Patients battling advanced breast cancer could be spared needless treatments with a clever DNA-based technique that uses personalised blood tests to closely monitor tumours.
With fresh funding from the New Zealand Breast Cancer Foundation (NZBCF), leading researcher Professor Parry Guilford will take an approach that's already delivered promising results in his Otago University lab to a wider trial involving 50 patients.
Today, fighting advanced breast cancer typically involves multiple drug treatments and expensive, infrequent scans to find out if certain drugs are working.
Unlike CT scans, which can only be performed a limited number of times and often aren't sensitive enough to detect changes in a person's cancer, the simple test being investigated could offer a much more detailed picture and be used as many times as needed.
"It could provide faster feedback to patients and doctors, so that minimal time is wasted on treatments that aren't working," said Guilford, who has so far studied the method's potential in colon cancer treatment.
The new $130,000 study draws on circulating tumour DNA (ctDNA), or the traces of DNA that tumours leave as signatures in the blood stream.
By comparing the DNA results of blood tests with assays developed from samples of the patient's removed tumour, clinicians could quickly detect changes.
"These ctDNA markers are tightly linked to the tumour, so if you can see them rising, you know the tumour is growing, and if they're falling, the tumour is shrinking," he said.
"So far, it seems extremely sensitive: our methods can pick up exceptionally low levels of tumour DNA in the blood, so we are very confident that we have the technology to make it work clinically."
With further research, he hoped the tests might ultimately be used to pin-point the precise mutations driving cancer growth in different patients.
Other blood-based tests, sometimes vulnerable to rogue spikes causing misleading results, could leave clincians with a messy picture and a weaker grasp of the cancer's evolution.
But the ctDNA approach could detect just what type of subclone had grown from a tumour mass and enable the right drug to be pitched against it.
Globally, there was a growing focus on ctDNA-based testing as the speed of DNA sequencing technology improved.
Guilford felt it was important for the method to be adapted by the New Zealand healthcare system as quickly as possible.
"We have to do it with our own hands - we can't just sit back and wait for the technology to be handed over by the British or the Americans in 10 years' time."
In New Zealand, it's estimated there are between 1000 and 2000 women alive with advanced breast cancer.
The NZBCF saw the study and others supported by its latest $340,000 funding round as something that could make a big difference for Kiwis in the short-term, and another step toward its goal of zero deaths from breast cancer.
"With this funding round, we insisted that applicants should show how patients might benefit from the study sooner rather than later, plus how they plan to build on previous studies, whether in breast cancer or other areas," chief executive Evangelia Henderson said.
"We owe it to patients and to our donors to get real-world benefit from research whenever possible, and to maximise the investment that we and other charities have made over the years."
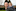
Tauranga mum lost to cancer would have backed study
Near Mt Maunganui beach, there's a table donated in memory of Jen Peeters.
It's the special place where Richard Peeters and four-year-old William go to be with their wife and mum.
If there's another legacy Peeters would like Jen to have, it would be shining the spotlight on faster and more effective treatments for cancer, which took her life two years ago this month.
She was diagnosed with breast cancer while pregnant with William in 2011, forcing her undergo chemotherapy and a mastectomy.
After radiotherapy and more chemotherapy treatment, she was told she was in remission.
But the cancer returned shortly after she underwent reconstructive surgery, eventually spreading to other parts of her body.
Several drugs were used to combat the cancer, but none were able to save her; she died in August 2014, aged 39.

"The treatment involved is more of a blanket situation, but not every drug that's on the market suits the type of cancer the patient has got," Peeters said.
"So the trouble is you have to do a full round of chemo to establish whether it's worked or not."
When it came to a disease as threatening as cancer, timing was everything: and administering a drug that didn't work was just stealing the time of one that could.
"When we went in there, we said throw everything at us: she had everything to live for, being pregnant, and we just told the doctor we'll go with what you tell us to do.
"But you go into these things blind, really. You hope for the best, but it's not until you see the oncologist that you learn if it's worked or if it hasn't.
"And when you're put in that life-threatening situation, you want to know everything, straight away."
It's why Jen couldn't have been more in support of potentially revolutionary studies like that being led by Otago University's Professor Parry Guilford.
"Anything that could eliminate cancer, or aid in its elimination, has got to be a good thing... and she was all for that."
Other funded studies
Targeting hard-to-treat cancers: Researchers are exploring the potential of a recently-discovered antibody that targets a protein called SHON, commonly found in treatment-resistant breast tumours.
Auckland University of Technology's Dr Dongxu Liu and his team will now test whether this antibody will stop tumour growth in human cancer cells, with an ultimate aim of reaching clinical trials involving breast cancer patients.
Sparing chemo side-effects: Auckland University's Associate Professor Nuala Helsby and colleagues will pilot a test to identify patients who will suffer severe side-effects of chemotherapy drug capecitabine, typically the first treatment women with advanced breast cancer receive.
Between 5 and 10 per cent of patients experience dangerous side-effects, including blistering or severe pain in the hands and feet, diarrhoea, and even cause death.
Those who suffer them are deficient in the liver enzyme which removes the drug, along with thymine, from the bloodstream.
The researchers aim to give breast cancer patients thymine, measure how much is removed from the bloodstream and use that data to figure out whether they're deficient in this important enzyme.
A genetic test for Kadcyla: A team led by Dr Francis Hunter of Auckland University will develop a genetic test that will determine which HER2+ breast cancer patients will benefit from the new drug Kadcyla.
Approved for use but not yet publicly funded, the drug has had promising clinical trial results for patients with advanced HER2+ breast cancer, with tumours shrinking in 44 per cent of cases and patients surviving seven months longer.
The new test will identify genes that control a patient's response to Kadcyla, telling doctors who will benefit and who won't - something vital for patients with incurable conditions and little time to waste on drugs that won't help them.

