Hope is a 41-year old, single mother of four. She's also a diabetic with failing kidneys, chronic vomiting and pain, and last month, for the first time in her life, she smoked cannabis.
She bought two foils from a friend for $40 and now she follows a new evening ritual. After her youngest kids - aged 8 and 9 - are in bed, she takes her rolling papers and carefully closes the garage door. Then she sits outside and smokes.
It helps the pain, she says, which comes on strong in the evening hours. It helps suppress the nausea that otherwise haunts her, and if she's lucky, it sometimes helps to stir her appetite.
The loose cannabis flower isn't Hope's first choice (she asked to have her surname withheld because it's still an illegal drug). She'd prefer to take the cannabidiol drops, which are not psychoactive, and which her GP prescribed for her over three weeks ago. But no medicinal cannabis products are subsidised by Pharmac, and there's no way her Supported Living Payment from Work and Income will stretch to cover the $464 that prescription will cost to fill.
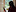
Hope applied to Work and Income to cover the cost separately. But she said that application was recently declined, despite supporting letters from her GP, dietician, and the social worker on the dialysis unit at Middlemore Hospital, which she attends three times a week, four hours at a time, for hemodialysis.
"I'm on OxyNorm at home, that's an opioid. They give me fentanyl at the hospital. They give me the anti-nausea drugs they give to cancer patients, only I'm not a cancer patient. But for this cannabis oil they want all these supporting letters. I get those and now they turn around and want me to go back to the doctor and have the doctor tell them everything about the other drugs and how they won't work," Hope said.
Hope's desperate measure is the kind the Government suggested would end once New Zealand introduced a legal and broadened medicinal cannabis regime.
READ MORE:
Premium - New Zealand's medicinal cannabis supply in jeopardy
In late 2018 it passed legislation that paved the way for the new system and last April new regulations were finalised that were supposed to achieve much broader patient access.
However, no domestically produced medical cannabis is yet on the market. And the new rules are so strict that, 10 months after their introduction, no products have yet been approved for import by the Ministry of Health.
Importers now warn that when old, stop-gap importing rules expire at the end of March, the legal cannabis supply in New Zealand will collapse. Three of the country's five main importers - Medleaf Therapeutics, Nubu Pharmaceuticals and Eqalis Pharmaceuticals -confirmed they do not expect their products to meet approval under the new rules by the deadline, and anticipate they will be forced out of the market, at least for a time.
Fewer competitors threaten even fewer legal choices for patients like Hope, and even higher prices.
