to these exceptional people, I am now once again living a relatively normal life.
"Because sometimes just a bit of normal can be exceptional!"
Stefan, heart transplant recipient
Annual services
Each year in April or May, a service is held in Auckland in recognition of those who have donated organs and given the gift of life to others.
A second service is also held on alternate years in Wellington and Christchurch.
Donor families, recipients and their families, as well as health professionals are invited to attend these services.

